Electronic Billing and Payment Companion Guide
This document was adapted with permission from the IAIABC Workers’ Compensation Electronic Billing and Payment National Companion Guide, release 2.3. The IAIABC companion guide is a template for jurisdictions to use to create their own guide and is based upon X12 005010 and NCPDP D.0.
Important Notes
- Assistance requests and documentation error reporting should be made to the IAIABC at 608- 841-2017 or www.iaiabc.org.
- The IAIABC companion guide was reviewed and approved by the X12 Intellectual Property (IP) Committee prior to publication. X12 has granted the IAIABC authority to review jurisdictions’ eBill companion guides that are based on the IAIABC template and to extend their permission to reproduce materials to those documents. Jurisdictions that customize this eBill companion guide to reflect their jurisdictional eBill requirements must submit their draft companion guide to the IAIABC for review and approval. Tennessee has completed this process. Future changes will be reflected as further explained below in Appendix C. The page, the section and the effective date of any changes will be tracked therein.
- This companion guide is the product of consensus. The IAIABC makes no warranties regarding the fitness for any purpose of any resource, product or service that is mentioned within the guide and assumes no responsibility for consequential damages resulting from the use or reliance thereupon.
© Copyright 2014 International Association of Industrial Accident Boards and Commissions (IAIABC). All rights reserved.
No part of this document may be copied or reproduced in any form without written permission of the IAIABC.
Attestation of Approval from IAIABC
On behalf of the IAIABC and the eBill Implementation Team, I am pleased to provide our approval of the Tennessee Bureau of Workers’ Compensation Electronic Billing and Payment Companion Guide dated 12/19/2017. - Gregg Lutz, IAIABC Director of Standards Development and Outreach
Purpose of the Electronic Billing and Payment Companion Guide
This guide has been created for use in conjunction with the X12 ( X12) Technical Reports Type 3 and the National Council for Prescription Drug Programs (NCPDP) Telecommunication Standard Implementation Guide Version D.0 national standard implementation guides adopted under the Health Insurance Portability and Accountability Act of 1996 (HIPAA). These national standard implementation guides are incorporated by reference. The Tennessee Companion Guide is not to be a replacement for those national standard implementation guides but rather is to be used as an additional source of information. This companion guide contains data clarifications derived from specific business rules that apply to processing bills and payments electronically within the Tennessee workers’ compensation system.
Documentation Change Control
The companion guide content is subject to change.
Documentation change control is maintained in this document through the use of the Change Control Table shown in Appendix C. Each change made to this companion guide after the creation date is noted, along with the date and reason for the change.
Tennessee Companion Guide Contact Information:
Tennessee Bureau of Workers’ Compensation
Address:
220 French Landing Drive, Suite 1-B
Nashville, TN 37243
Attn: Electronic Billing
Telephone Number: (615) 741-2395
Fax Number: (615) 253-1223
Email Address: WC.eBill@tn.gov
Methodology for Updating Companion Guide Document
Please contact the Tennessee Bureau of Workers’ Compensation above regarding instructions for submitting change requests, recommendations, and document updates. Such requests will be directed to the IAIABC for consideration.
Table of Contents
- Introduction and Overview
- Tennessee Bureau of Workers’ Compensation Requirements
- Compliance
- National Standard Formats
- Companion Guide Usage
- Description of X12 Transaction Identification Numbers
- Claim Administrator Validation Edits
- Description of Formatting Requirements
- Description of X12 Transmission/Transaction Dates
- Description of Code Sets
- Participant Roles
- Health Care Provider Agent/Claim Administrator Agent Roles
- Duplicate, Appeal/Reconsideration, and Corrected Bill Resubmissions
- Tennessee and Workers' Compensation Specific Requirements
- Companion Guide X12N/005010X222A1 Health Care Claim: Professional (837)
- Companion Guide X12N/005010X223A2 Health Care Claim: Institutional (837)
- Companion Guide X12N/005010X224A2 Health Care Claim: Dental (837)
- Companion Guide NCPDP D.0 Pharmacy
- Companion Guide X12N/005010X221A1 Health Care Claim Payment/Advice (835) and Electronic Funds Transfer (EFT)
- Purpose, Applicability and Expected Implementation Date
- Trading Partner Agreements
- Claim Adjustment Group Codes
- Claim Adjustment Reason Codes
- Remittance Advice Remark Codes
- 6 X12 Technical Report Type 2 Health Care Claim Payment/ AdviceCode Usage Rules (TR2)
- Electronic Funds Transfer (EFT) and Electronic Remittance Advice (ERA) Operating Rules
- Claim Level Jurisdictional Explanation of Review (EOR) or Explanation of Benefit (EOB)Statement ID Qualifier
- Line Level Reason Code ID Qualifier and URL Reference
- Product/Service ID Qualifier
- Workers’ Compensation Health Care Claim Payment/Advice Instructions
- Companion Guide X12N/005010X210 Additional Information to Support a Health Care Claim or Encounter (275)
- Companion Guide Acknowledgments
Appendix A - Glossary of Terms
Appendix B - Jurisdictional Report Type Codes and Tennessee Descriptions
Chapter 1 | Introduction and Overview
1.1 HIPAA
The Administrative Simplification Act provisions of the Federal Health Insurance Portability and Accountability Act of 1996 (HIPAA, Title II) include requirements that national standards for electronic health care transactions and national identifiers for Health Care Providers (Provider), Health Plans, and Employers be established. These standards were adopted to improve the efficiency and effectiveness of the nation's health care system by encouraging the widespread use of electronic data interchange in health care. Additional information regarding the formats adopted under HIPAA is included in Chapter 2.
1.2 Tennessee Law
Tennessee Code Annotated §50-6-202 mandates that payers accept electronic bills for medical goods and services. This companion guide attempts to establish electronic billing rules that are as consistent with HIPAA as possible. The health care provider, health care facility, or third-party biller/assignee shall use the HIPAA-adopted electronic transaction formats to submit medical or pharmacy bills to the appropriate claim administrator associated with the employer of the injured employee to whom the services are provided.
In workers’ compensation, the payer is the claim administrator providing coverage for the employer of the injured employee to whom the services are provided. The claim administrator, or its authorized agent, is to validate the Electronic Data Interchange (EDI) file according to the guidelines provided in the prescribed national standard format implementation guide, this companion guide, and the jurisdictional data requirements. Problems associated with the processing of the X12 Health Care Claim (837) EDI file are to be reported using acknowledgment transactions described in this companion guide. Problems associated with the processing of the NCPDP Telecommunication D.0 bills are reported via the reject response transactions described in this companion guide. The claim administrator will use the HIPAA-adopted electronic transaction formats to report explanations of payments, reductions, and denials to the health care provider, health care facility, or third-party biller/assignee. These electronic transaction formats include the X12N/005010X221A1, Health Care Claim Payment/Advice (835), and the NCPDP Telecommunication D.0 Paid response transaction.
Health care providers, health care facilities, or third-party biller/assignees, claim administrators, clearinghouses, or other electronic data submission entities shall use this guideline in conjunction with the HIPAA-adopted X12 Technical Reports Type 3 (implementation guides) and the NCPDP Telecommunication Standard Implementation Guide Version D.0. The X12 Technical Reports Type 3 (implementation guides) can be accessed by contacting the Accredited Standards Committee ( ) X12, http://store.x12.org. The NCPDP Telecommunication Standard Implementation Guide Version D.0 is available from NCPDP at www.ncpdp.org.
