REWARD Toolkit
Jump to Section: About | R.E.W.A.R.D. Program | Before an Injury Occurs | After an Injury Occurs | Transitional: Return to Work | Next Step Program | Support/Recognition for REWARD Employers | Appendix
Appendix Tools
- REWARD Tool #1 - ROI Calculator
- REWARD Tool #1A - RTW Difference in WC Benefits
- REWARD Tool #2 - Sample Return to Work Policy
- REWARD Tool #7 - Information Exchange Between the Employer and the Authorized Treating Physician (ATP)
- REWARD Tool #8 - Transitional Work Letter to Physician, Placement Offer (Template), and Job Description/Analysis - Physical Demands Form
About the Tennessee Bureau of Workers’ Compensation REWARD Toolkit
In the fall of 2019, the Bureau began to work on a program with dual goals: to reduce both the time that injured employees lost to work-related injuries and illnesses, and the number of employees who never returned to the workforce. This project was consistent with the Bureau’s mission – “to fulfill the promise of workers’ compensation today and tomorrow,” which means to minimize the impact of job-related injuries and illnesses on employees and employers.
People need to work for reasons beside earning an income; they need to connect with other people with whom they have common work interests. They need to have purpose in their lives and going to work and accomplishing something gives them purpose. They want the security that comes from knowing that they have a job and a future income. And, certainly they need work to provide salaries for the material essentials of living and, hopefully, some of the wants, too. It’s myth that going on disability is a desirable outcome for employees.
To get people back to work sooner and more often, the Bureau began developing the REWARD program. The project started out with a small number of people on the Bureau staff and then grew into a task force, as interested employers, medical professionals, and insurance companies shared their time and expertise to focus on a broad spectrum of issues that affect whether employees with workers’ compensation injuries can return to work sooner.
The program includes:
- This REWARD Toolkit;
- Certified Physician Program;
- Resources and networking opportunities for employers who are interested in a return-to-work program; and,
- Yearly Honor Roll to recognize employers who have outstanding return-to-work programs.
These program elements are based on the belief that all parties involved in workers’ compensation must work together to achieve the best outcomes for employees and employers. Claire Muselman, 2020 winner of the Magna Comp Laude award for her career contributions to the workers’ compensation industry and Workers’ Recovery Unit Director for Continental Western Group, a Berkley Company, expressed it well:
Workers’ Compensation is a team approach bringing employers, adjusters, and injured workers together for a collective purpose. Back to work, back to LIFE should be the motto of all parties involved in the workers’ compensation process, as we work together to help someone during an unfortunate circumstance. When the collective group works as a team, great things can happen!
This toolkit would not have been possible without the following people who are part of the REWARD Task Force. They are:
Stakeholder Representatives
- Erin Bartholomew, Claims Team Manager II, Liberty Mutual Insurance Co.
- Terry Horn, RN, CCM, CHC, Vanderbilt Corporate Health, Corporate Health & Wellness, Executive Health
- Nancy Kelly, RN, MSN, COHN-S/CM, Nurse Case Manager & OSHA, Averitt Express
- Dr. Les Kertay, Ph.D., ABPP
- Nanette Ray, RN, Regional Nurse Case Manager, U.S. Health and Wellbeing, Mars, Inc.
- Diane Stinnett, RN, BSN, COHN, U.S. Health and Wellbeing, Mars, Inc.
- Shirley Vincent, RN, CCM, Guardian Medical Consulting
- Michelle McBroom Weiss, MA, CRC, CCM, NCC, MSCC, ABVE/D, IPEC, Vocational Consultant
And from the Bureau of Workers’ Compensation
- Jay Blaisdell, Coordinator, TN BWC
- Suzy Douglas, RN, Assistant Administrator, TN BWC
- Jeff Francis, Former Assistant Administrator, TN BWC
- Brian Holmes, Director, MOST, TN BWC
- Abbie Hudgens, Former Administrator (2011 - 2022), TN BWC
- Dr. Robert Snyder, Medical Director, TN BWC
- Dr. James Talmage, Assistant Medical Director, TN Bureau of Workers’ Compensation
R.E.W.A.R.D. Program: Return Employees to Work And Reduce Disabilities
When an Employee is Injured at Work, Everyone Loses.
Work-related accidents have negative consequences. Employees may be left with a permanent physical impairment as well as anxiety and depression, a lost sense of personal worth, and a fear of losing their
jobs. They may be taken off work by their doctors for an extended period or permanently.
Employers are negatively impacted, too. A 2018 National Council on Compensation Insurance (NCCI) study reported that work injuries cost employers an average of $41,000 per claim.1 Employers also have indirect costs for overtime, training temporary and/or replacement employees, administrative costs, and lost productivity that are not included in the average cost of a claim. These indirect costs can be higher than the direct costs.
What if there was a way to lessen the impact for both employers and employees? There is. It is the Tennessee Bureau of Workers’ Compensation REWARD Program. When an injured employee returns to work, everyone WINS.
A “Win-Win”
By offering a ‘return-to-work’ plan, our associates know that they can focus on recovery while having the support and security of their workplace. Temporary, modified work provides a transitional pathway to full-duty work. By participating in the REWARD program, employers have the support and assistance from the State of Tennessee to provide an RTW program to their employees. We call this return-to-work process a win-win for our associates and for our company.
- Nancy Kelly, RN, MSN, COHN-S/CM Nurse Case Manager & OSHA, Averitt Express
How Can the REWARD Program Help?
The best way to reduce the effect of injuries is to reduce accidents, of course. But accidents still occur, even when employers have done their best to prevent them. The good news is, what happens after an accident can make a real difference in the life of the injured worker and on the bottom line of the employer.
The REWARD Program provides resources to improve the recovery process and return employees to work within their physical restrictions as early as possible, which benefits employers and employees.
Employers benefit when they help injured workers return to work sooner, even if the employer must make accommodations or find “light-duty” opportunities. This will lower claims costs and workers’ comp premiums. Overall productivity returns to normal quicker when skilled and qualified employees perform the work instead of temporary or fill-in employees.
Tool #1 in the Appendix is a calculator for employers to estimate how much a REWARD Program can save them.
Employees benefit psychologically and socially by working. Lifespans are lengthened and improved when people work. A primary goal of workers’ compensation is to return injured employees to their pre-injury status. This means providing them timely access to appropriate medical care at no cost and wage replacement benefits if they are taken off work by the treating physician for more than seven days. It also means returning them to work whenever possible.
Collaborate on Solutions
The human, social, and economic harm caused by unnecessary work disability is real, significant, and preventable. We need to build an environment and system that not only engages the employee in their recovery and RTW but also helps them to decide to RTW. The employer and employee have the most power to facilitate a successful RTW when they collaborate on solutions to address concerns and develop a clear path to return to work. Only then can a provider have a clear understanding of what their patient is returning to and get behind and support the transition back.
– Jason Parker, CEO/Founder/Work Disability Consultant, Centrix Disability Management Services Inc.
What Does the REWARD Program Offer Employers?
Employers participating in the REWARD Program can expect many benefits. For starters, the program lowers workers’ comp costs due to shortened periods of workers’ compensation disability benefit payments and reduced medical costs. Wages are paid for actual work performed rather than workers’ comp disability benefits. Productivity improves by allowing employers to retain the subject-matter expertise and experience of injured workers, while reducing the time other non-injured employees must “fill-in” for injured workers. In addition, employers can avoid the costs for recruiting and training permanent replacements for injured workers who never return to work.
What Does the REWARD Program Offer Employees?
Employees who work for employers participating in the REWARD Program reap benefits as well, such as increased job security and a quicker return to their regular wages and their “normal” standard of living. It will also boost their physical and psychological health by being gainfully employed, retaining or improving their job skills, and focusing on what they can do instead of what they can’t do. They feel decreased financial and emotional strain and less stress on their families, as well as less chance that family and social activities will be negatively impacted. Finally, and importantly, they will have a reduced likelihood of permanent unemployment and negative impacts on their health and financial situations caused by not working.
In summary, a REWARD program can improve
a company’s operations and bottom line, and
the lives of its employees, in multiple ways.
How Does This Toolkit Help Employers Return Injured Workers to Work?
The Bureau has gathered multiple resources—some from companies with successful return-to-work programs, and others from professional organizations that focus on workers’ compensation —and assembled them into this “toolkit.”
The needs of one employer are different than others’, so this “toolkit” contains help for small and large employers. A small company with few workers’ comp claims might need a guide that shows them what to do when a worker is injured. A large employer, with a sizeable number of claims, can benefit by developing a more comprehensive program with staff dedicated to working with injured employees. But any size company can find ideas to help to return their injured employees to work sooner. The first step is to develop a program that is already in place before an injury happens.
Getting Started: Before an Injury Occurs
There are six steps an employer can take before an injury occurs to establish a REWARD program.
1. Commit To Having a Return-to-Work (RTW) Program.
A successful REWARD program begins with top management making a commitment to a return-to-work program. The head of the company, its management, and all supervisors must believe in the value of returning injured employees to work as soon as the treating physician permits, even if working within the restrictions assigned by the physician requires worksite accommodations.
This commitment is demonstrated to employees by a return-to-work policy and is the basis of the RTW program.
If the company doesn’t have one, Tool #2 in the Appendix has two samples of an RTW Policy.
