Rural Health
Healthy People 2020 listed geographic location as one of their fourteen health disparities. Where you live and grow up has such a powerful impact on your health that some say your zip code is a greater determinant of your health and lifespan than your genetic code. The built environment varies widely between rural, suburban, and urban domains and, thus, has varying impacts on individual and community health depending on geographic location. The CDC characterizes the built environment as "all of the physical components of where we live and work." The built environment encompasses everything from housing and food availability to infrastructure like parks, roads, healthcare facilities, and vacant properties.
While rural populations might enjoy tight knit communities and idyllic landscapes, they are more at risk for health disparities. A study published in the Journal of the American Medical Association analyzed data from 1999 to 2019 and found that although overall mortality for Americans decreased, rural and urban populations did not benefit equally. During this same window, the mortality gap between large metropolitan areas and rural areas tripled. The study revealed a 12% increase in age adjusted mortality rates for rural populations between the ages of 25 to 64.
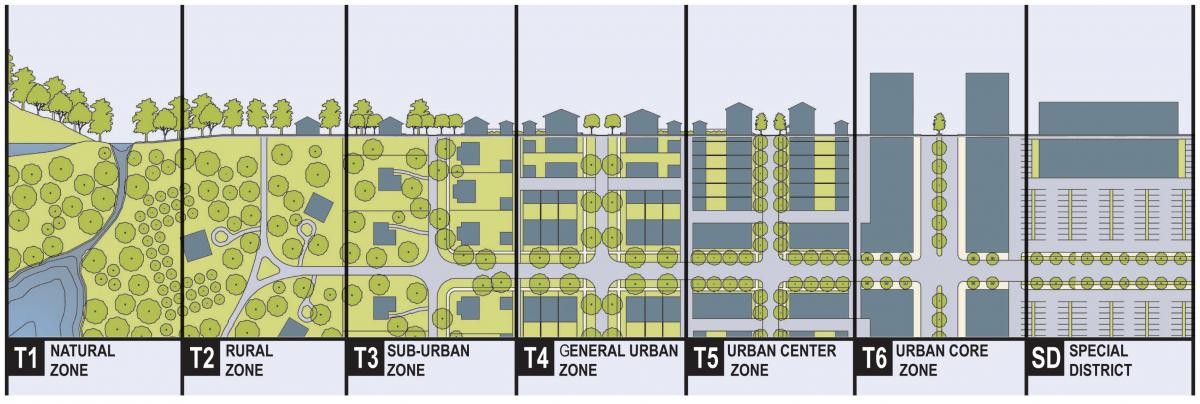
The Tennessee Vital Signs highlights 12 key metrics to measure the health and prosperity of the state. Some metrics, such as per capita income and access to greenways, may not be what we immediately think of when we think of health. However, they have significant impacts on health. Built environment interventions can address rural health concerns including upstream factors that cause health disparities. In “The Depth of Rural Health Disparities in America: the ABCDEs”, Drs. Florence, Southerland, Pack, and Wykoff presented their rural health identification tool, which includes:
(A) availability and access to health care
(B) behavioral patterns
(C) cultural influences
(D) determinants of socioeconomic origin
(E) environmental factors affecting health in rural areas.[1]
The interplay of these factors contribute to each community’s unique health outcome. Rural western and eastern Tennesseans experience unique health inequities, yet they face similar issues of access to health care, healthy foods, and opportunities for physical activity. As a result, it is necessary to understand the individual advantages and challenges that a region faces. The Urban Institute created an interactive map to visulize and propose interventions that work with the assets that the county already has to best address the challenges they are facing.
The majority of issues being faced in rural areas are the result of a lack of access to vital resources to maintain health. Here are some examples of access challenges in rural areas.