This guide outlines jurisdictional procedures necessary for engaging in Electronic Data Interchange (EDI) and specifies clarifications where applicable. When coordination of a solution is required, Tennessee Bureau of Workers’ Compensation will work with the IAIABC EDI Medical Committee and Provider to Payer Subcommittee to coordinate with national standard setting organizations and committees to address workers’ compensation needs.
Chapter 2 | Tennessee Bureau of Workers’ Compensation Requirements
2.1 Compliance
If a billing entity is not granted an exception from mandatory participation from submitting bills electronically, it must also be able to receive an electronic response from the claim administrator. The electronic responses include electronic acknowledgments and electronic remittance advices (Explanation of Review).
Electronic billing rules allow for providers and claim administrators to use agents to meet the requirement of electronic billing, but these rules do not mandate the method of connectivity, or the use of, or connectivity to, clearinghouses or similar types of vendors.
Nothing in this document prevents the parties from utilizing Electronic Funds Transfer (EFT) to facilitate payment of electronically submitted bills. Use of EFT is required under Rule 0800-02-26-.05 (6) (b) unless the payer and provider agreed to an alternate electronic method of payment.
Health care providers, health care facilities, third-party biller/assignees, and claim administrators must be able to exchange electronic bills in the prescribed standard formats and may exchange data in non-prescribed formats by mutual agreement. All jurisdictionally-required data content must be present in mutually agreed upon formats.
2.1.1 Agents
Electronic billing rules allow for health care providers and claim administrators to use agents to accomplish the requirement of electronic billing.
Claim administrators and health care providers are responsible for the acts or omissions of their agents.
2.1.2 Privacy, Confidentiality, and Security
Health care providers, health care facilities, third-party biller/assignees, claim administrators, and their agents must comply with all applicable Federal and Tennessee Acts, Codes, or Rules related to the privacy, confidentiality, security or similar issues.
2.2 National Standard Formats
The national standard formats for billing, remittance, and acknowledgments are those adopted by the Federal Department of Health and Human Services rules (45 CFR Parts 160 and 162). The formats adopted under 0800-02-26 that are aligned with the current Federal HIPAA implementation include:
- X12N/005010X222A1 Health Care Claim: Professional (837);
- X12N/005010X223A2 Health Care Claim: Institutional (837);
- X12N/005010X224A2 Health Care Claim: Dental (837);
- X12N/005010X221A1 Health Care Claim Payment/Advice (835);
- X12N/005010X212 Health Care Claim Status Request and Response (276/277);
- X12N005010TA1 Interchange Acknowledgment;
- X12C005010X231 Implementation Acknowledgment for Health Care Insurance (999);
- X12N005010X214 Health Care Claim Acknowledgment (277);
- NCPDP Telecommunication Standard Implementation Guide Version D.0; and
- NCPDP Batch Standard Implementation Guide 1.2.
These acknowledgment formats and the attachment format have not been adopted in the current HIPAA rules but are also based on X12 standards.
- The X12N/005010X213 Request for Additional Information (277) is used to request additional attachments that were not originally submitted with the electronic medical bill.
- The X12N/005010X210 Additional Information to Support a Health Care Claim or Encounter (275) is used to transmit electronic documentation associated with an electronic medical bill. The 005010X210 can accompany the original electronic medical bill, or may be sent in response to a 005010X213 Request for Additional Information.
The NCPDP Telecommunication Standard Implementation Guide Version D.0 contains the corresponding request and response messages to be used for pharmacy transactions.
2.2.1 Tennessee Bureau of Workers’ Compensation Prescribed Formats
| Format | Corresponding Paper Form | Function |
|---|---|---|
| 005010X222A1 | CMS-1500 | Professional Billing |
| 005010X223A2 | UB-04 | Institutional/Hospital Billing |
| 005010X224A2 | ADA-2006 | Dental Billing |
| NCPDP D.0 and Batch 1.2 | NCPDP WC/PC UCF | Pharmacy Billing |
| 005010X221A1 | None | Explanation of Review (EOR) |
| TA1 005010 | None | Interchange Acknowledgment |
| 005010X231 | None | Transmission Level Acknowledgment |
| 005010X214 | None | Bill Acknowledgment |
2.2.2 X12 Ancillary Formats
Other formats not adopted by Tennessee Bureau of Workers’ Compensation rule are used in ancillary processes related to electronic billing and reimbursement. The use of these formats is voluntary, and the companion guide is presented as a tool to facilitate their use in workers’ compensation.
| Format | Corresponding Process | Function |
|---|---|---|
| 005010X210 | Documentation/Attachments | Documentation/Attachments |
| 005010X212 | Health Claim Status Request and Response | Medical Bill Status Request and Response |
| 005010X213 | Request for Additional Information | Request for Medical Documentation |
2.3 Companion Guide Usage
Tennessee Bureau of Workers’ Compensation implementation of the national standard formats aligns with HIPAA usage and requirements in most circumstances. This jurisdictional companion guide is intended to convey information that is within the framework of the X12 Technical Reports Type 3 (Implementation Guides) and NCPDP Telecommunication Standard Implementation Guide Version D.0 adopted for use. The jurisdictional companion guide is not intended to convey information that in any way exceeds the requirements or usages of data expressed in the X12 Technical Reports Type 3 (Implementation Guides) or NCPDP Telecommunication Standard Implementation Guide Version D.0. The jurisdictional companion guide, where applicable, provides additional instruction on situational implementation factors that are different in workers’ compensation than in the HIPAA implementation.
When the workers’ compensation application situation needs additional clarification or a specific code value is expected, the companion guide includes this information in a table format. Shaded rows represent “segments” in the X12 Technical Reports Type 3 (Implementation Guides). Non-shaded rows represent “data elements” in the X12 Technical Reports Type 3 (Implementation Guides). An example is provided in the following table:
| Loop | Segment or Element | Value | Description | Tennessee Bureau of Workers’ Compensation Instructions |
|---|---|---|---|---|
| 2000B | SBR | Subscriber Information | In workers’ compensation, the Subscriber is the Employer. | |
| SBR04 | Group or Plan Name | Required when the Employer Department Name/Division is applicable and is different than the Employer reported in Loop 2010BA NM103. | ||
| SBR09 | WC | Claim Filing Indicator Code | Value must be ‘WC’ to indicate workers’ compensation bill. |
Detailed information explaining the various components of the use of loops, segments, data elements, and conditions can be found in the appropriate X12 Technical Reports Type 3 (Implementation Guides).
The X12 Technical Reports Type 3 (Implementation Guides) also include elements that do not relate directly to workers’ compensation processes, for example, coordination of benefits. If necessary, the identification of these loops, segments, and data elements can be described in the trading partner agreements to help ensure efficient processing of standard transaction sets.
2.4 Description of X12 Transaction Identification Numbers
The X12 Transaction Identification requirements are defined in the appropriate X12 Technical Reports Type 3 (Implementation Guides), available through the Accredited Standards Committee X12, http://store.x12.org. The Tennessee Bureau of Workers’ Compensation has provided the following additional information regarding transaction identification number requirements.
2.4.1 Sender/Receiver Trading Partner Identification
Workers’ compensation standards require the use of the Federal Employer Identification Number (FEIN) or other mutually agreed upon identification numbers to identify Trading Partners (sender/receiver) in electronic billing and reimbursement transmissions. Trading Partners will exchange the appropriate and necessary identification numbers to be reported based on the applicable transaction format requirements.