2. Communicate the Return-to-Work Program to All Employees.
Once the company has a written RTW policy, share it and the company’s commitment to the program with employees. They need to understand that top management values its employees.
A company’s frontline supervisors play an essential role because they are often the “face” of the company for those they supervise. Supervisors who support the program will make an injured employee feel missed while they are off work and support them when they return. They will encourage coworkers to be understanding and helpful to a returning employee who has a modified duty assignment.
Supervisors who don’t support the program can undermine it. These supervisors may discourage employees from returning unless they are at 100 percent. They may be unwilling to look for possible accommodations that would allow injured employees to return sooner and make it difficult or unpleasant for employees who have job restrictions and need accommodations. They don’t understand the benefits to everyone for bringing injured employees back as soon as possible.
Top management should regularly reinforce its
commitment to the return-to-work approach
to supervisors and impress upon them that
they are critical to the success of the program.
They are!
The best time to introduce a company’s RTW program is the first day of employment. Most companies use the first day to explain their mission statements, values, rules, and policies and procedures. Covering the company’s approach to RTW of injured employees conveys company values, improves business performance, and fits within a company’s rules and policies. Discussing the RTW program is an important part of onboarding employees.
When providing information on the RTW program during onboarding, it will improve new employees’ commitment to the company and might reduce turnover. Explanation of the program should include:
- Accident Prevention and Safety – A safe workplace is the best return-to-work program, and safety is a core value of the company. Safety is also the responsibility of every employee. Let them know that following safety rules is an absolute condition of employment.
- Report Procedure – If an injury occurs, all employees should be aware of how and when to report it. Failure to notify the right person immediately when an injury occurs is one of the reasons that claims might get off to a poor start. The Bureau’s Posting Notice should be displayed in a prominent place. This will reinforce this information.
- Introduction to RTW Coordinator – Introduce new employees to the person responsible for return-to-work coordination. This is a vital step. A positive first impression is important to letting new employees know whom to contact with questions and that they can trust the RTW coordinator.
- RTW Policy and Acknowledgment – Go over the company’s RTW policy and explain that the company believes that early return to work is good for employees and the company. Presented as a benefit of employment, new employees will feel that they are starting a new job with a good employer.
Explain any time limits on how long the company will allow injured employees to work modified- or restricted-duty assignments or any maximum length of time the company will hold the injured employee’s job open for them. Disclosing these time limits maintains transparency and reduces future misunderstandings.
A Top Priority
At Charter Construction, we will not rest until all hazards are controlled and our employees are provided a workplace that is free of recognized hazards! When accidents do happen, it is a top priority, from our owners, management, and insurance company to provide the best care available to our employees.
– John Burch, Sr. Safety Coordinator, Charter Construction, Inc.
3. Designate Someone To Serve As The Return-To-Work Coordinator.
An important person in an RTW program is the RTW coordinator. This position doesn’t have to be a full time position or even have the job title. That decision will depend on the needs of each company. The RTW coordinator communicates with injured employees to make sure they understand the workers’ compensation process and the RTW policy. They also interact with adjusters to make sure communications are accurate and to resolve issues that might arise. The RTW coordinator additionally interacts with medical providers, and he or she offers information on modified-duty positions, job descriptions, and accommodations that might enable an employee to return to work. They also work with case managers to make it easier for them to provide the best services to injured employees, and they communicate with supervisors to ensure that they are an effective part of injured employees’ paths to recovery.
Whether full- or part-time, one of the RTW coordinator’s most important roles is to promote a positive RTW culture and oversee the implementation of the RTW policy.
More detailed information on the role of the RTW coordinator is in Tool #3 in the Appendix.
4. Establish a Positive Relationship with the Adjuster.
This will help the employee, the company, and the adjuster. The best person to do this is the RTW coordinator.
Adjusters’ jobs can be difficult. They often have large caseloads. Their job is easier, and the employer will see better results, if they have the information needed to do their job and an effective contact person at the company, the RTW coordinator.
Without a positive working relationship with the adjuster, problems might result, such as delays in employees receiving treatment and benefits, and less frequent communications with injured employees. These problems can cause negative feelings against employers as well as the adjuster, and they can create avoidable disputes that can impede claim resolution.
To establish a strong working relationship, the RTW coordinator needs to ask the insurance company or third-party administrator to identify the adjuster(s) who will be assigned to the company’s claims and provide their email address, direct phone number, and fax number. The RTW coordinator should then discuss the company’s expectations for claims-handling with the adjuster.
The primary expectations are that the adjuster will, as much as possible, avoid delays, help injured workers receive their lost wage benefits timely, and promptly approve prescribed, appropriate medical treatment. The adjuster will provide their contact information (email and direct phone number) to injured employees. The adjuster should answer calls from the RTW coordinator and injured employees whenever possible rather than communicate only through voicemails. Not accepting phone calls is one of the most frequent complaints about adjusters. The adjuster will notify the RTW coordinator of any changes in the assigned adjuster promptly. It’s not unusual for the adjuster handling a claim to change during the claim’s life. This is especially true if the claim involves extensive injuries, or if it evolves from a medical-only claim to one with lost time. Adjusters are required to alert the injured employee and the treating physician if a claim is reassigned. If necessary, the RTW coordinator should facilitate this.
Most importantly, the adjuster should be a resource to provide answers to the questions employees will have along the way.
To help adjusters do their jobs well, the RTW coordinator should agree to provide:
- Contact information, so the adjuster has direct access to the company when needed.
- The injured worker’s contact information (home phone, work phone, cell and email). The more ways the adjuster can reach the injured worker, the better. Often delays result because the adjuster doesn’t have the most current information and can’t get in touch with the injured employee.
- Accurate injury and accident details, payroll and personnel records, and any other information that will facilitate the return-to-work process.
If the company is large and operates in multiple states, it might have an account representative with an insurance carrier with whom to discuss expectations. If the company isn’t large enough to have an account representative, it might still have a dedicated adjuster for any claims it will have. Call the insurance company’s 1-800 number to establish a connection with that adjuster. Or, contact the local insurance agent who sold the company its workers’ comp policy for help in establishing a relationship with the adjuster.
5. Establish a Relationship with the Case Manager.
When an employee is injured at work, they are often scared and confused. Unless the employee has had work injuries in the past, the injured worker won’t know how the work comp system works. If the injury is complex, their fear and confusion can be overwhelming. Often the injured worker will turn to someone for advice and help. If the employer doesn’t give them an advocate to help them through the process, they might go in search of one who isn’t qualified to steer them in the right direction, or worse, they might reach out to people who don’t truly have their best interests at heart. In either case, the outcome is rarely beneficial.
Involving case management early promotes healthier relationships between all parties because the worker feels that they have an advocate. The case manager can explain the treatment in lay terms, facilitate earlier appointments, and collaborate with the physician. This results in more timely treatment and a shortened time that a claim is open.
An experienced case manager is trained to assess and monitor the treatment to make sure it’s based on acceptable medical standards. They know the local medical providers who have experience in workers’ compensation cases. If the injured worker’s recovery isn’t progressing, the case manager can look for alternative medical options and discuss them with the authorized treating physician (ATP). An effective case manager will begin to discuss return-to-work possibilities with the employee, employer, adjuster, and doctor at the beginning of the injury. The case manager should understand that the employee might be frightened about the potential of losing their job and worried about how they will make a living after the injury. They can set the tone and pace for the injured worker’s recovery. A skilled case manager understands that the best possible outcome for the injured worker is to get them appropriate treatment to recover and to set the expectation of returning to work in some capacity as soon as the injury occurs.
In other words, a case manager can help shorten the span between an employee’s injury and their return to work. They’ve been compared to a train. If the case manager gets on at the beginning of the trip, the case is far less likely to derail.
Utilizing the services of a capable case manager can save on medical and indemnity costs.
For more information on the role of a case manager in successful RTW cases, see Tool #4 in the Appendix.
6. Choose the Right Medical Providers.
The most effective return-to-work programs rely on the right medical providers. Finding the best physicians is important because employers in Tennessee have the right to participate in the physician-selection process. Workers’ compensation law allows employers to “designate” three or more physicians from which their employees must choose the physician who will treat them. This right is explained in greater detail in the “After an Injury Occurs” section of this document.
Before an injury occurs, identify providers who support return-to-work policies and will be suitable candidates for panels. Look for physicians who focus on recovery from the first office visit. Find physicians who work with injured employees and their employers to identify work possibilities and job modifications that allow them to return as soon as possible.
Place the physicians identified into a “pool” of physicians available for panels. Important considerations when physicians are placed into the pool include:
- Location. Not all employees live in the same area or have convenient access to the same physicians, so the company needs physicians to cover communities where employees live or work.
- Specialized expertise. Not all injuries involve the same body parts or require the same type of treatment or specialty, so the company needs a variety of specialties. The best pools have physicians from specialties such as orthopedics, occupational medicine, and walk-in clinics, so panels can be quickly produced for the most common workplace injuries.
- Willingness to treat. While many physicians accept workers’ comp patients, not all do. Others see injured workers infrequently. Do the research before an injury occurs to identify the best providers for the pool. The law requires the providers listed on a panel be able and willing to provide medical care to workers’ comp patients. Listing providers who aren’t exposes an employer to the risk of a monetary penalty. This pre-injury research allows employers to provide the best medical treatment to their injured employees.
