Special Qualifying Events
Eligible individuals have additional opportunities to enroll in coverage if they meet the conditions of a special qualifying event. Information provided below explains what triggers such opportunities, who may enroll, deadlines for enrolling, the documentation that is required to support the application and coverage effective dates. The medical plan documents are the legal publications that define eligibility, enrollment, benefits and administrative rules of the plan. You can find the medical plan documents on the publications page of the Partners for Health website.
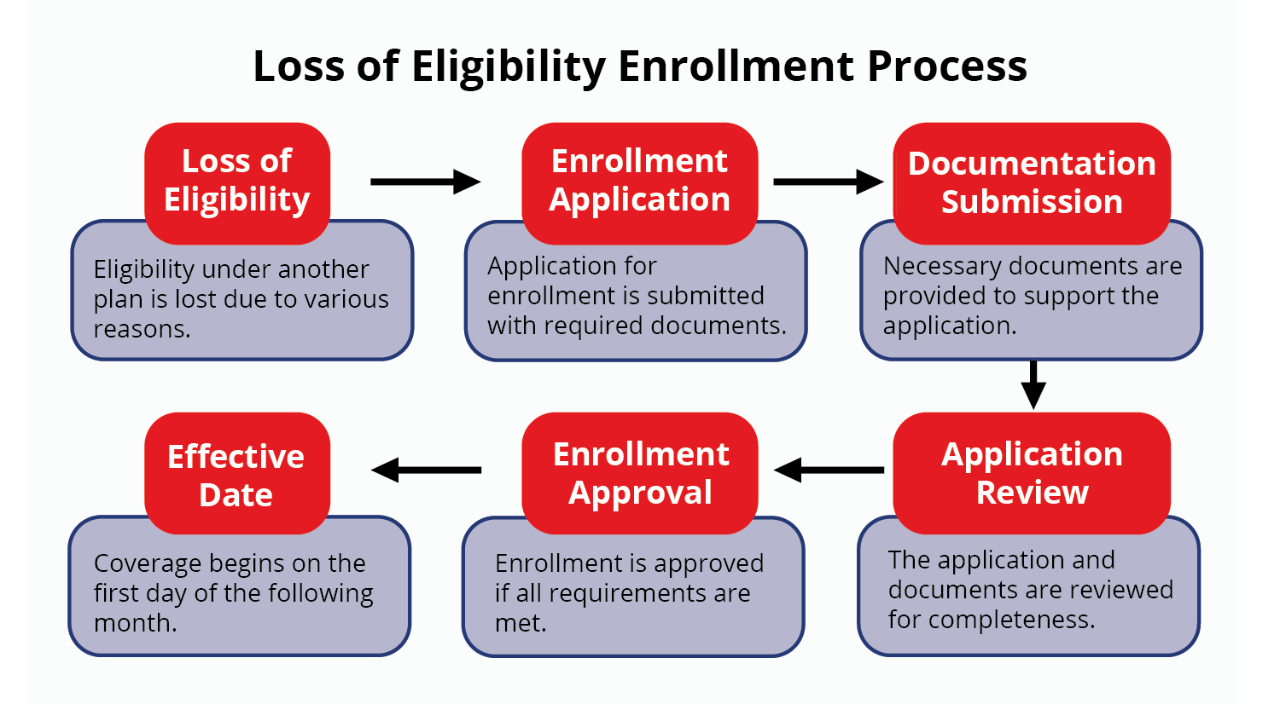
Loss of Eligibility: Eligibility under another plan is lost due to various reasons.
Enrollment Application: Application for enrollment is submitted with required documents.
Documentation Submission: Necessary documents are provided to support the application.
Application Review: The application and documents are reviewed for completeness.
Enrollment Approval: Enrollment is approved if all requirements are met.
Effective Date: Coverage begins on the first day of the following month.
Loss of Eligibility
What happens if there’s a loss of eligibility under another group insurance plan for any reason (including divorce, death of spouse or involuntary loss of other government coverage)?
- Only the employee and any dependents who have lost or will lose eligibility may enroll. Individuals who lose other coverage may only enroll in the types of coverage lost (medical for medical, dental for dental or vision for vision). A voluntary action that results in loss of coverage is NOT a qualifying event, including a voluntary cancellation of coverage, a cancellation of coverage for not paying premiums, or electing to cancel, waive or decline coverage during another plan’s enrollment period.
- If adding dependents to existing health insurance coverage, you and your dependents may transfer to a different carrier or health care option, if eligible.
Deadline: The ABC or BA must receive the application for enrollment with the required documentation within 60 days of the loss of eligibility.
Effective date: The first day of the month after the ABC or BA receives a completed application with documentation.
Documentation required: Written documentation from an employer, former employer, insurance company or former insurance company on company letterhead that lists:
- Names of covered participants.
- Dates of coverage, including your coverage at the time coverage in this plan was declined.
- Types of coverage (medical, dental, vision).
- Each participant who lost eligibility for coverage.
- The date of loss of eligibility to continue coverage.
- The reason why eligibility for coverage was lost.
Acquisition of a New Dependent
What can occur when there’s an acquisition of a new spouse or stepchild by marriage?
- The employee may enroll in employee-only or family coverage.
- The employee may add new dependents and any eligible dependents who were not enrolled when initially eligible and are still eligible.
- If adding dependents to existing health insurance coverage, you and your dependents may transfer to a different carrier or healthcare option, if eligible.