2.4.2 Claim Administrator Identification
Claim administrators and their agents are also identified through the use of the FEIN or other mutually agreed upon identification number. Claim administrator information is available through direct contact with the claim administrator. The Claim Administrator Identification information is populated in Loop 2010BB for 005010X222A1, 005010X223A2, and 005010X224A2 transactions.
Health care providers will need to obtain payer identification information from their connectivity trading partner agent (i.e. clearinghouses, practice management system, billing agent and/or other third party vendor) if they are not directly connecting to a claim administrator.
2.4.3 Health Care Provider Identification
Health Care Provider roles and identification numbers are addressed extensively in the X12 Technical Reports Type 3 (Implementation Guides). However, it is noted that in the national transaction sets most health care providers are identified by the National Provider Identification number, and secondary identification numbers are generally not transmitted.
2.4.4 Injured Employee Identification
The injured employee is identified by (Social Security Number), date of birth, date of injury, and workers’ compensation claim number (see below).
The injured employee’s (patient’s) Identification Number is submitted using the Property and Casualty Patient Identifier REF segment in Loop 2010CA.
2.4.5 Claim Identification
The workers’ compensation claim number assigned by the claim administrator is the claim identification number for purposes of electronic bill processes. This claim identification number is reported in the REF segment of Loop 2010CA, Property and Casualty Claim Number.
The X12N Technical Report Type 3 (Implementation Guides) instructions for the Property and Casualty Claim Number REF segments require the health care provider, health care facility, or third-party biller/assignee to submit the claim identification number in the 005010X222A1, 005010X223A2 and 005010X224A2 transactions.
2.4.6 Bill Identification
The X12N Technical Report Type 3 (Implementation Guides) refers to a bill as a “claim” for electronic billing transactions. This companion guide refers to these transactions as “bills” because in workers’ compensation, a “claim” refers to the full case for a unique injured employee and injury.
The health care provider, health care facility, or third-party biller/assignee, assigns a unique identification number to the electronic bill transaction. For 005010X222A1, 005010X223A2, and 005010224A2 transactions, the bill transaction identification number is populated in Loop 2300 Claim Information CLM Health Claim segment CLM01 Claim (Bill) Submitter’s Identifier data element. This standard HIPAA implementation allows for a patient account number but strongly recommends that submitters use a completely unique number for this data element on each individual bill.
2.4.7 Document/Attachment Identification
The 005010X210 is the standard electronic format for submitting electronic documentation and is addressed in a later chapter of this Tennessee Bureau of Workers’ Compensation companion guide.
Documentation to support electronic medical bills may be submitted by facsimile (fax), electronic mail (email), electronic transmission using the prescribed format, or by a mutually agreed upon format. Documentation related to an electronic bill must identify the following elements:
- Patient name (ill or injured worker)
- Date of birth (if available)
- Employer name
- Insurer name
- Date of service
- Claim number (if no claim number, use “UNKNOWN”)
- Unique attachment indicator number
- The PWK segment and the associated documentation identify the type of documentation through the use of X12 standard Report Type Codes. The PWK segment and the associated documentation also identify the method of submission of the documentation through the use of X12 Report Transmission Codes.
- A unique Attachment Indicator Number shall be assigned to all documentation. The Attachment Indicator Number populated on the document shall include the Report Type Code, the Report Transmission Code, the Attachment Control Qualifier (AC) and the Attachment Control Number. For example, operative note (report type code OB) sent by fax is identified as OBFXAC12345. The combination of these data elements will allow a claim administrator to appropriately match the incoming attachment to the electronic medical bill.
- In situations when the documentation represents a Jurisdictional Report, the provider uses code value ‘OZ’ (Support Data for Claim) as the Report Type Code in PWK01 and enters the Jurisdictional Report Type Code (e.g. J1=Doctor First Report) in front of the Attachment Control Number. Example: OZFXACJ199923 in PWK06.
- If sending preauthorization supporting documentation for treatment authorization use PWK 01 Report Type Qualifier CT = certification.
- Please refer to Appendix B for a list of Jurisdictional Report Type Codes and associated Tennessee Bureau of Workers’ Compensation report type code descriptions.
2.5 Claim Administrator Validation Edits
Claim administrators may refer to various sources for the validation edits they apply to electronic bills received from providers. Sources for validation edits may include:
- The IAIABC Medical Bill/Payment Records Implementation Guide,
- X12N Technical Reports Type 3 (Implementation Guides) requirements, or
- Medicare coding and billing policies when applicable.
Claim administrators use the 005010X214 transaction, referred to in this companion guide as an Acknowledgment, to communicate transaction (individual bill) rejections for X12-based electronic medical bills. Error rejection codes are used to indicate the reason for the transaction rejection.
2.6 Description of Formatting Requirements
The X12 formatting requirements are defined in the X12 Technical Reports Type 3 (Implementation Guides), Appendices B.1, available through the Accredited Standards Committee X12, http://store.x12.org. The Tennessee Bureau of Workers’ Compensation has provided the following additional information regarding formatting requirements:
The NCPDP Telecommunication D.0 formatting requirements are defined in the NCPDP Telecommunication Standard Implementation Guide Version D.0, available at http://www.ncpdp.org.
2.6.1 X12 Hierarchical Structure
For information on how the X12 Hierarchical Structure works, refer to Section 2.3.2 HL segment of the X12 Technical Reports Type 3 (Implementation Guides), available through the Accredited Standards Committee X12, http://store.x12.org.
2.7 Description of X12 Transmission/Transaction Dates
The X12 required Transmission/Transaction Dates are defined in the X12 Technical Reports Type 3 (Implementation Guides) available through the Accredited Standards Committee ( ) X12, http://store.x12.org. The Tennessee Bureau of Workers’ Compensation has provided additional information regarding specific transmission/transaction identification requirements.
2.7.1 Date Sent/Invoice Date
In the manual paper medical bill processing model, the paper bill includes a date the bill was generated, to verify timely filing. For electronic billing, the Invoice Date is the Date Sent, which is reflected in the Interchange Control Header ISA segment Interchange Date. The date in the Interchange Control Header ISA segment must be the actual date the transmission is sent.
2.7.2 Date Received
For medical bill processing purposes, the Date Received is the date the claim administrator or its agent systematically received the transaction. Other dates included in the electronic transaction or outer envelope (e.g. Interchange Control Header ISA segment Interchange Date, Business Application Creation Date) are often the same as the actual date systematically received, but based on processing delays, intermediary connections, or other automated handling by the submitter or the submitter agent, those dates are not considered as the Date Received because they may not be current. The Date Received is used to track timely processing of electronic bills, electronic reconsideration/appeal transactions, acknowledgment transactions, and timeliness of payments.
2.7.3 Paid Date
When the 005010X221A1 transaction set is used to electronically provide the remittance advice, the Paid Date is the date contained in BPR16, “Check Issue or EFT Effective Date,” in the BPR Financial Information segment.
2.8 Description of Code Sets
Code sets utilized in electronic billing and reimbursement and other ancillary processes are prescribed by the applicable X12 Technical Reports Type 3 (Implementation Guides), NCPDP Implementation Guide, Tennessee Bureau of Workers’ Compensation rule, and this companion guide. The code sets are maintained by multiple standard setting organizations.
Participants are required to utilize current valid codes based on requirements contained in the applicable implementation guide. The validity of the various codes may be based on the date of service (e.g., procedure and diagnosis codes) or based on the date of the electronic transaction (e.g., claim adjustment reason codes).
2.9 Participant Roles
Roles in the HIPAA implementation guides are generally the same as in workers’ compensation. The Employer, Insured, Injured Employee, and Patient are roles that are used differently in workers’ compensation and are addressed later in this section.