Understand the Benefits
Early return to work benefits the employee with a faster recovery, staying in the routine of working, maintaining workplace relationships and skills, and enhanced selfworth. Physicians should practice effective, empathic communication strategies to help injured workers understand the benefits of early return to work.
- J. Mark Melhorn, Editor AMA Guides to Disease and Injury Causation
Getting Started Checklist
- Create an RTW culture.
- Communicate information on the RTW program to employees.
- Develop an RTW policy.
- Make sure supervisors are on board with the RTW program.
- Appoint an RTW coordinator to assume the responsibilities in the Toolkit.
- Establish a positive relationship with the adjuster.
- Select the right physicians for panels.
After An Injury Occurs: Implement your Plan
A REWARD program should allow for three important steps to take after an injury occurs.
1. Help Injured Employees Obtain Medial Care.
Provide medical attention rapidly. If the injury appears serious, call 911. If the injury doesn’t require emergency treatment, having a pool of physicians already developed will make the next step much easier. Tennessee employers have a right to provide an appropriate panel of physicians who are willing and able to treat an employee reporting a work injury.
Employers should follow these procedures when offering panels. While employers have the right to choose the providers listed on a panel of physicians, they don’t have the right to require injured employees to receive care from a specific physician on that panel. The physicians’ names must be provided on the Bureau’s form, called an “Employee’s Choice of Physician form.” It should be provided within three business days of when the employer received the report of injury and the employee expressed a need for medical care.
Sometimes multiple panels need to be provided if multiple body parts are injured.
The form must name at least three physicians who aren’t associated in practice together. If walk-in clinics or urgent care facilities are listed, list the name of the staff physician or medical director working there and not just the name of the clinic to comply with the law.
Some large employers have a medical provider or nurse on-site. They use this provider to help identify the type or specialties of medical providers to list on the panel. An onsite provider doesn’t alleviate the requirement to provide an appropriate panel, but it can be listed on the panel.
The injured employee must choose one physician from this panel. Their choice becomes the “authorized treating physician” (ATP). After an injured employee has selected their ATP, provide that physician with information that helps them treat the injured employee:
- The injured employee’s current job description.
- The return-to-work policy and modified-duty assignments available for the injured employee.
- The RTW coordinator’s direct phone number and email.
- The adjuster’s name, direct phone number, and email.
- Information about pharmacy benefits options, if applicable.
When providing the doctor written information, copy the injured worker as well. Make them feel like their recovery is a team effort, because it is.
Making the most of a pool of physicians doesn’t end with the selection of the right physicians. Establish a productive working relationship with those physicians by providing information to streamline decision-making and help them provide the best care to their patients.
See Information Exchange Between the Employer and the Authorized Treating Physician (ATP), Tool #7 in the Appendix which also includes a sample form, Contact Information for Medical Providers.
2. Report the Injury.
Report workplace injuries to the adjuster immediately. Tennessee workers’ compensation rules and regulations require employers to contact the adjuster within 24 hours of being notified of an injury and need for medical care. Coordinate the completion of a First Report of Injury with the adjuster for submission to the Bureau of Workers’ Compensation.
After reporting an injury, provide the adjuster with contact information for the injured employee. Include their home phone, work phone, cell and email. The more ways the adjuster can contact the injured worker, the better.
- Reporting a claim to an insurance adjuster doesn’t mean an employer has accepted the claim as
compensable. It only means that an injury has been reported. - Employers don’t have the right to refuse to accept an employee’s report of an injury, even if they
believe that the employee is being untruthful. Workers’ compensation rules and regulations
require the adjuster to investigate claims before they accept or deny them based on their
findings.
Sometimes a company is reluctant to report a claim to the adjuster. This reluctance might come from a fear that a claim report will increase their insurance premiums—especially if the company is small, or if the injury isn’t severe. However, simply reporting an injury won’t increase premiums; premiums are based on actual costs incurred and not on the number of injuries that are reported.
Other times, this reluctance is because the employer doesn’t believe that the worker got hurt, or they don’t believe the employee’s version of events. Not reporting an injury as soon as it is reported might delay medical care and cause additional harm to the injured employee, as well as delay their recovery and return to work. Delays in reporting an injury could also result in a monetary penalty.
The longer an employer delays reporting an injury, the greater the chances that the adjuster’s claims-handling and the injured employee’s recovery won’t go well—either from problems caused by delayed treatment or a lack of trust that develops with the injured employee.
If the company has questions or doubts about how the injury occurred and is hesitant to report it, report it anyway and convey the concerns at the same time. The best practice is to always report an injury and provide necessary treatment until the adjuster decides whether the claim is compensable. Help them conduct their investigation by providing the reasons for the concerns, copies of witness statements and any other helpful information. Also, let the adjuster know quickly if the employer’s opinion changes. As in most of life, effective communications during the claim will make a positive difference.
3. Let the RTW Coordinator Become an Advocate and Source of Information for Injured Employees.
Injured employees will have questions, and where they turn for answers is important. They might turn to their family, friends, advertising, or the Internet. These sources of information are often inaccurate. It is better if they consider the RTW coordinator an advocate and their primary information resource. The RTW coordinator should be accessible, empathetic, and ready to provide injured employees helpful information in case they have questions or problems obtaining their benefits.
The start of the claim is an appropriate time to talk to injured employees about the advantages of returning to work when they’re medically able within their restrictions and the disadvantages if they decline. Encourage them to accomplish the short-term goals physicians give them at each appointment. The success from meeting these short-term goals will give employees a sense of accomplishment and support their commitment to additional goals. This employee-centric approach will make recovery more likely and lead to the return of the employee to work, whether on a modified-duty or full-time basis.
The Bureau has developed several resources to help injured workers learn more about their rights and responsibilities. Here are some that an RTW coordinator might provide:
- The Bureau’s Beginner’s Guide to Tennessee Workers’ Compensation.
- The Bureau’s website. Visit the area of the website that is intended to assist injured employees
is located here. - The Bureau’s Ombudsman phone number: 800-332-2667.
In addition, provide them with a copy of the company’s RTW policy.
- Unfortunately, an injury might be catastrophic. These cases require a different approach.
See The Catastrophic Injured Employee, Tool #10 in the Appendix.
Post-Injury Checklist
- Accept the report of injury from the injured employee and provide emergency care if necessary.
- Report the injury to the adjuster, sharing any concerns about the claim.
- Use the pool of physicians to develop an appropriate panel of physicians based on the specific injuries reported and the location of the injured employee’s "community" (home address).
- Present the panel to the injured employee on the Bureau’s Employee’s Choice of Physician form.
- Request the employee to select a physician from the panel, and sign and return the form. The physician selected becomes the Authorized Treating Physician(ATP).
- Assist the employee in the recovery process. Anticipate questions, and provide useful information such as the Beginner’s Guide to Tennessee Workers’ Compensation, the Bureau’s website and the number to the Bureau’s Ombudsman Program: 800-332-2667.
- Highlight the benefits of returning to work and advise of the consequences of refusing a transitional duty assignment.
Transitional: Return to Work
One of the major hindrances to returning to work sooner is the misconception that injured employees must be 100% recovered before they can return. Management might worry about the safety of the injured employee, or coworkers might think that the injured employee can’t be productive at work. Some injured employees may have concerns also. They may fear additional injury, have family or other concerns even if a transitional position would mean more money than the temporary disability benefit.
However, many transitional (light-duty) assignments can serve both the employee and the company well and help the injured employee recover sooner.
Most return-to-work assignments are short-term. Employers with employees represented by a union need to remember that under some union contracts, a temporary assignment becomes permanent if it extends beyond a certain length of time.
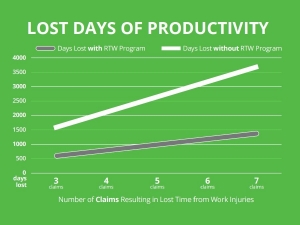
Appropriate assignments benefit all involved. They contribute to the employees’ recovery by keeping them productive, engaged, and active. Transitional assignments help shift everyone’s focus from the injury itself and job duties that can’t be performed to their recovery and job duties that can be performed if accommodations are made. A U.S. Department of Labor study found that only 50% of injured workers who didn’t return to work within 12 weeks of their injury would ever return to work. Fortunately, this outcome can be avoided.
Who's 100% On Any Given Day?
Time away from the workplace is a distance that grows larger and larger both physically and emotionally. I am frustrated with “don’t come back until you are 100%” statements from employers. Who is at 100% on any given day? It’s a standard that can’t be met and leads to loss of a lot of employee time. It may result in loss of the employee altogether.
- John Lochemes, MD, Titan Orthopedics, Memphis
To be effective, transitional assignments must be meaningful and take into consideration an employee’s skills and experience as well as physical restrictions that are necessary while the recovery continues. Assignments
such as “counting paperclips” or simply watching safety films might be perceived by an injured employee as a punishment rather than a positive step back to their job. After identifying transitional duties that might be available, a company should consider how existing jobs could be modified to allow the injured employee to do them. For example, a business process might be redesigned to eliminate lifting, or a lift-aid might make the job possible for the recovering employee.