Geographic and socioeconomic challenges have resulted in the closure of many rural hospitals nationwide. In the last decade, more than 130 rural hospitals have closed. Tennessee accounts for 16 of the hospital closures and ranks second for the most hospital closures since 2005. Over a quarter of rural Tennessee counties lack a hospital, and 22 out of the 48 rural hospitals left in Tennessee are currently at risk of closing. Many already struggle to get care because of the time required or the costs of care; however, the divide in care has only continued to grow. 630 hospital beds have been lost, emergency care services are inaccessible, and patients are losing their primary care. [4]
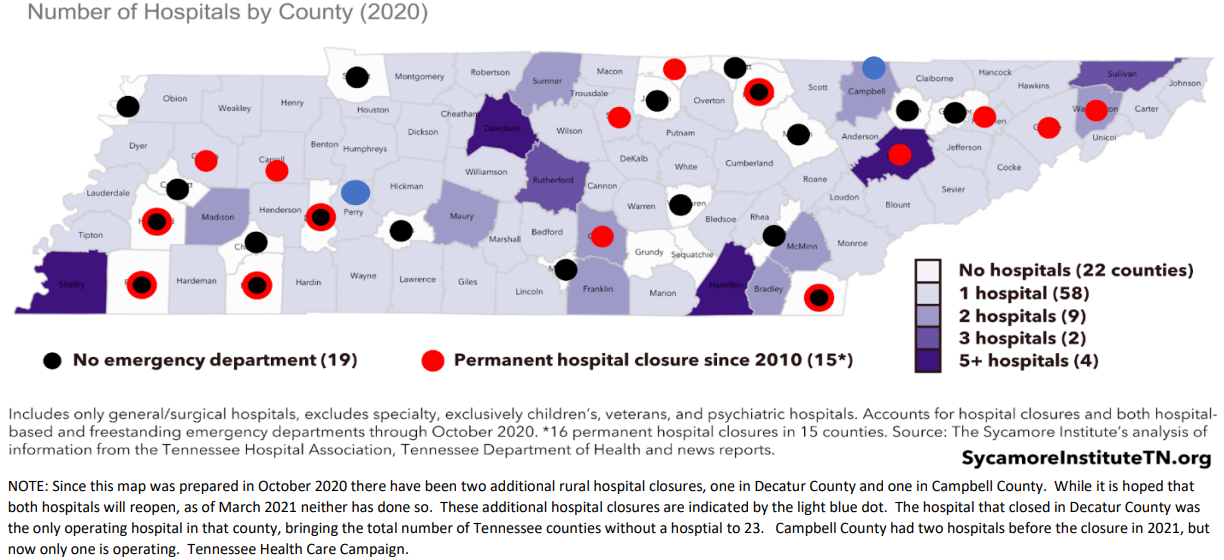
Much of our wellbeing dependends on investments in health in our communities. Urban areas often have surpluses of medical care and increased rates of access to employee sponsored insurance. On the other hand, rural Americans have lower rates of insurance coverage and when covered are relying on public options that do not provide the same accessibility to care. In rural areas, geographic isolation not only limits availability and accessibility to care, but it can discourage utilizing preventative care services such as routine cancer screenings and annual checkups. One reason is because of the increased cost, which includes the time and money required to travel to care as transportation options are limited. As a result, patients may only seek healthcare when an illness has advanced.
Areas where the rural hospitals have closed have experienced economic losses which also affect food. Food insecurity often affects those experiencing poverty and can compound health disparities, including associated risk of obesity. The southern region of the United States faces the greatest food insecurity nationally and within that, rural regions experience a greater rate of food insecurity. Many rural places are considered food deserts, as healthy options can be inaccessible and more expensive. New establishments in these areas are likely to be fast food restaurants that target lower income areas. The Tennessee Health Care Campaign within their Rural Equity Project stated that owners of fast-food restaurants in areas affected by a hospital closure saw a greater increase in dollar menu sales after the closure. Even when there is access to limited food options, there are still concerns of high food costs. A possible alternative is frozen and canned foods, which can provide greater security and tend to be less expensive than fresh food and healthier than fast food.