2.9.1 Trading Partner
Trading Partners are entities that have established EDI relationships and that exchange information electronically either in standard or mutually agreed-upon formats. Trading Partners can be both Senders and Receivers, depending on the electronic process involved (i.e. Billing or Acknowledgment).
2.9.2 Sender
A Sender is the entity submitting a transmission to the Receiver, or its Trading Partner. The health care provider, health care facility, or third-party biller/assignee, is the Sender in the 005010X222A1, 005010X223A2 and 005010X224A2 electronic billing transactions. The claim administrator, or its agent, is the Sender in the 005010X214, 005010X231 or 005010X221A1 electronic acknowledgment or remittance transactions.
2.9.3 Receiver
A Receiver is the entity that accepts a transmission submitted by a Sender. The health care provider, health care facility, or third-party biller/assignee, is the Receiver in the 005010X214, 005010X231 or 005010X221A1 electronic acknowledgment or remittance transactions. The claim administrator, or its agent, is the Receiver in the 005010X222A1, 005010X223A2, and 005010X224A2 electronic billing transactions.
2.9.4 Employer
The Employer, as the policyholder of the workers’ compensation insurance coverage, is considered the Subscriber in the workers’ compensation implementation of the HIPAA electronic billing and reimbursement formats.
2.9.5 Subscriber
The subscriber or insured is the individual or entity that purchases or is covered by an insurance policy. In this implementation, the workers’ compensation insurance policy is obtained by the Employer, who is considered the Subscriber.
2.9.6 Insured
The insured or subscriber is the individual or entity that purchases or is covered by an insurance policy. In group health, the insured may be the patient, the spouse or the parent of the patient. In this workers' compensation implementation, the Employer is considered the insured entity.
2.9.7 Injured Employee
In workers' compensation, the Injured Employee, as the person who has been injured on the job or has a work related illness, is always considered to be the patient. In group health, there are many relationships a patient may have to the insured. For example, the patient may be the insured, or may be the child or spouse of the insured.
2.9.8 Patient
The patient is the person receiving medical services. In the workers’ compensation implementation of electronic billing and reimbursement processes, the patient is considered the Injured Employee.
2.10 Health Care Provider Agent/Claim Administrator Agent Roles
Electronic billing and reimbursement rules include provisions that allow for providers and claim administrators to utilize agents to comply with the electronic billing (eBill) requirements. Billing agents, third party administrators, bill review companies, software vendors, data collection agents, and clearinghouses are examples of companies that may have a role in eBill. Entities using agents are responsible for the acts or omissions of their agents executed in the performance of services for the entity.
Under the eBill rules, claim administrators must be able to exchange medical billing and reimbursement information electronically with health care providers. Claim administrators may establish direct electronic connections to health care providers or may use agents to perform eBill functions. The rules do not mandate the use of, or regulate the costs of, agents performing eBill functions. Providers and claim administrators are not required by Tennessee Bureau of Workers’ Compensation rule to establish connectivity with a clearinghouse or to utilize a specific media/method of connectivity (i.e. Secured File Transfer Protocol [SFTP]).
By mutual agreement, use of non-standard formats between the health care provider, health care facility, or third-party biller/assignee and the claim administrator is permissible.
The eBill rules do not regulate the formats utilized between providers and their agents, or claim administrators and their agents, or the method of connectivity between those parties.
2.11 Duplicate, Appeal/Reconsideration, and Corrected Bill Resubmissions
2.11.1 Claim (Corrected Bill) Resubmission Code - 837 Billing Formats
Health care providers will identify resubmissions of prior medical bills (not including duplicate original submissions) by using the Claim Frequency Type Code of 7 (Resubmission/Replacement). The value is populated in Loop 2300 Claim Information CLM Health Claim segment CLM05-3 Claim Frequency Type Code of the 005010X222A1, 005010X223A2 and 005010X224A2 electronic billing transactions. When the payer has provided the Payer Claim Control Number it had assigned to the previous bill, the health care provider must use this number when the bill is replaced. This information is populated in Loop 2300 Claim Information REF Payer Claim Control Number of the 005010X222A1, 005010X223A2 and 005010X224A2 electronic billing transactions.
On electronically submitted medical bills, health care providers must also populate the appropriate NUBC Condition Code to identify the type of resubmission. Condition codes provide additional information to the claim administrator when the resubmitted bill is a request for reconsideration or a new submission after receipt of a decision from the Tennessee Bureau of Workers’ Compensation Medical Payment Committee or, if appealed, the order resolving the contested case hearing or other administrative proceeding, such as a judicial review. Based on the instructions for each bill type, the Condition Code is submitted in the HI segment for 005010X222A1 and 005010X223A2 transactions and in the NTE segment for the 005010X224A2 transaction. (The use of the NTE segment is at the discretion of the sender.)
The NUBC Instruction for the use of Claim Frequency Type Codes can be referenced on the NUBC website at http://www.nucc.org/index.php/code-sets-mainmenu-41/condition-codes-mainmenu-38
The CMS-required bill processing documentation for adjustments can be referenced at http://www.cms.hhs.gov/manuals/downloads/clm104c01.pdf.
2.11.2 Duplicate Bill Transaction Prior To Payment
A Condition Code ‘W2’ (Duplicate of the original bill) is required when a provider submits a bill that is a duplicate. The Condition Code is submitted based on the instructions for each bill type. It is submitted in the HI segment for professional and institutional transactions and in the NTE segment for dental transactions. (The use of the NTE segment is at the discretion of the sender.) The duplicate bill must be identical to the original bill, with the exception of the added Condition Code. No new dates of service or itemized services may be included on the duplicate bill.
Duplicate Bill Transaction
- • CLM05-3 = Identical value as original. Cannot be ‘7’.
- Condition codes in HI/K3 are populated with a condition code qualifier ‘BG’ and code value: ‘W2’ = Duplicate.
- NTE Example: NTE*ADD*BGW2
- Payer Claim Control Number does not apply.
- The resubmitted bill must be identical to the original bill, except for the ‘W2’ condition code. No new dates of service or itemized services may be included on the duplicate bill.
Duplicate bill transactions shall be submitted no earlier than thirty (30) working days after the claim administrator has acknowledged receipt of a complete electronic bill transaction and prior to receipt of a 005010X221A1 transaction.
The claim administrator may reject a bill transaction with a Condition Code ‘W2’ indicator if
- the duplicate bill is received within thirty (30) working days after acknowledgment,
- the bill has been processed and the 005010X221A1 transaction has been generated, or
- the claim administrator does not have a corresponding accepted original transaction with the same bill identification numbers.
If the claim administrator does not reject the duplicate bill transaction within two business days, the duplicate bill transaction may be denied for the reasons listed above through the use of the 005010X221A1 transaction.
2.11.3 Corrected Bill Transactions
A replacement bill is sent when a data element on the original bill was either not previously sent or needs to be corrected.
When identifying elements change, the correction is accomplished by a void and re-submission process: a bill with CLM05-3 = ‘8’ (Void) must be submitted to cancel the incorrect bill, followed by the submission of a new original bill with the correct information.
Billers must not replace or void a prior bill until that prior submitted bill has reached final adjudication status, which can be determined from the remittance advice, a web application, when showing a finalized code under Claim Status Category in the 277, or by non-electronic means.
Corrected Bill Transaction
- CLM05-3 = ‘7’ indicates a replacement bill.