To implement transitional assignments, RTW coordinators should monitor injured employees’ ongoing medical care and maintain communications with them and the treating physicians throughout their recoveries. They also should track the injured employee’s increase in functional capacity after each physician appointment and use that information to speak with the physician and injured employee about when the employee can return to work, either in a transitional assignment or in the pre-injury job with some accommodations.
When a transitional work plan has been developed and the employer is ready to offer the employee a temporary assignment, Tool #8 in the Appendix will be helpful. This tool includes: Transitional Work Placement Offer, Transitional Work Placement Job Description/Analysis – Physical Demands, and Sample letter to a Medical Provider about a Transitional Position.
Employers should keep in mind, however, that the decision to accept a transitional work assignment is ultimately the injured worker’s call. This makes it important for the RTW coordinator to be a trusted advocate and source of information for the injured employee, so they have the information they need to make an informed decision and have a positive outlook about the company and their return.
Strive to Accommodate
We strive to be able to accommodate restricted duty as soon as the provider is able to release the employee to come back to work. In doing so, the employee will receive their full weekly compensation. He/she is able to provide for their family the same as they did prior to the incident. It also benefits a company by the employee working at some capacity until they can return to full duty.
- John Burch, Sr. Safety Coordinator, Charter Construction, Inc.
Providing Transitional Duty Assignments Checklist
- Develop a list of meaningful transitional-work assignments.
- Provide the list to the ATP as early in the recovery as possible.
- Obtain specific information from the ATP about the physical tasks that employee can and cannot do.
- Monitor the course of the employee’s recovery and increase in functional capacity.
- Develop a transitional work plan with the injured employee and his/her supervisor within the guidelines provided by the ATP and offer the assignment to the injured employee.
If an injured worker can’t return to work for the company, that doesn’t mean they can’t return to any work at all. Tennessee’s workers’ compensation system has a resource available that might help called the “Next Step” program. This program helps injured workers who lose their job because of a
work injury to re-enter the workforce in a new field.
The Next Step Program utilizes state, federal, and non-profit programs to help injured workers obtain vocational assessment and testing, employment training, resume writing assistance and interview preparation, job analysis for in-demand jobs, and education at Tennessee public community colleges, universities, and colleges of applied technology.
Funding is available for injured workers who have a compensable injury, a permanent, partial disability, and received an “increased” disability award for not returning to work. Funding is limited to tuition, books, and materials required for courses in the maximum amount of $5,000 per fiscal year (July 1 – June 30) for four years.
The Bureau will provide step-by-step assistance with college applications, including completing the Free Application for Federal Student Aid (FAFSA).
For more information, contact the Next Step Program Specialist, Marion White, at 615-253-1204 or at marion.white@tn.gov.

The Tennessee Bureau of Workers’ Compensation invites interested employers to join the REWARD Employers Group. This free group has no eligibility requirements and offers many benefits.
The REWARD Employers Group will receive bi-monthly newsletters with articles by experts in the fields of workers’ compensation and return-to-work programs.
The Bureau will host quarterly meetings of REWARD employers. The first meeting will be virtual, but we expect meetings afterward will be in-person with a virtual option for employers who cannot travel. These meetings will include a speaker on topics of interest and opportunities to share experiences and learn from other employers.
The Bureau will begin a special recognition program (REWARD Honor Roll) for employers whose return-to-work programs meet certain criteria. The benefits of this recognition include permission to use the Honor Roll logo in company publications, and complimentary registration for their RTW coordinator at the Bureau’s annual educational conference.
Honor Roll employers exemplify the REWARD Program Principles and must show proof that they have:
- Created and maintained a return-to-work program that has:
- Been in effect for at least twelve months,
- A written return-to-work policy
- A designated return-to-work coordinator as defined in the Bureau’s REWARD Program Toolkit.
- Communicated their return-to-work policy with all current employees.
- Communicated their return-to-work plan with physicians.
- Offered, over the last twelve months, panels of physicians to employees within three days of their report of a work injury and their need for medical care in accordance with T.C.A. § 50-6-204.
- Maintained good standing with the Bureau of Workers’ Compensation as determined by the Administrator.
- Displayed the BWC’s Posting Notice in a conspicuous location in all appropriate languages.
- Utilized their return-to-work plan where possible.
- Submitted a completed Honor Roll application no later than November 15th for consideration of the following calendar year.
In Conclusion
This information and the tools that follow in the Appendix are resources for employers to gain the rewards of returning employees to work and reducing their disabilities. The Bureau hopes employers will join it in improving Tennessee’s workers’ compensation system by focusing on injured worker recovery in all claims. For questions or more information about the REWARD Program, please contact: WC.Info@tn.gov.
Appendix: ROI Calculator | RTW Difference in WC Benefits | Sample Return to Work Policy | Return-to-Work Coordinator | The Role of Case Managers | How to Pick the Right Panel Physicians for Workers’ Compensation Claims | Certified Physician Program | Information Exchange Between the Employer and the Authorized Treating Physician (ATP)| Transitional Work Letter to Physician, Placement Offer (Template), and Job Description/Analysis - Physical Demands Form | Job Description/Job Analysis | The Catastrophically Injured Employee | Evaluation of a Return-to-Work Program
REWARD Tool #1: Return on Investment Calculator
It takes an investment to implement an RTW program. For example, a RTW Coordinator will be paid to help injured employees return to work by adapting jobs and finding meaningful work opportunities. Is the investment it takes to implement a program worthwhile? This form is designed to help employers conduct a cost/benefit analysis.
Instructions:
In this example, we show the financial impact for an average Tennessee employer by using an average Tennessee employee (we named her “Jane”). Jane earns $20 per hour, was injured at work and missed 960 hours of work, about 24 weeks. When Jane returned to work with an RTW program, she only missed 456 hours of work. The impact on her employer is dramatic—even after factoring in the cost of the RTW Program.
To develop your own estimates: enter your details on this fillable PDF, let the calculator do its magic, and compare.
| Example | Jane's Sample Data | Calculation Explanation |
|---|---|---|
| Before her injury, Jane made $106.12 worth of widgets per hour. | $106.12 | To calculate your hourly productivity: Divide revenue by labor hours. Download a spreadsheet of hourly productivity estimates per industry. |
| Jane's work injury caused her to miss 960 hours of work when there is not a RTW Program. | x 960 | Why 960? TN BWC stats show that the average TTD period is 24 weeks. 24 x 40-hour work week is 960 hours. |
| Non-produced widgets causes lost revenue totaling. | = $101,875.20 | |
| RTW Program allows Jane to work 504 hours. | 504 | Why 504? RTW reduces out of work by 12.6 weeks. Learn more from this RAND study. |
Jane's productivity is lower because of her restrictions. She can make $88.82 worth of widgets per hour. |
x $88.82 | Why $88.82? Estimated 16.3% loss of productivity. Learn more from this Cornell University study. |
| Jane's ability to make widgets reduces the amount of lost productivity or unmade widgets by this amount. | = $44,765.28 | |
| Cost to run the RTW program for Jane | - $1500.00 | Includes costs for equipment, vendors, and RTW coordinator per RTW injury. Learn more about RTW at askJAN.org. |
| RTW created additional net income of: | = $43,265.28 | |
| RTW Program reduced wc claim costs | + $15,899.82 | Calculate this with the "Effect of Return to Work on WC Payments" tool. |
| Employer's Net Benefit of Return to Work Program for Jane's Injury | = $59,165.10 | |
This is a simple model for illustrative purposes. Each business is different and should consider appropriate information and context for itself. Costs to replace injured workers may also be taken into account including lost productivity while recruiting and training in addition to overtime and other costs. For questions, comments or to discuss options for your company, contact Brian.Holmes@tn.gov, 615-253-1206.
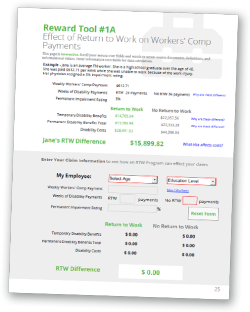
Reward Tool #1A: Effect of Return to Work on Workers' Comp Payments
Download an interactive PDF of Tool 1A.
Example
Jane is an average TN worker. She is a high school graduate over the age of 40. She was paid $612.71 per week while she was unable to work because of the work injury. Her physician assigned a 5% impairment rating.
| Example Factors | Example Amounts | |
|---|---|---|
| Weekly Workers' Comp Payment View more about workers' compensation benefits. |
$612.71 | |
| Weeks of Disability Payments Why are these different? A RAND Institute study shows an average of more than twelve additional weeks of disability for injured workers who do not return to modified work. |
(RTW) 24 Payments | (No RTW) 36 Payments |
| Weeks of Disability Payments | 5% | |
| Benefits for Jane Example | Return to Work | No Return to Work |
|---|---|---|
| Temporary Disability Benefits Why are these different? A RAND Institute study shows an average of more than twelve additional weeks of disability for injured workers who do not return to modified work. |
$14,705.04 | $22,057.56 |
| Permanent Disability Benefits Total Why are these different? Tennessee Code § 50-6-207 provides additional permanent partial disability benefits to injured workers who do not return to work after a work injury compared to those who do. Learn more. |
$13,785.98 | $22,333.28 |
| Disability Costs | $28,491.02 | $44,390.84 |
| Jane's RTW Difference What else affects costs? A study of the Washington State workers' compensation system shows non-light duty workers had medical costs that were seven percent higher than those who did perform modified work. The TN BWC 2019 Annual reported the average medical expenses per claim in the period 2015-2018 was $22,816. This represents additional RTW savings in the amount almost $1,600. |
$15,899.82 | |
Company Letterhead
Date:
TO: All Employees
(Company Name) values its employees and commits to providing a safe and healthy work environment for them. Illnesses and injuries might still occur occasionally, and when an employee has a work-related, compensable illness or injury, our policy is to try to provide opportunities for every employee to remain at work or return to work as soon as medically possible.