Active living begins with a culture and environment that supports health. It is currently recommended that individuals engage in 150 min of moderate-intensity or 75 min of vigorous-intensity physical activity a week. However, almost a third of rural populations do not engage in physical activity beyond work (Jones et. al. 2021). While the geographic isolation characteristic of rural regions may bring cleaner air, water, or land for some, this can result in losses to an individual’s ability to sustain a healthy lifestyle. For example, if road designs do not allow for safe biking or walking, an individual may need to rely on a personal car for transportation. This increases the amount of time they spend sedentary during the day. In these areas, there may not be public transportation, leading to further disparities between those who can afford and car and cannot. Furthermore, a reduced number of active living facilities and perceptions of an unsafe or inaccessible park result in even less opportunities to pursue physical activity. Rural areas also lack a “third location,” a place for someone to exist outside of their home or work. These places foster social connectivity and healthy minds. However, when nonresidential establishments do exist, they are unlikely to be free to the public, limiting accessibility.
While rural Americans have access to broadband now more than ever, they still may not enjoy the same technological advantages of their urban counterparts. Whether due to the local government or outside investors, rural regions do not have the same economic capacity to invest in faster and greater internet capabilities. As a result, rural populations have reduced access to job opportunities, such as remote jobs, and kids have less access to educational resources. This lack of access affects health in numerous ways. The internet is a powerful resource for individuals to understand and take authority over their own health. Access to the internet increases health literacy and understanding of diagnosis and medication. Furthermore, rural populations have less access to telehealth, which served a very important role during the COVID-19 pandemic. Telehealth is also an important resource to increase access to mental health services. Mental health resources must be as barrier-free as possible to be helpful, especially since rural populations face greater rates of mental illnesses and stigmatization.
Rural Americans have been experiencing a mental health crisis at higher rates with limited access to mental health resources. Social isolation, low socioeconomic status, and chronic health conditions are risks factors that many individuals in rural America face, especially within older populations. Day to day stressors from the family to economic instability, the workplace, or longer commutes can result in physical concerns such as higher risk of cardiovascular disease, weight gain, and immune suppression. However, an even greater concern is mental health that is left unaddressed because of social stigma, cost, or lack of available treatment. Living in a state of constant stress is living in constant survival mode. When mental health crises are left untreated, the effects of it continue to harm the individual. The National Alliance on Mental Illness states, “untreated mental health conditions can result in unnecessary disability, unemployment, substance abuse, homelessness, inappropriate incarceration, and suicide, and poor quality of life.” In fact, half of all people that have had mental illnesses have also experience substance misuse. When treatment is unavailable, people will look to other means to cope or self-medicate.
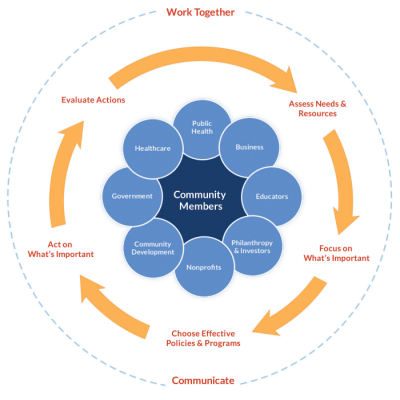
The greatest priority for rural public health is investing in and empowering rural communities. Issues of access are the result of the lack of investment in the community and are exacerbated when individuals lack the economic or physical capacity to create a culture of health. Geographic isolation has meant that these regions were not able to keep up with the technological advances that allowed urban regions to develop. Rural regions now experience disparities in capital and economic capacities for development.
Mistrust in government intervention in addition to medical and public health interventions is prevalent among rural populations. As a result, it is necessary to embrace community engagement for interventions within the region to garner the greatest success. These are strong communities that know what needs to be improved but may lack access to the tools to take action. Whereas a needs assessment can be used to identify where interventions should be targeted; an Asset Based Community Development model can be used to mobilize sustainable interventions that enrich and work with the community. The Appalachian Service Project is a volunteer-based group that provides free home improvements to substandard housing, including ramps, insulation, and ceilings. These improvements provide better access to physical and mental health by reducing exposure to cold weather and black mold or by providing a new sense of comfort in the home. Revitalizing homes and lives can extend to revitalizing communities, downtown spaces, and local businesses.