- Condition codes of ‘W2’ to ‘W5’ in HI/K3 are not used.
- REF*F8 includes the Payer Claim Control Number, if assigned by the payer.
- A corrected bill shall include the original dates of service and the same itemized services rendered as the original bill.
- When identifying elements change, the correction is accomplished by a void and re-submission process. A bill with CLM05-3 = ‘8’ (Void) must be submitted to cancel the incorrect bill, followed by the submission of a new original bill with the correct information.
The claim administrator may reject a revised bill transaction if
- the claim administrator does not have a corresponding adjudicated bill transaction with the same bill identification number, or
- there is incorrect billing documentation for an adjustment based on CMS guidelines (inappropriate changed data).
If the claim administrator does not reject the revised bill transaction within two business days, the revised bill transaction may be denied for the reasons listed above through the use of the 005010X221A1 transaction.
2.11.4 Appeal/Reconsideration Bill Transactions
Electronic submission of Reconsideration transactions is accomplished in the 005010X222A1, 005010X223A2, and 005010X224A2 electronic billing transactions through the use of Claim Frequency Type Code ‘7’ in Loop 2300 Claim Information CLM Health Claim segment CLM05-3 Claim Frequency Type Code. The value ‘7’ Replacement of a Prior Claim represents Resubmission transactions.
The Reconsideration Claim Frequency Type Code ‘7’ is used in conjunction with the Payer Claim Control Number assigned to the bill by the claim administrator when the payer has provided this number in response to the previous bill submission. This information is populated in Loop 2300 Claim Information REF Payer Claim Control Number of the 005010X222A1, 005010X223A2, and 005010X224A2 electronic billing transactions.
The health care provider must also populate the appropriate condition code to identify the type of resubmission on electronically submitted medical bills. The NUBC Condition Codes which apply to reconsiderations and appeals include:
- 'W3' – 1st Level Appeal Request for reconsideration or appeal with the payer. Resolution at this level may entail several reconsideration\\ appeal communications as specified in Rule 0800-02-17. This level appeal must be exhausted before proceeding to the next level.
- 'W4' – 2nd Level Appeal Resubmitted after receipt of a decision on the merits from the Bureau of Workers’ Compensation Medical Payment Committee. E-bill process is not used for this appeal. At this level, paper documents are filed with the Medical Payment Committee pending a decision.
- 'W5' – 3rd Level Appeal Resubmitted after receipt of order following a contested case hearing or further judicial appeal. E-bill process is not used for this appeal.
At this level, paper documents are filed with the Bureau Administrative Hearing Clerk pending a contested case hearing before an administrative law judge.
These codes are included in the 2300/HI segment on professional and institutional claims, and in the 2300/NTE segment on dental claims. (Note: the use of the NTE segment is at the discretion of the sender.)
Reconsideration bill transactions may only be submitted after receipt of the 005010X221A1 transaction for the corresponding accepted original bill or 15 calendar days after the claim administrator acknowledged receipt of a complete electronic medical bill when no 005010X221A1 transaction has been received. Reconsideration bill transactions shall be submitted by the provider, and processed by the claim administrator in accordance with Tennessee Bureau of Workers’ Compensation Rules 0800-02-17-.13, 0800-02-18-.15, 0800-02-19-.06, 0800-02-01-.10 or TCA 50-6-125 as applicable. The same bill identification number is used on both the original and the Reconsideration bill transaction to associate the transactions. All elements, fields, and values in the Reconsideration bill transaction, except the Reconsideration-specific qualifiers and the Claim Supplemental Information PWK segment, must be the same as on the original bill transaction. Subsequent Reconsideration bill transactions related to the same original bill transaction may be submitted after receipt of the 005010X221A1 transaction corresponding to the initial Reconsideration bill transaction. Subsequent Reconsideration bill transactions shall not be submitted prior to 30 calendar days from the date the original request for reconsideration was sent or after the claim administrator has taken final action on the reconsideration request.
Corresponding documentation related to an appeal/reconsideration is required in accordance with the Tennessee Bureau of Workers’ Compensation rules for initial bill submission. The PWK segment (Claim Supplemental Information) is required to be properly annotated when submitting an attachment related to an appeal/reconsideration.
The X12 Technical Reports Type 3 (Implementation Guides) and the Tennessee Bureau of Workers’ Compensation recommend that the value passed in CLM01 represent a unique identification number specific to the bill transaction, the Provider Unique Bill Identification Number. The Tennessee Bureau of Workers’ Compensation eBilling implementation uses the Provider Unique Bill Identification Number (CLM01) to link the original bill to the subsequent bill transaction. The intent is to link an appeal, or multiple subsequent appeals, to a single original bill transaction.
The X12 Technical Reports Type 3 (Implementation Guides) include a Reference Identification Number REF segment in Loop 2300 Claim Information that represents the Payer Claim Control Number, which is the unique transaction identification number generated by the claim administrator. This number must be included on resubmitted bills to ensure that the payer can match the resubmission request with its original processing action.
Appeal/Reconsideration Bill Transaction
- CLM05-3 = ‘7’;
- Condition codes in HI/NTE are populated with a condition code qualifier ‘BG’ and one of the following codes values must be present:
- ‘W3’ = 1st Level Appeal - Request for reconsideration or appeal with the payer
- ‘W4’ = 2nd Level Appeal - Resubmitted after receipt of a decision on the merits from the Medical Payment Committee. See description above.
- ‘W5’ = 3rd Level Appeal - Resubmitted after receipt of order following a contested case hearing or further judicial appeal. See description above.
- Condition codes in HI/NTE are populated with a condition code qualifier ‘BG’ and one of the following codes values must be present:
- REF*F8 includes the Payer Claim Control Number, if assigned by the payer.
- The appeal/reconsideration bill must be identical to the original bill, with the exception of the added Condition Code, Payer Claim Control Number, and the Claim Frequency Type Code. No new dates of service or itemized services may be included on the appeal/reconsideration bill.
- Supporting documentation is required.
- Loop 2300, PWK segment must be properly annotated.
The claim administrator may reject an appeal/reconsideration bill transaction if:
- the bill information does not match the corresponding original bill transaction;
- the claim administrator does not have a corresponding accepted original transaction;
- the original bill transaction has not been completed (no corresponding 005010X221A1 transaction or the Remittance submission Jurisdiction-allowed time period has not been exceeded);or
- the bill is submitted without the PWK annotation.
Corresponding documentation related to appeals/reconsideration is required in accordance with the Jurisdiction rules for initial bill submission.
The claim administrator may deny appeal/reconsideration bill transactions for missing documentation. If the claim administrator does not reject the appeal/reconsideration bill transaction within two business days because it is incomplete, the bill transaction may be denied through the use of the 005010X221A1 transaction for the reasons of missing documentation as well as other data content problems with the 837.
2.12 Tennessee Bureau of Workers’ Compensation and Workers’ Compensation Specific Requirements
The requirements in this section identify Tennessee Bureau of Workers’ Compensation workers’ compensation specific requirements that apply to more than one electronic format. Requirements that are related to a specific format are identified in the chapter related to that format.
2.12.1 Claim Filing Indicator
The Claim Filing Indicator code for workers’ compensation is ‘WC’ populated in Loop 2000B Subscriber Information, SBR Subscriber Information segment field SBR09 for the 005010X222A1, 005010X223A2, or 005010X224A2 transactions.