(Company Name) will work with the recovering employee and the authorized treating physician (selected from the panel provided by (Company Name)) to identify transitional job assignments when the employee is not able to do all or part of their regular work during their recovery. Traditional job assignments for meaningful and productive work will be temporary and based on information provided by the employee’s authorized treating physician. We believe this approach will help our employees to come back to work sooner, which is our goal. This also means our employees will be able to return to their pre-injury wages and benefits sooner.
This policy applies to all employees who are unable to perform part or all their regular work duties from a compensable, work-related injury or illness. All employees are expected to fully cooperate in the safe and timely return to work when they are injured.
Chief Executive Officer Signature ______________ Date ___________
(Company Name) values its employees and commits to providing a safe and healthy work environment for them. Illnesses and injuries do occur, and when an employee has a work related, compensable illness or injury, our policy is to provide opportunities for every employee to remain at work or return to work as soon as medically possible. This policy applies to all employees and will be followed whenever possible.
(Company Name) will work with the recovering employee and their physician to identify transitional work when the employee is not able to do all or part of their regular work while recovering. Transitional job assignments for meaningful and productive work are temporary and based on information about the employee’s physical abilities provided by the employee’s physician (selected from the panel provided by (Company Name)), the business needs of (Company Name), and the availability of alternate work. (Company name) reserves the right to determine how long the transitional job will continue.
If the physician releases the employee to return to work for a transitional job, the employee shall obtain a Release to Return to Work that includes the physician’s opinion of the physical demands that the employee can meet in a transitional job assignment. The employee must make sure that they do not work outside either the duties of the transitional job assignment or the physician’s restrictions while in a transitional job.
The Return to Work coordinator (or name of the person who has the responsibility for the company’s return-to-work program) will monitor the employee’s case to assess the employee’s progress and to make changes if warranted.
Chief Executive Officer Signature ____________________ Date __________
Worker acknowledgment
____ I have read the policy and was given an opportunity to have my questions answered.
____ I agree to comply with the policy and its procedures.
____ I understand failure to follow this policy might affect the continuation of my transitional job-duty assignment.
Employee Signature ____________________ Date __________
REWARD Tool #3: Return-to-Work Coordinator
The pivotal role in a successful return-to-work program is the return-to-work (RTW) coordinator. This person is the linchpin who pulls all the elements together for injured workers to focus on returning to work.
Many employers use a safety manager, human resource professional, risk manager, or case manager as a return-to-work coordinator. Whether it is a full-time position in the company, or in conjunction with other responsibilities, a return-to-work coordinator seeks to combine collective efforts for a common goal.
Each instance of a meaningful return to work is a combined effort of people and resources. It starts with commitment of the company’s leadership. Top management, middle management, and supervisors must create a return-to-work culture. Frontline employees must operate within the culture, believe in its goals, and contribute to it.
It also requires commitment from physicians, adjusters, and case managers. Their approaches after a work injury significantly impact a program’s success. The list of people required to coordinate a positive and meaningful return to work outcome is extensive.
The RTW coordinator’s skills should also be extensive. The ability to communicate with leadership and frontline employees is an important skill and involves the ability to establish rapport, build credibility, and effectively persuade and influence.
Another asset for an RTW coordinator is knowledge of workers’ compensation law and processes. Tennessee workers’ compensation is like many states; yet, it is unique in many ways, too. For example, in Tennessee the employment must be the primary cause of an injury for the employee to have a compensable workers’ comp claim, while in many other states the employment must only contribute to the injury.
This medical and legal distinction affects many claims. Selecting physicians who understand this distinction is an important duty for an RTW coordinator. Having the right physicians evaluate, diagnose, and provide appropriate care and return-to-work guidance significantly impacts the success of a return-to-work program.
See Tool #5 for more information about selecting and working with physicians.
Physicians depend on accurate job and task information to make appropriate restrictions and define return-to-work parameters. RTW coordinators need to provide them and establish effective return-to-work communications with physicians, to ensure they can place injured workers appropriately.
See Tool #9 for more information about job descriptions and job-demand analyses.
Coordinating return to work includes complying with Tennessee state and federal laws such as Title VII, ADA, and FMLA. An RTW coordinator should know how these laws apply so they can provide accurate information to managers, supervisors, and employees. As noted on pages 8-9, an RTW coordinator should be an advocate and source of information for injured employees.
Advocacy and Trust Pre-Injury
A key component to being a trusted advocate and source of information is a positive relationship among coordinators, supervisors, and injured workers. Conscientious, intentional trust- and rapport-building activities among the three contribute to a positive relationship.
They need to understand that returning to work benefits everyone and gets to the heart of a REWARD program. Injured workers who return to work have better recoveries. On average, their disability periods are shorter, and medical costs are lower. Return-to-work coordinators must help injured workers understand this fact. They should remind them that having a workplace injury doesn’t mean their employment relationship ends.
Fear of retribution can cause some employees to be afraid to report an injury. They think they are putting their jobs at risk. One study found that men are less likely to seek medical care. Some workers might think that their injury will get better with ice, over-the-counter pain relievers, or rest, so they don’t report it for those reasons.
All employees need to be taught and reminded to report their injuries immediately. A reporting delay might make an injury worse. In addition, nursing an injury without appropriate medical care can lead to decreased productivity.
Delayed reporting can cause credibility concerns when an injury is finally reported, especially if it comes after a supervisor expresses productivity concerns or disciplines the worker.
Disputes often arise when injury reports are not timely or complete. The mechanism of injury might be expressed in vague terms due to language barriers, fear of punishment, or a lack of knowledge. Sometimes an injured worker only knows his leg and hip hurt; he doesn’t know that a herniated disk in his back is the cause. Return-to-work coordinators who understand the problems that these discrepancies cause and work to prevent them can prevent problems before they occur.
Advocacy and Trust Post-Injury
Trust and rapport are also developed and improved after an injury by intentionally establishing and maintaining connections between the company and the injured worker. Supervisors and return-to-work coordinators should contact injured workers often to show concern and maintain relationships, as well as keep them connected to their co-workers.
Return-to-work coordinators should begin by explaining the workers’ compensation claim process. Include details about the roles of the physician, adjuster, case manager, and the RTW coordinator. Highlight the benefits of modified duty in recovery. They should provide the injured worker the adjuster’s name and contact information. Employee advocacy also includes giving information to the adjuster to assist with timely benefit-eligibility determinations.
Provide the adjuster with accurate contact information for the injured worker. This helps with investigation and improves the adjuster’s ability to communicate and establish a relationship with the injured worker. Good communication might reduce delays in decisions about compensability which can lead to delays in medical care and disability payments that will get the claim off on the wrong foot, cause mistrust, and undermine return-to-work efforts.
Adjusters are required to conduct thorough and timely accident investigations. Those who understand the mechanism of injury and applicable safety rules, interview witnesses, and obtain other pertinent accident information can quickly make compensability determinations. Pre-existing medical histories and accommodations also affect compensability decisions.
Once an adjuster accepts a claim as compensable, temporary disability benefits might already be due. Accurate payroll information helps get the initial payments online before a missing check becomes a problem. Return-to-work coordinators might coordinate with payroll staff when wages or hours are reduced for modified duty, so the adjuster can pay appropriate temporary partial disability benefits. Injured workers can quickly lose patience when income isn’t received, and bills are delayed or go unpaid.
Routine conversations with adjusters regarding the recovery plan and medical status are also part of return-to-work coordination. A common understanding about the need for diagnostic testing, surgery, post-surgical recovery periods, and modified duty provides an injured worker the return-to-work focus and improves the workers’ compensation claim experience. Routine conversations with injured workers also improve the claim process. If the return-to-work coordinator meets with injured workers in-person or virtually after every physician visit, it will provide an opportunity for a coordinator and injured worker to get to know each other better. This humanizes the relationship, builds trust, establishes rapport, and helps identify the need for support services.
The meetings also provide the opportunity to discuss the doctor’s prognosis and work restrictions. They set the stage for dialogue to make sure restrictions are followed at work and at home, and they lead to an appropriate modified-work placement. The worker’s feelings and perceptions about their medical care and recovery can also be explored. Some injured workers readily act on their own internal motivation to return to work. Others view returning to work and recovering as conflicting goals. They have questions, unstated fears, and needs.
Employers shouldn’t automatically discount workers’ concerns and judge them as being unwilling to participate. Listening to and addressing these matters are important to the success of an RTW program. An injured worker who is unsure about a work activity might need to give it a try before completely ruling it out. Discussing the activity and further modifications to alleviate concerns might be helpful. This is especially important when confronting fears of re-injury or performing new tasks with new team members.