The most critical intervention for rural health is increasing access to healthcare for rural populations. The Tennessee Center for Workforce Development offers the Residency Incentive Program, which provides $35,000 a year to residents who commit to practicing in underserved populations. Furthermore, state and federally sponsored loan repayment programs are available to practitioners located in Health Professional Shortage Areas. However, increasing access can only provide so much benefit when there is still the economic barrier to healthcare. Rural Americans do not have equal access to insurance programs, and policies often provide limited coverage at higher costs compared to urban counties. Interventions could include bringing low cost or free service to a community. Project Rural Recovery provides physical and behavioral health treatment to rural counties across middle and east Tennessee. In its first two years, Project Rural Recovery has served more than 1,600 Tennesseans. Additionally, providing accessible transportation opportunities like senior or care share shuttles can reduce the burden of seeking care.
With any action, it is valuable to reach out to community leaders and organizations when creating or expanding opportunities related to health. These key stakeholders are vital in creating a culture of health.
“About Mental Illness.” NAMI California, 26 July 2021, https://namica.org/what-is-mental-illness/#:~:text=Without%20treatment%2C%20the%20consequences%20of,and%20poor%20quality%20of%20life.
Alfero, Charlie, et al. "Insuring rural America: Health insurance challenges and opportunities." (2018).
Bolin, Jane N., et al. "Rural healthy people 2020: new decade, same challenges." The Journal of Rural Health 31.3 (2015): 326-333.
Cross, Sarah H., Robert M. Califf, and Haider J. Warraich. "Rural-Urban disparity in mortality in the US from 1999 to 2019." JAMA 325.22 (2021): 2312-2314.
Jones, Natalie, et al. "Physical activity barriers and assets in rural Appalachian Kentucky: a mixed-methods study." International journal of environmental research and public health 18.14 (2021): 7646.
Lister, Jamey J., and Paul J. Joudrey. "Rural mistrust of public health interventions in the United States: A call for taking the long view to improve adoption." The Journal of Rural Health (2022).
National Institute on Drug Abuse. "Common comorbidities with substance use disorders." (2018).
Pack, James E. Florence Robert P., Jodi Southerland, and Randolph F. Wykoff. "The Depth of Rural Health Disparities in America." Rural Populations and Health: Determinants, Disparities, and Solutions (2012): 51.
“Rural Hospital Closures.” Tennessee Health Care Campaign, Tennessee Health Care Campaign, Mar. 2021, https://tnhealthcarecampaign.org/wp-content/uploads/2021/03/ToolKIT-Final-Draft-3-16-2021-1.pdf.
Tennessee Department of Economic & Community Development (ECD)
www.tn.gov/ecd.html
Tennessee Department of Agriculture (Ag)
tn.gov/agriculture
U.S. Department of Agriculture (USDA)
Rural Development, natural resource conservation
rd.usda.gov
U.S. Department of Health & Human Services, Health Resources and Services Administration (HRSA)
Federal Office of Rural Health Policy
www.hrsa.gov/ruralhealth
U.S. Environmental Protection Agency (EPA)
Smart Growth in Small Towns and Rural Communities
www.epa.gov/smartgrowth/smart-growth-small-towns-and-rural-communities
Rural Health Association of Tennessee
www.rhat.org
Tennessee Center for Workforce Development
tncwd.com
Rural Health Information Hub
www.ruralhealthinfo.org/states/tennessee
Center for Rural Strategies
www.ruralstrategies.org
The Land Trust for Tennessee
landtrusttn.org
Tennessee Recreation and Parks Association
Benefits of Parks and Recreation
www.trpa.net
National Agricultural Library
What is Rural?
https://www.nal.usda.gov/rural-development-and-communities/what-is-rural
For comments or suggestions concerning this web content, please contact Mariagorathy Okonkwo at mariagorathy.n.okonkwo@tn.gov.