- Head of Contract and eligible dependents may enroll in dental and vision coverage if the requirements stated in the dental or vision certificates of coverage are met.
Deadline: The ABC or BA must receive the application for enrollment with the required documentation* within 60 days of the date of acquisition (the date of acquisition is the date of the marriage or the date of the placement order).
Effective date: The first day of the month after the ABC or BA receives a completed application with documentation.
*Documentation required:
- Birth Certificate (will accept mother’s copy for newborn)
- Marriage Certificate
- Secondary document to validate marriage from list below:
- Bank Statement issued within the last six months with both names; or
- Mortgage Statement issued within the last six months with both names; or
- Residential Lease Agreement within the current terms with both names; or
- Credit Card Statement issued within the last six months with both names; or
- Property Tax Statement issued within the last 12 months with both names; or
- The first page of most recent Federal Tax Return filed showing “married filing jointly” or “married filing separately” with the name of the spouse provided
What can occur when there’s an acquisition of a new dependent by order of guardianship?
- Employee-only coverage is not permitted.
- All change requests due to an Order of Guardianship must arise out of and correspond with the terms of the guardianship order.
- HOC and eligible dependents may enroll in dental and vision coverage if the requirements stated in the dental or vision certificates of coverage are met.
Deadline: The same as when acquiring a new spouse or stepchild by marriage – within 60 days of the date of acquisition.
Effective date: Also, the same as when acquiring a new spouse or stepchild by marriage – the first day of the month after the ABC or BA receives a completed application with documentation.
Documentation required:
- Birth Certificate (will accept mother’s copy for newborn)
- Order of Guardianship requiring financial support and provision of insurance coverage, which sets out the date of the guardianship period.
- Certification of Eligibility for Dependents placed with Head of Contract by Valid Placement Order or Dependent Eligibility Certification for Dependent with Expired Placement Order.
When a new dependent is acquired by birth, adoption or placement for adoption, enrollment should be completed and submitted to the ABC or BA within 30 days to ensure the earliest possible effective date.
What can occur when there’s an acquisition by birth, adoption or placement for adoption?
- The employee may enroll in employee-only or family coverage.
- The employee may add the new dependent and any other eligible dependents who were not enrolled when initially eligible and are otherwise still eligible.
- If dependents are added to existing health insurance coverage, the HOC and eligible dependents may transfer to a different carrier or health care option, if eligible.
- The HOC and eligible dependents may additionally enroll in dental and vision coverage if the requirements stated in the dental or vision certificates of coverage are met (no retroactive coverage is available for dental and vision).
Deadline: The ABC or BA must receive the application for enrollment with required documentation* within 30 days of the birth, adoption or placement of adoption for retroactive health insurance coverage.
Effective date: The date of birth, adoption, or placement for adoption. Other coverage (dental/vision) will begin the first day of the month following the enrollment request. An application with required documentation* that is received by the ABC or BA 31 to 60 days after the birth, adoption or placement for adoption will result in an effective date of the first day of the following month.
*Documentation required:
- Birth Certificate (will accept mother’s copy for newborn).
- Final Order of Adoption or Order of Custody in anticipation of adoption.
Special Qualifying Event Examples
A couple gets married on June 15.
- Enrollment is submitted to the ABC/BA on June 25 (within 30 days of marriage): All coverage will begin July 1, the first day of the month following submission of the completed application.
- Enrollment is submitted to the ABC/BA on Aug. 14 (within 31-60 days): All coverage will begin Sept. 1, the first day of the month following submission of a completed application.
- Enrollment is submitted to the ABC/BA after 60 days on Aug. 15 (61 days after the event): This will exceed the 60-day enrollment period, and the request will be denied.
A son or daughter is acquired via birth, adoption or placement for adoption on June 15.
- Enrollment is submitted to the ABC/BA on June 25 (within 30 days): Health insurance will be retroactive to June 15, the date of birth. All other coverage (dental/vision) will begin July 1, the first day of the month following submission of a completed application.
- Enrollment is submitted to the ABC/BA on July 15 (within 31-60 days): All coverage will begin Aug. 1, the first day of the month following submission of a completed application.
- Enrollment is submitted to the ABC/BA on Aug. 14 (60 days after the birth/adoption/placement of adoption): All coverage will begin Sept. 1, the first day of the month following submission of the completed application.
- Enrollment is submitted to the ABC/BA after 60 days on Aug. 15 (61 days after the event): This will exceed the 60-day enrollment period, and the request will be denied.
New Eligibility for Premium Subsidy
An employee and any dependents newly eligible for a premium subsidy through a Children's Health Insurance Program or Medicaid program may enroll in health insurance coverage midyear.
- The ABC or BA must receive the application for enrollment with documentation within 60 days of the new eligibility.

Important Reminders
- If adding dependents to existing health coverage, the HOC and eligible dependents can switch to a different carrier or health care option.
- Premiums are not prorated. If approved, you must pay the premium for the entire month in which the effective date occurs.
- Eligible persons may also enroll in dental and vision coverage if they meet the requirements stated in the dental or vision certificates of coverage.
- A request to enroll due to loss of eligibility under another group insurance plan must be submitted to and received by the ABC/BA within 60 days of the loss of eligibility.
- A request to enroll due to acquiring a new dependent must be submitted to and received by the ABC/BA within 60 days of the acquisition date. Enrollment should be completed and submitted to the ABC or BA within 30 days to ensure the earliest possible effective date.