Employees’ perceptions are critical because, more than anyone, injured workers are responsible for their own physical and economic recoveries. Their attitude and approach will define their ability to recover. Their cooperation and participation are gauges to understanding an injured employee’s attitude and beliefs.
A previously engaged worker who suddenly seems less interested might be experiencing a setback unrelated to their recovery. Or, it could be a problem caused by the adjuster, such as delays in getting medical treatment approved. Perceptive coordinators can take quick action when there are behavioral changes, even subtle ones, to improve recovery outcomes.
Understanding motivations and perceptions helps return-to-work coordinators identify recovery obstacles. This assists in understanding unstated interests and identifying appropriate and meaningful return-to-work options.
Meaningful Modified Work Pre-Injury
Identify appropriate and meaningful return-to-work opportunities before a work injury occurs to normalize the process and create return to work expectations. Organization and preparation add credibility, and they ease the transition for supervisors and injured workers.
Modified duty options can be identified with a thorough examination of the business processes. If some types of injuries occur more frequently, modified duty options for the job classifications associated with these injuries will be helpful. Consider long-term projects that might otherwise be given lower priority but are nonetheless important to the employer’s mission as a source for modified duty options. Other options are modified work at a different location or non-profits.
Several heavy-duty employers, such as trucking and trash-hauling companies, use non-profits to provide modified duty work. For example, injured workers are paid to work at shelters, food banks, animal conservatories, etc.
Here, they have daily interactions with people, learn new skills, and maintain a “get-up-and-go-to-work” mentality. This has proven to help workers improve their recoveries, reduce their disabilities, and increase the likelihood that they are able to return to the pre-injury employer after reaching maximum medical improvement (MMI). These successful outcomes are more likely if the employer has identified modified duty options before an injury.
In addition to identifying available modified duty jobs, examine how current jobs can be changed before an injury occurs. Should an infrequent task be re-assigned to another position? Can a process be re-designed to eliminate lifting? Can a lift-aid be used to modify the job?
Work with employees and supervisors to understand jobs and identify opportunities, pre-injury. They are the experts in doing their jobs and understanding the key tasks involved. Thoughtful consideration of how jobs can be modified, created, or re-assigned before a work injury communicates the return-to-work culture and the employer’s commitment to it for all employees.
Meaningful Transitional Work Ideas:
- Training
- Switching Jobs
- Changing tasks in a job
- Rotating between jobs
- Identifying organizational tasks that are incomplete.
- Look up specific injury and task accommodation ideas from SOAR, Searchable Online Accommodation Resource: askjan.org/soar.cfm
Meaningful Modified Work Post-Injury
Communicate to an injured worker about the role of modified duty in recovery after an injury. Make sure they know the physician’s role is to diagnose, treat, and return the employee to work. The physician should have been advised about the company’s intention to use modified duty in recovery. Send the injured worker to the first visit with the selected physician (ATP) with a work injury packet.
Flexibility is important. Some restrictions make sense with some jobs, but they don’t make sense with others. A return-to-work coordinator, in conjunction with the employee, is permitted to contact a physician for clarification of both restrictions and the jobs or tasks available to accommodate the restrictions.
Injured worker and supervisor participation with identifying return-to-work options after an injury is also important for buy-in and commitment from both. It clarifies tasks, roles, and expectations. Using restrictions and guidance from physicians, return-to-work coordinators should look at the modified positions identified pre-injury and discuss with both the injured worker and supervisor how to make the modified position fit the circumstance. They should also consider how the position can be expanded as functionality increases.
Coordination includes understanding what an injured worker can do, then finding or modifying jobs to accommodate their abilities. While providing a physician examples of modified duty jobs in a physician packet is helpful, physicians should not try to fit injured workers into specific jobs. This is the responsibility of the coordinator, supervisor, and injured worker, with the physician’s guidance regarding capabilities to perform activities safely.
Once a transitional job is identified, put the position’s tasks and responsibilities in writing. Include:
- A brief description of the modified-duty assignment and the physical requirements that comply with the employee’s medical assessment;
- Anticipated duration of the assignment;
- The employee’s work schedule and pay rate;
- The location of the assignment;
- The name of the supervisor to whom the employee will report; and,
- A section for the employee to indicate acceptance or refusal of the assignment.
See a sample job offer form in Tool #7 in the Appendix.
Return-To-Work Coordinator Training
A successful return-to-work coordinator has strong people skills that inspire, motivate, and persuade. The Bureau of Workers’ Compensation (BWC) is currently developing a comprehensive twelve-hour certification program for return-to-work coordinators. The program is designed to introduce skills and techniques to help a coordinator be the catalyst that inspires and facilitates a strong return-to-work culture. Attendees will be certified for two years. The virtual and classroom experience takes the participant through the skills needed to successfully help workers return to work.
The training includes an in-depth look at the return-to-work coordinators’ job duties, teaches soft people skills proven to improve communication, and covers the basics of Tennessee workers’ compensation.
The BWC training will help return-to-work coordinators convince management and employee influencers to prioritize RTW. Common techniques include updating employee orientation or onboarding to include return-to-work expectations, engaging physicians to promote return-to-work, and influencing leadership to address anti-return-to-work behaviors.
The training also focuses on applying communication and motivation skills to help hesitant, injured workers take an active role in their own recovery via returning to work. This is more effective when the injured worker’s supervisor and co-workers are supportive. Effective techniques used by successful return-to-work efforts in companies across Tennessee will be explored.
For information regarding training opportunities, contact Brian Holmes, 615-253-1206 or brian.holmes@tn.gov.
The Bureau is committed to make Tennessee a better place to live and work. To this end, a return-to-work coordinator who leverages relationships and supports a return-to-work culture can build morale, reduce workers’ compensation costs, and shorten disability periods. This can lead to improved productivity, a positive return on investment, and a competitive advantage, while improving the future for injured workers.
REWARD Tool #4: The Role of Case Managers
Who is a Case Manager, and What Do They Do?
A case manager may be a registered nurse possessing one or more accepted credentials listed in the rules or a certified case manager with the Commission for Case Manager Certification who has met state requirements and is registered with the Tennessee Bureau of Workers’ Compensation to provide medical case management services for injured workers. They must meet educational and other requirements to maintain their registration.
The case manager acts as an advocate and liaison among all parties involved. The case manager actively works with the injured worker to obtain and coordinate the injured worker’s appropriate, cost-effective medical care, while developing a plan to help the injured worker return to life and work. Case management services may be provided in-person or telephonically.
Who Selects the Case Managers?
In Tennessee, any insurer or employer providing workers’ compensation coverage may use case managers. If so, the injured worker must cooperate with the case manager. An employer may allow their adjuster to select the case manager or choose the case manager itself. If the company opts to select the case manager, the RTW coordinator will need to interview and select a case-management organization that will best serve injured employees.
Is It Important to Establish a Relationship with the Case Manager Before an Injury Occurs?
Absolutely! Most reputable case-management companies and case managers are willing to meet to establish a relationship before they’re needed. Most will meet at the business to get a better understanding of what the company does, and the type of jobs employees perform. Ask for their resume(s) and get to know the person(s) who will be directly working with employees. They become an extension of the company, so they must be knowledgeable and personable.
If the case manager cannot establish a rapport with the RTW coordinator, then they probably can’t with injured employees, either. The ability to establish rapport with injured employees and build trust might be their most important task. Without them, the RTW coordinator won’t be effective in helping the employee recover. It’s not enough for a case manager to be knowledgeable and go down a checklist to get information; they need to have the ability to relate to people.
What Should Be Expected from the Case Manager?
The most effective case managers will want to collaborate with employers to ensure every injured worker is provided with the most appropriate medical care and the best possible options to return to work in some capacity. A seasoned case manager will know more about the most appropriate medical providers in their area than almost anyone in the process, so they can be an invaluable resource. They’re knowledgeable about the process because they’re in the doctor’s offices attending appointments. They visit patients in emergency rooms and ICUs. They talk to therapists about patients and review reports from numerous physical therapy clinics. They talk to plaintiff and defense attorneys. They do home assessments. They communicate with Bureau staff when they have questions. They see and talk to people on all levels of the process and can speak with them openly. They can provide the employer and the injured employees honest answers to tough questions. An experienced case manager will be able to deliver difficult messages with kindness and empathy.
When an employer establishes a trusting relationship with a case manager or case-management company, it will realize that it can call on them for advice about creating physician panels, developing modified-duty plans, finding treatment options, expediting medical care, and giving honest assessments of how the claim is going. Many employers and adjusters have found that an effective case manager can be the go-to person for information.
Does Every Occupational Injury Need a Case Manager?
No. Injuries such as simple cuts, bruises and strains don’t, as they can easily be handled by the RTW coordinator and adjuster. Case management is recommended if the injuries are complex enough that they require the use of medical specialists, hospitalization, or complicated surgeries. If an employee has frequent work injuries, many employers find it helpful to assign a case manager for continuity, who makes sure all the providers have the same information. The case manager might also investigate frequent accidents and help the employee and employer make simple adjustments to prevent future accidents.
In Tennessee, all catastrophic injuries should be assigned to a case manager. If the case is catastrophic, ask that the case manager be local, on-site, experienced with catastrophic injuries, and familiar with the providers. Catastrophic cases can rarely be effectively managed by a telephonic case manager.