2.12.2 Transaction Set Purpose Code
The Transaction Set Purpose Code in the Transaction Set Header BHT Beginning of Hierarchical Transaction segment field BHT02 in 005010X222A1, 005010X223A2, or 005010X224A2 transactions is designated as ‘00’ Original. Claim administrators are required to acknowledge acceptance or rejection of transmissions (files) and transactions (bills). Transmissions that are rejected by the claim administrator and then corrected by the provider are submitted, after correction, as ‘00’ Original transmissions.
2.12.3 Transaction Type Code
The Transaction Type Code in the Transaction Set Header BHT Beginning of Hierarchical Transaction segment field BHT06 in 005010X222A1, 005010X223A2, or 005010X224A2 transactions is designated as ‘CH’ Chargeable. Currently, health care providers are not required to report electronic billing data to the Tennessee Bureau of Workers’ Compensation. Therefore, code ‘RP’ (Reporting) is not appropriate for this implementation.
2.12.4 Other State Data Requirements
Reserved
2.12.5 NCPDP Telecommunication Standard D.0 Pharmacy Formats
Issues related to electronic pharmacy billing transactions are addressed in Chapter 6 Companion Guide NCPDP
D.0 Pharmacy.
Chapter 3 | Companion Guide X12N/005010X222A1 Health Care Claim: Professional (837)
3.1 Introduction and Overview
The information contained in this companion guide has been created for use in conjunction with the X12N/005010X222A1 Health Care Claim: Professional (837) Technical Report Type 3. It is not to be considered a replacement for the X12N/005010X222A1 Health Care Claim: Professional (837) Technical Report Type 3, but rather is to be used as an additional source of information.
The X12N/005010X222A1 Health Care Claim: Professional (837) Technical Report Type 3 is available through the Accredited Standards Committee ( ) X12, http://store.x12.org.
3.2 Trading Partner Agreements
The data elements transmitted as part of a trading partner agreement must, at a minimum, contain all the same required data elements found within the X12 Technical Reports Type 3 and the jurisdiction-specific companion guide. The trading partner agreement must not change the workers’ compensation field value designations as defined in the jurisdiction-specific companion guide.
3.3 Workers’ Compensation Health Care Claim: Professional Instructions
The following table identifies the application/instructions for Tennessee workers’ compensation that need clarification beyond the X12 Technical Report Type 3.
| Loop | Segment | Description | IAIABC Companion Guide Workers’ Compensation Comments or Instructions |
|---|---|---|---|
| 1000A | PER | SUBMITTER EDI CONTACT INFORMATION | One occurrence of the Communication Number Qualifier must be ‘TE’ – Telephone Number. |
| 2000B | SBR | SUBSCRIBER INFORMATION | In workers' compensation, the Subscriber is the Employer. |
| 2000B | SBR04 | NAME | In workers’ compensation, the group name is the employer of the patient/employee. |
| 2000B | SBR09 | CLAIM FILING INDICATOR CODE | Value must be 'WC' for workers’ compensation. |
| 2010BA | SUBSCRIBER NAME | In workers' compensation, the Subscriber is the Employer. | |
| 2010BA | NM102 | ENTITY TYPE QUALIFIER | Value must be '2' non-person. |
| 2010BA | NM103 | NAME LAST OR ORGANIZATION NAME | Value must be the name of the Employer. |
| 2000C | PAT01 | INDIVIDUAL RELATIONSHIP CODE | Value must be '20' Employee. |
| 2010CA | REF | PROPERTY AND CASUALTY CLAIM NUMBER | When the workers’ compensation claim number is not assigned or is not available, use “UNKNOWN” as the default value. The claim number is required when assigned by the insurer. |
| 2010CA | REF | PROPERTY AND CASUALTY PATIENT IDENTIFIER | Required |
| 2010CA | REF01 | REFERENCE IDENTIFICATION QUALIFIER | Value must be “SY” |
| 2010CA | REF02 | REFERENCE IDENTIFICATION | Value must be the patient’s Social Security Number. When applicable, utilize ‘999999999’ as a default value where the social security number is not known. |
| 2300 | CLM11 | RELATED CAUSES INFORMATION | One of the occurrences in CLM11 must have a value of ‘EM’ -- Employment Related. |
| 2300 | DTP | DATE – ACCIDENT | Required when the condition reported is for an occupational accident/injury. |
| 2300 | DTP | DATE – DISABILITY DATES | Do not use this segment. |
| 2300 | DTP | DATE – PROPERTY AND CASUALTY DATE OF FIRST CONTACT | Do not use this segment. |
| 2300 | PWK | CLAIM SUPPLEMENTAL INFORMATION | Required when submitting attachments related to a medical bill. |
| 2300 | PWK01 | REPORT TYPE CODE | Value must be 'OZ' when report is a Jurisdictional Report. For all other reports, use appropriate 005010 Report Type Code. |
| 2300 | PWK06 | ATTACHMENT CONTROL NUMBER | When the Report Type Code is ‘OZ’ and a Jurisdiction report is sent, the first two characters of the attachment control number must be the Jurisdictional Report Type Code. Examples: Standard Report: PWK*OB*BM***AC*DMN0012~ Jurisdictional Report: PWK*OZ*FX***J1*ACDMN0012~ |
| 2300 | K3 | FILE INFORMATION | State Jurisdictional Code |
| 2300 | K301 | FIXED FORMAT INFORMATION | Jurisdiction State Code (TN). Value must be the state code qualifier ‘LU’ followed by the two alpha character state code. For example, ‘LUTN’ indicates the medical bill is being submitted under Tennessee medical billing requirements. |
| 2300 | HI | CONDITION INFORMATION | For workers’ compensation purposes, the National Uniform Billing Committee and the National Uniform Claims Committee have approved the following condition codes for resubmissions: W2 - Duplicate of the original bill W3 - Level 1 Appeal W4 - Level 2 Appeal W5 - Level 3 Appeal Note: Do not use condition codes when submitting revised or corrected bills. (See section 2.11) |
| 2310B | PRV | RENDERING PROVIDER SPECIALTY INFORMATION | Not applicable |
| 2400 | K3 | FILE INFORMATION | Not applicable in Tennessee at this time. Refer to Medical Fee Schedule Rules for re-packaging. |
| 2400 | K301 | FIXED FORMAT INFORMATION | Not applicable in Tennessee at this time. |
| 2410 | LIN | DRUG IDENTIFICATION | Not applicable in Tennessee at this time. |
| 2420A | PRV | RENDERING PROVIDER SPECIALTY INFORMATION | Not applicable in Tennessee at this time. |
Chapter 4 | Companion Guide X12N/005010X223A2 Health Care Claim: Institutional (837)
4.1 Introduction and Overview
The information contained in this companion guide has been created for use in conjunction with the X12N/005010X223A2 Health Care Claim: Institutional (837) Technical Report Type 3. It is not a replacement for the X12N/005010X223A2 Health Care Claim: Institutional (837) Technical Report Type 3, but rather is an additional source of information.
The X12N/005010X223A2 Health Care Claim: Institutional (837) Technical Report Type 3 is available through the Accredited Standards Committee ( ) X12, http://store.x12.org.
4.2 Trading Partner Agreements
The data elements transmitted as part of a trading partner agreement must, at a minimum, contain all the same required data elements found within the X12 Technical Reports Type 3 and the this companion guide. The workers’ compensation field value designations as defined in this companion guide must remain the same as part of any trading partner agreement.