Our Key to Success
Orgill, Inc.’s experience with case managers. Orgill, founded in 1847, is the world’s largest independent hardware distributor and is headquartered in Memphis.
RN case managers are the key to a successful return-to-work program and have been the longstanding backbone of Orgill’s successful and effective Workers’ Compensation and Safety program. Orgill takes the time to interview and select case managers at each facility who can manage every injury from start to finish, partnering with the company to ensure injured workers receive exceptional care. Apart from first-aid incidents, case managers are assigned immediately to all work comp injuries, securing timely medical specialist appointments; coordinating MRIs and physical therapy appointments; and ensuring workers know how to fill their prescriptions. All case managers who Orgill partners with tour our facilities, understand the physical requirements of each job, and can inform treating physicians of transitional-duty work that is available during doctor visits. Since case managers advocate for the injured worker from the very beginning of the injury and ensure receipt of exceptional care, Orgill has a very high percentage of workers who are able to return to work, and they obtain full duty/MMI more quickly and with less permanent impairment. Overall, the RN case manager is always better postured to make an affirmative impact with respect to an injured worker’s overall care, versus relying on an overworked insurance adjuster to handle coordination.
- Kelli Kelly, SPHR, SCP - VP, Human Resources, Orgill, Inc.
How Does the Case Manager Help the Injured Worker?
Work comp systems can be very confusing for employees because they are so different from their regular health insurance. The case manager will be able to talk the employee through the process, answer questions, and help them access medical care quicker and more efficiently. The case manager should act as an advocate for the injured employee’s return to work and coordinate medical care. As such their services benefit the employee and employer.
Can the Case Manager Change During the Life of the Claim?
Occasionally, case managers change for various reasons; however, the case manager should remain constant if possible. Changes in case managers leave the employee without a dependable advocate that they can trust to be honest and fair with them. It can also disrupt the continuity of care because the case manager generally knows all aspects of the care being provided. In Tennessee at least one face-to-face meeting between the case manager and the employee is required. A telephonic case management may send onsite case managers only to attend the doctor’s appointments. If the telephonic case manager feels the case needs frequent onsite visits, it might be appropriate to transfer the case to an on-site case manager, who can better manage the case. This is especially true if the telephonic case-management company does not use the same on-site case manager for each visit. Having a different on-site case manager show up at every appointment might leave the employee without consistency.
REWARD Tool #5: How to Pick the Right Panel Physicians for Workers’ Compensation Claims
Tennessee allows employers some choice in who an injured worker sees for medical treatment. To take advantage of this right, and to maximize the chances that injured workers will successfully return to work, employers must carefully choose the physicians listed on their physician panels.
Employers should develop a diverse “pool” of physicians with a variety of specialties and practice locations. This makes it easier to comply with Tennessee law to provide appropriate physicians within the correct communities.
Tennessee rules and regulations require a panel be provided within three business days of the date the employer has notice of the injury and the employee has expressed the need for medical care. The law also requires the panel be provided on the BWC form. The forms are available in two languages.
- Form C-42 | Employee’s Choice of Physician (English)
- Form C-42 | Employee’s Choice of Physician (Spanish)
Finding physicians to put in a panel pool is the first step. A valuable source of information to create a pool is the employer’s workers’ compensation carrier or third-party administrator (TPA). Most insurers/TPAs track physicians and have metrics on physician performance for common injuries (e.g. average time off work, average cost of care provided, etc.).
Another potential source of physicians for a pool is the Bureau of Workers’ Compensation (BWC) website. The site lists over seventy-five physicians who are on the Medical Impairment Rating (MIR) Registry. The registry lists doctors who’ve successfully taken the BWC’s course work on the AMA Guides to the Evaluation of Permanent Impairment, Sixth Edition and passed the required testing on impairment ratings in the Tennessee’s worker’s compensation system. The MIR registry list is posted online. The American Academy of Orthopaedic Surgeons Annual Workers’ Compensation and Musculoskeletal Injuries Course also provides workers’ compensation specialized physician training.
The Bureau’s Certified Physician Program will be a third source of physicians for an employer’s pool once it is launched in 2022. Before becoming certified, a physician will have completed specialized training facilitated by the Bureau and passed required testing on the Tennessee workers’ compensation system. They will have agreed to best practices that will help your return-to-work program be effective. At that time, the Bureau will post their names on its website.
For more information on the Certified Physician Program, see Tool #6 in the Appendix.
Employers who have employees in higher-risk job classifications, or have a higher rate of injuries, may find it beneficial to request a face-to-face meeting with prospective physician panel members. At this meeting, the RTW coordinator should explain the company’s business and its work processes. A tour of the employer’s facility so the physician can see the work done by employees has a significant impact as well.
Employers should explain and give the prospective physician a copy of the company’s return-to-work program. Include a current list of jobs available for transitional duty. Ask the physician whether he/she is willing to “foreshadow,” or predict the recovery improvement expected between one office visit and the next office visit. Foreshadowing is communicated orally to the injured worker and in writing to the employer in the physician’s office note and on the physician’s own work ability form. When placing a physician on the employer’s panel, provide the physician a contact information sheet listing the RTW coordinator’s and adjuster’s names and addresses, phone numbers, and email addresses.
A sample form is in Tool #7 in the Appendix.
Also, provide the adjuster’s supervisor’s name and contact information in the event the adjuster changes. For example, a medical-only claim that converts to a lost time claim often results in an adjuster change. Once a physician has been selected from a panel, monitor the physician’s performance to determine whether the physician should be placed on future panels. One monitoring metric is the injured worker’s recovery satisfaction with his/her physician. Interview injured workers after each physician visit to gauge the workers’ satisfaction with the physicians and to monitor the workers’ recovery with decreasing work restrictions.
Some workers may express dissatisfaction with the physician. Consider whether the dissatisfaction stems from the physician’s bedside manner or competency, or if it comes from an employee’s ill-advised desire to recover at home without a return to work. A second measurement is recovery progress. The injured workers’ recovery progress is measured by treatment progression, setbacks, and ultimate recovery. Treatment progression includes the need for multiple surgeries, increasing and decreasing restrictions, and approval of a physician’s treatment plan.
Frequent insurance company/TPA denials of testing, medications, and surgeries could be a problem with a physician or it could be a problem with the insurance company/TPA. The utilization review process is one way to tell which it is. Utilization review is a way to determine if a physician’s recommendations are reasonable and medically necessary. Insurance companies hire physicians to perform these reviews. Frequent denials and confirmation of the denials by the Bureau’s medical director might indicate a treating physician is recommending treatment that is not evidence based. Frequent denial reversals by the Bureau’s medical director might suggest erroneous denials by the insurance company.
The Bureau of Workers’ Compensation has adopted the Work Loss Data Institute ODG® Guidelines as the criteria used to determine the recommended treatments for injured workers in Tennessee. The Treatment Guidelines are recommendations, not mandates. Their use supports the goal of an accessible, transparent, single reference for determining the medical necessity of recommended treatments.
REWARD Tool #6: Certified Physician Program
The Tennessee Bureau of Workers’ Compensation developed a program to train, test, and certify physicians interested in providing best practices in the Tennessee workers’ compensation system. The program includes training on the workers’ compensation system in a self-paced, online training. Training will be provided in two stages. The first will include:
- The duties and responsibilities of the authorized treating physician.
- The forms physicians must complete.
- Injury causation analysis and report-writing.
- Use of the Work Loss Data Institute ODG Guidelines for treatment, with the presumption that those guidelines are correct.
- The importance of communication with the injured worker, adjuster and employer.
- The utilization review process and how to minimize friction and obtain the best outcomes for patients.
- The value of return-to-work, and tips on how to encourage the injured worker’s participation.
- The differences and appropriate assessment of risk-based “restrictions,” capacity-based “limitations,” and worker “tolerance” for symptoms.
- Written work guidelines, and how to foreshadow and coach expected goals for the injured worker, including expected increased activity for home and work.
- The assessment of maximum medical improvement (MMI), and the assignment of a permanent impairment rating and permanent work restrictions.
A test will be administered afterward. Participation in the program will include requirements for physicians concerning interactions with employers, their RTW coordinators, and case managers. Recertification will be on a three-year cycle and include a performance review.
The second stage will include training on the 6th Edition of the AMA Guides to the Evaluation of Permanent Impairment. This training will cover the medical and legal components of maximum medical improvement (MMI), and frequently used chapters of the Guides. A test will be given on this material as well.
After a physician has successfully completed training, the physician’s name, specialty, and contact information will be listed on the Bureau’s website as a certified physician.
Physicians and employers alike will gain from the certification program. Expected benefits for certified physicians will include added reimbursement for certain services, fewer utilization reviews, an increased number of patients, and a more satisfying experience in workers’ compensation. Benefits to employers that utilize these physicians are a reduced administrative burden, improved communications, less employee lost time, better employee morale, and lower workers’ compensation costs.
REWARD Tool #7: Information Exchange Between the Employer and the Authorized Treating Physician (ATP)
Employers can help the physician (ATP) chosen by the employee by providing information about the company and its operations. At the start of medical treatment, the employer should inform the ATP whether the employer has established that work caused the injury and accepted the claim or whether the cause is not known yet and the employer needs the ATP to provide an opinion about causation. Under Tennessee law the ATP’s opinion regarding causation is presumed accurate. Unless the physician knows at the time of the initial appointment that the employer is unsure whether the injury was caused by work, they are likely to assume that causation isn’t an issue, and the claim has been accepted.