4.3 Workers’ Compensation Health Care Claim: Institutional Instructions
Instructions for Tennessee specific requirements are also provided in Tennessee Workers’ Compensation Requirements. The following table identifies the application/instructions for Tennessee workers’ compensation that need clarification beyond the X12 Technical Reports Type 3.
| Loop | Segment | Description | IAIABC Companion Guide Workers’ Compensation Comments or Instructions |
|---|---|---|---|
| 1000A | PER | SUBMITTER EDI CONTACT INFORMATION | One occurrence of the Communication Number Qualifier must be ‘TE’ – Telephone Number. |
| 2000B | SBR | SUBSCRIBER INFORMATION | In workers' compensation, the Subscriber is the Employer. |
| 2000B | SBR04 | NAME | In workers’ compensation, the group name is the employer of the patient/employee. |
| 2000B | SBR09 | CLAIM FILING INDICATOR CODE | Value must be 'WC' for workers’ compensation. |
| 2010BA | SUBSCRIBER NAME | In workers' compensation, the Subscriber is the Employer. | |
| 2010BA | NM102 | ENTITY TYPE QUALIFIER | Value must be '2' non-person. |
| 2010BA | NM103 | NAME LAST OR ORGANIZATION NAME | Value must be the name of the Employer. |
| 2000C | PAT01 | INDIVIDUAL RELATIONSHIP CODE | Value must be '20' Employee. |
| 2010CA | REF02 | PROPERTY CASUALTY CLAIM NUMBER | When the workers’ compensation claim number is not assigned or is not available, use “UNKNOWN” as the default value. The claim number is required when assigned by the insurer. |
| 2010CA | REF | PROPERTY AND CASUALTY PATIENT IDENTIFIER | Required. |
| 2010CA | REF01 | REFERENCE IDENTIFICATION QUALIFIER | Value must be ‘SY’. |
| 2010CA | REF02 | REFERENCE IDENTIFICATION | Value must be the patient’s Social Security Number. When applicable, utilize ‘999999999’ as a default value where the social security number is not known |
| 2300 | PWK | CLAIM SUPPLEMENTAL INFORMATION | Required when submitting attachments related to a bill. |
| 2300 | PWK01 | REPORT TYPE CODE | Value must be 'OZ' when report is a Jurisdictional Report. For all other reports, use appropriate 005010 Report Type Code. |
| 2300 | PWK06 | ATTACHMENT CONTROL NUMBER | When the Report Type Code is ‘OZ’ and a Jurisdiction report is sent, the first two characters of the attachment control number must be the Jurisdictional Report Type Code. Examples: Standard Report: PWK*OB*EL***AC*DMN0012~ Jurisdictional Report: PWK*OZ*EL***AC*J1DMN0012~ |
| 2300 | K3 | FILE INFORMATION | State Jurisdictional Code is expected here. |
| 2300 | K301 | FIXED FORMAT INFORMATION | Tennessee State Code (State of Compliance Code) Value must be the state code qualifier ‘LU’ followed by the two alpha character state code. “LUTN” |
| 2300 | HI01 | OCCURRENCE INFORMATION | At least one Occurrence Code must be entered with a value of '04' - Accident/Employment Related or ‘11’ - Illness. The Occurrence Date must be the Date of Occupational Injury or Illness. |
| 2300 | HI | CONDITION INFORMATION | For workers’ compensation purposes, the National Uniform Billing Committee and the National Uniform Claims Committee has approved the following condition codes for resubmissions: • W2 - Duplicate of the original bill • W3 - Level 1 Appeal • W4 - Level 2 Appeal • W5 - Level 3 Appeal Note: Do not use condition codes when submitting revised or corrected bills. |
Chapter 5 | Companion Guide X12N/005010X224A2 Health Care Claim: Dental (837)
5.1 Purpose, Introduction and Overview
The information contained in this companion guide has been created for use in conjunction with the X12N/05010X224A2 Health Care Claim: Dental (837) Technical Report Type 3. It is not a replacement for the X12N/05010X224A2 Health Care Claim: Dental (837) Technical Report Type 3, but rather is an additional source of information.
This companion guide is not, nor was it ever intended to be, a comprehensive guide to the electronic transaction requirements for each of the jurisdictions. The companion guide is intended to be used by jurisdictions to develop and publish companion guides tailored to their regulatory environment that consistently apply the syntactical requirements of the X12 Technical Reports Type 3.
The X12N/05010X224A2 Health Care Claim: Dental (837) Technical Report Type 3 is available through the Accredited Standards Committee ( ) X12, http://store.x12.org.
5.2 Trading Partner Agreements
The data elements transmitted as part of a trading partner agreement must, at a minimum, contain all the same required data elements found within the X12 Technical Reports Type 3 and this companion guide. The workers’ compensation field value designations as defined in this companion guide must remain the same as part of any trading partner agreement.
5.3 Workers’ Compensation Health Care Claim: Dental Instructions
Instructions for Tennessee specific requirements are also provided in Tennessee Workers’ Compensation Requirements. The following table identifies the application/instructions for Tennessee workers’ compensation that need clarification beyond the X12 Technical Report Type 3.
| Loop | Segment | Description | IAIABC Companion Guide Workers’ Compensation Comments or Instructions |
|---|---|---|---|
| 1000A | PER | SUBMITTER EDI CONTACT INFORMATION | One occurrence of the Communication Number Qualifier must be ‘TE’ – Telephone Number.” |
| 2000B | SBR | SUBSCRIBER INFORMATION | In workers' compensation, the Subscriber is the Employer. |
| 2000B | SBR04 | NAME | In workers’ compensation, the group name is the employer of the patient/employee. |
| 2000B | SBR09 | CLAIM FILING INDICATOR CODE | Value must be 'WC' for workers’ compensation. |
| 2010BA | SUBSCRIBER NAME | In workers' compensation, the Subscriber is the Employer. | |
| 2010BA | NM102 | ENTITY TYPE QUALIFIER | Value must be '2' non-person. |
| 2010BA | NM103 | NAME LAST OR ORGANIZATION NAME | Value must be the name of the Employer. |
| 2000C | PAT01 | INDIVIDUAL RELATIONSHIP CODE | Value must be '20' Employee. |
| 2010CA | REF02 | PROPERTY CASUALTY CLAIM NUMBER | When the workers’ compensation claim number is not assigned or is not available, use “UNKNOWN” as the default value. The claim number is required when assigned by the insurer. |
| 2300 | CLM11 | RELATED CAUSES INFORMATION | One of the occurrences in CLM11 must have a value of ‘EM’ -- Employment Related. |
| 2010CA | REF | PROPERTY AND CASUALTY PATIENT IDENTIFIER | Required |
| 2010CA | REF01 | REFERENCE IDENTIFICATION QUALIFIER | Value must be ‘SY’.. |
| 2010CA | REF02 | REFERENCE IDENTIFICATION | Value must be the patient’s Social Security Number. When applicable, utilize ‘999999999’ as a default value when the social security number is not known |
| 2300 | DTP | DATE -- ACCIDENT | Required when the condition reported is for an occupational accident/injury. |
| 2300 | PWK | CLAIM SUPPLEMENTAL INFORMATION | Required when submitting attachments related to a medical bill. |
| 2300 | PWK01 | REPORT TYPE CODE | Value must be 'OZ' when report is a Jurisdictional Report. For all other reports use appropriate 005010 Report Type Code. |
| 2300 | PWK06 | ATTACHMENT CONTROL NUMBER | When the Report Type Code is ‘OZ’ and a Jurisdiction report is sent, the first two characters of the attachment control number must be the Jurisdictional Report Type Code. Examples: Standard Report: PWK*OB*EL***AC*DMN0012~ Jurisdictional Report: PWK*OZ*EL***AC*J1DMN0012~ |
| 2300 | K3 | FILE INFORMATION | State jurisdictional code is expected here. |
| 2300 | K301 | FIXED FORMAT INFORMATION | Jurisdiction State Code (State of Compliance Code) Value must be the state code qualifier ‘LU’ followed by the two alpha character state code. For example, ‘LUTN’ indicates the medical bill is being submitted under Tennessee medical billing requirements. |
Chapter 6 | Companion Guide NCPDP D.0 Pharmacy
6.1 | Purpose Introduction and Overview
The information contained in this companion guide has been created for use in conjunction with the NCPDP Telecommunication Standard Implementation Guide Version D.0 for pharmacy claim transactions. It is not a replacement for the NCPDP Telecommunication Standard Implementation Guide Version D.0, but rather is an additional source of information.