If doubt exists about causation, the employee needs to be seen by the ATP physician because the causation opinion of a mid-level provider such as a physician assistant or nurse practitioner is insufficient, unless a physician reviews the records and clearly conveys agreement with the causation opinion of the mid-level provider by signing the record in which the opinion is expressed. Employers should also provide the physician:
- The employee’s job description. This information is crucial for the ATP to consider when placing work restrictions and in treatment-planning.
- The employer’s return-to-work policy. This conveys the employer’s preference for employees to work modified duties whenever possible.
- Contact information. The direct phone and email of anyone who has authority to discuss questions about return-to-work with the ATP, as well as for the adjuster and employee.
See the Employer Contact Information for Workers’ Compensation Medical Provider (Sample), below, which can be modified to meet the company’s needs.
Tool #8: Transitional Work Letter to Physician, Placement Offer (Template), and Job Description/Analysis - Physical Demands Form
- SAMPLE Letter to Medical Provider about Transitional Position
- SAMPLE Transitional Job Offer to Employee
- Transitional Work Placement Job Description/Analysis of Physical Demands
REWARD Tool #9: Job Description/Job Analysis
The packet that the Employer will provide to the panel physician will include the employee’s job description, job analysis, if available, and transitional jobs that are currently available with the employer or alternate assignments that the employer can provide.
According to the Society for Human Resource Management (SHRM), a job description is a useful, plain-language tool that explains the tasks, duties, functions, and responsibilities of a position. It details who performs a specific type of work, how that work is to be completed, and the frequency and the purpose of the work as it relates to the company’s mission and goals. It should also include the requirements for the position (education, certifications, etc.). The job description should also include a section on Essential Functions that describes which activities are the core functions of the
job that cannot be modified or delegated to others (Example: an airplane pilot’s essential functions would include the ability to land the plane in multiple weather conditions). Other work activities that are not essential functions can be detailed in a separate section.
Free information about how to develop a job description is available from SHRM.
A job description describes the work performed; a job demand analysis determines the force, repetition, and continuation of movements associated with a job, in addition to the body positions and movements required and the conditions of the surrounding environment. This requires measuring the size and weights of products, boxes, etc. and tools handled, the position of these objects in space when handled, and distances objects need to be moved. Employers with many employees in a specific, somewhat demanding job (for example a delivery driver with a truck line) are more likely to benefit from having a formal job analysis.
The many measurements and skills required for a job demand analysis make it more expensive than creating a job description. Formal job demand analyses should be written by a trained professional, such as a physical therapist, vocational consultant, or medical case manager. Their training includes
job demands, accommodations, and applying restrictions to determine a worker’s ability to perform a job. Confirmation of training and competency is recommended. Having a formal job demand analysis of positions might be appropriate for individuals with specific body part injuries. It will permit the RTW coordinator to ask the injured worker’s treating physician if the injured employee could return to temporary work in these particular jobs, while hopefully continuing to improve toward ultimate return to unrestricted work and the employee’s original job. In addition to return to work, employers may benefit from having a formal job analysis when assessing candidates for hiring.
REWARD Tool #10: The Catastrophically Injured Employee
Fortunately, catastrophic injuries such as a head trauma with serious brain injury or amputations are rare. When they do occur, it’s not just the injured employee who is affected. News of the injury creates a ripple effect throughout the company and the employee’s family. Catastrophic injuries are
extremely stressful for everyone involved. Emotions run high and the air is charged with tension which can complicate decision making.
Companies should have a plan for responding to a catastrophic injury. Planning for an injury that might never happen is preferable to responding to a crisis without preparation. The plan should include a checklist of the people who need to be notified and a list of actions that must be taken quickly. The plan needs to be developed in collaboration with the company’s safety/risk management division, legal team, case manager, supervisors, and adjuster. Their experiences will be helpful.
If a serious accident does occur, the top priority is to get medical care for the employee immediately. Call 911 or the EMS service that has been designated for transportation. When they arrive, verify the medical facility to which they will take the injured employee.
Next, contact the injured employee’s family/emergency contact to let them know what has happened and the medical facility where the employee has been taken. Arrange transportation for the family to the medical facility if they need it.
For the injured workers and their family members, it may be their first experience with an ICU, large emergency room, or trauma unit in a hospital. The facilities that treat catastrophic injures are generally large regional hospitals which might not be in the best areas of town or even in the employee’s hometown. Family members might not know where to park or how to find where the injured employee has been taken. The sights, sounds, and general busyness of trauma units can look chaotic and frightening to them.
The injured employees and their families will be afraid of what is ahead for them. They will be worried about how their family will survive financially and whether the injured employee will recover. They might not have the financial resources for temporary housing and restaurant meals. Employers should consider obtaining a pre-paid credit card to help the family stay close to the trauma center. This kindness will be remembered, will give the employer a sense that they were able to help in some way, and provide a measure of comfort to a family in shock.
After notifying the family, secure the accident scene for the investigation. The RTW coordinator and/or safety manager must notify multiple people: the risk management division and upper management, the insurance broker, agent, insurance carrier or self-insurance administrator, and the person who has the responsibility for reporting injuries to OSHA/TOSHA. The First Report of Injury needs to be completed as soon as possible, because there are many people who will need the information on the form.
Request the adjuster to immediately assign a catastrophic case manager with at least two or three years of catastrophic experience who will visit the hospital within 24-48 hours. Catastrophic injuries require advance medical knowledge of specific injuries (spinal cord, burns, traumatic amputation, brain injuries, etc.) and an understanding of complex family dynamics. They need a case manager who has existing relationships with local medical providers, experience with home modification, expertise on prosthetics, advanced durable medical equipment, and life-planning.
The case manager has a crucial role in a catastrophic injury and should become a trusted advocate for the injured employee, maintain cost effectiveness of the case, and be an excellent resource for all parties. During the first 48 hours the catastrophic case manager should do the following:
- Determine the severity, survivability, and potential long term limitations of the injured employee;
- Build rapport with the family and develop their needs assessment;
- Develop a rehabilitation plan and potential return to work assessment;
- Offer emotional support and reassurance;
- Begin discharge planning; and
- Provide education for both the family and employer on the injury and the road to recovery.
The RTW coordinator should review the needs identified by the case manager and determine the support the company and coworkers can provide. If the employee is being treated outside of his hometown, the employer might arrange for lodging near the hospital. Many hotels offer significant discounts for hospital patients’ families. The employer and/or fellow employees might drop off snacks or meals for the family while they are waiting in the ICU or the ER. Employees can sign up to help with lawn care while the employee is in the hospital. Coworkers can visit the employee and family while the employee is hospitalized and after they are discharged. If the employee has young children or elderly family members, look for options to help with their care so the spouse can visit the injured employee. Most ICUs, burn units, and Trauma Intensive Care Units (TICUs) do not allow children. Contact the employee’s place of worship to access their community outreach services, if available.
During the employee’s hospitalization and recovery, communication among all the parties is critical. Everyone should be kept in the information loop. When new information emerges about the injury, it should be communicated to everyone.
When it is time for the injured employee to be discharged from the hospital, the employer should not assume they will be permanently disabled. Employees who have had a catastrophic injury can return to work even though it is a much longer process. They might not be able to return to work in
the same position they held when they were injured, but many can return to meaningful work. The employer might have to be creative and make some reasonable accommodations for the employee, but the benefit can be priceless, and it is the right thing for the employer to do. Plus, the returning employee can be the best safety spokesperson for the company; it shows other employees why safety is so important.
If an employee has a catastrophic injury on the job, they should be treated with respect and dignity. Giving them a way to return to life and a purpose should be a common and shared goal of the company and society. Bringing back an employee who had a catastrophic injury shows the company’s employees that it takes care of its own.
REWARD Tool #11: Evaluation of a Return-to-Work Program
Evaluations of a return-to-work program should be conducted annually by staff who are knowledgeable about it. They should assess its strengths, weaknesses, opportunities, and threats.
Measure specified, quantifiable data points. Several examples include:
- The length of time from injury to return to work for injuries that occurred during the past 12 months, and for the 12 months before the year being analyzed.
- The number of injured employees during the past 12 months who had lost time claims and percentage decline from the prior 12 months.
- The total number of lost time hours in the past 12 months and for the 12 months before the year being analyzed.
- The total number of modified-duty (transitional) days provided to injured employees as a percentage of the prior 12 months and for the 12 months before the year being analyzed.
- The total cost of accommodations or modifications for injured employees and for the 12 months before the year being analyzed.
- The cost of workers’ compensation premiums for the year compared to the prior year, adjusted for changes in underwriting.
- Employee satisfaction with the RTW program, if applicable
Draw conclusions about the appropriateness and effectiveness of the RTW program from current-year data compared with the prior year.
Then, make improvements to the RTW program. Consider:
- The duration of modified duty currently allowed.
- The use of off-site modified duty programs, such as non-profits.
- Changes in the pool of physicians.
- Additional supervisor training.
These annual evaluations ensure that program objectives are consistently met and maintain the integrity and effectiveness of the RTW program.