Pharmacy transactions are processed both in real-time and via batch. Every transmission request has a transmission response. To address the appropriate process for responding to request transactions and reversal processing, users are directed to utilize the NCPDP Telecommunication Standard Implementation Guide Version D.0 and Batch Standard Implementation Guide Version 1.2.
This companion guide is not, nor was it ever intended to be, a comprehensive guide to the electronic transaction requirements for each of the jurisdictions. The companion guide is intended to be used by jurisdictions to develop and publish companion guides tailored to their regulatory environment that consistently apply the syntactical requirements of the NCPDP Implementation Guide.
The implementation guide for electronic pharmacy claims and responses is available through the National Council for Prescription Drug Programs (NCPDP) at http://www.ncpdp.org.
6.2 Trading Partner Agreements
The data elements transmitted as part of a trading partner agreement must, at a minimum, contain all the same required data elements found within the NCPDP Implementation Guide and the jurisdiction-specific companion guide. The workers’ compensation field value designations as defined in the jurisdiction-specific companion guide must remain the same as part of any trading partner agreement.
6.3 Workers’ Compensation NCPDP Pharmacy Claim Instructions
The following table identifies the application/instructions for Tennessee workers’ compensation that need clarification beyond the NCPDP Telecommunication Standard Implementation Guide Version D.0.
| Segment | Field | Description | IAIABC Companion Guide Workers’ Compensation Comments or Instructions |
|---|---|---|---|
| INSURANCE | 3Ø2-C2 | CARDHOLDER ID | If the Cardholder ID is not available or not applicable, the value must be ‘NA’. |
| CLAIM | 415-DF | NUMBER OF REFILLS AUTHORIZED | Required. If no refills this value must be ‘0’. |
| PRICING | 426-DQ | USUAL AND CUSTOMARY CHARGE | This field is optional. In Tennessee, the fees are subject to the Medical Fee Schedule. |
| PHARMACY PROVIDER | 465-EY | PROVIDER ID QUALIFIER | : The value must be ‘05’ – NPI Number. |
| PRESCRIBER | 466-EZ | PRESCRIBER ID QUALIFIER | The value must be ‘01’ – NPI Number. |
| WORKERS’ COMPENSATION | The Workers’ Compensation segment is required for workers’ compensation claims. | ||
| WORKERS’ COMPENSATION | 435-DZ | CLAIM/REFERENCE ID | When the workers’ compensation claim number is not assigned or is not available, use “UNKNOWN” as the default value. The claim number is required when assigned by the insurer. |
Chapter 7 | Companion Guide X12N/005010X221A1 Health Care Claim Payment/Advice (835) and Electronic Funds Transfer (EFT)
7.1 Introduction and Overview
The information contained in this companion guide has been created for use in conjunction with the X12N/005010X221A1 Health Care Claim Payment Advice (835) Technical Report Type 3. It is not a replacement for the X12N/005010X221A1 Health Care Claim Payment Advice (835) Technical Report Type 3, but rather is an additional source of information.
This companion guide is not, nor was it ever intended to be, a comprehensive guide to the electronic transaction requirements for each of the jurisdictions. The companion guide is intended to be used by jurisdictions to develop and publish companion guides tailored to their regulatory environment that consistently apply the syntactical requirements of the X12 Technical Reports Type 3.
The X12N/005010X221A1 Health Care Claim Payment Advice (835) Technical Report Type 3 is available through the Accredited Standards Committee ( ) X12, http://store.x12.org.
The NCPDP X12N 835 (005010X221) Pharmacy Remittance Advice Template, is available at https://www.ncpdp.org/Resources/X12N-835-Payment-Guidance-and-Related-Documents-NC
Electronic submission and processing of medical bills relating to workers’ compensation is required by Tennessee Code Annotated §50-6-202.
7.2 Trading Partner Agreements
The components of trading partner agreements that define other transaction parameters beyond the ones described in this companion guide (such as transmission parameters) remain the same; this companion guide is not intended to replace any of those components.
The data elements transmitted as part of a trading partner agreement must at a minimum contain all the same required data elements found within the X12 Technical Reports Type 3 and this companion guide. The workers’ compensation field value designations as defined in this companion guide must remain the same as part of any trading partner agreement.
Trading partner agreements must follow the X12TR2 Health Care Claim Payment/Advice Code Usage Rules (TR2) that specify the specific Group Code, Claim Adjustment Reason Code, and Remittance Advice Remark Code combinations that are to be used when providing payment, reduction, or denial information. The TR2 is available at www.wpc-edi.com.
7.3 Claim Adjustment Group Codes
The 005010X221A1 transaction requires the use of Claim Adjustment Group Codes. The most current valid codes must be used as appropriate for workers’ compensation. The Claim Adjustment Group Code represents the general category of payment, reduction, or denial. For example, the Group Code ‘CO’ (Contractual Obligation) might be used in conjunction with a Claim Adjustment Reason Code for a network contract reduction.
The Claim Adjustment Group Code transmitted in the 005010X221A1 transaction is the same code that is transmitted in the IAIABC 837 Medical State Reporting EDI reporting format. Tennessee accepts Claim Adjustment Group Codes that were valid on the date the claim administrator paid or denied a bill.
7.4 Claim Adjustment Reason Codes
The 005010X221A1 transaction requires the use of Claim Adjustment Reason Codes (CARC) as the electronic means of providing specific payment, reduction, or denial information. As a result, use of the 005010X221A1 transaction eliminates the use of proprietary reduction codes, Jurisdiction specific Claim Adjustment Reason Codes, and free form text used on paper Explanation of Review (EOR) forms. Claim Adjustment Reason Codes are available through Washington Publishing Company at http://www.wpc-edi.com/codes.
7.5 Remittance Advice Remark Codes
The 005010X221A1 transaction supports the use of Remittance Advice Remark Codes to provide supplemental explanations for a payment, reduction, or denial already described by a Claim Adjustment Reason Code. NCPDP Reject Codes are allowed for NCPDP transactions. Claim administrators must use the Remittance Advice Remark Codes to provide additional information to the health care provider regarding why a bill was adjusted or denied. The use of the 005010X221A1 transaction eliminates the use of proprietary reduction codes and free form text used on paper Explanation of Review (EOR) forms. Remittance Advice Remark Codes are not associated with a Group or Reason Code in the same manner that a Claim Adjustment Reason Code is associated with a Group Code. Remittance Advice Remark Codes are available through Washington Publishing Company at http://www.wpc-edi.com/codes.
7.6 X12 Technical Report Type 2 Health Care Claim Payment/ Advice Code Usage Rules (TR2)
The X12 Technical Report Type 2 Health Care Claim Payment/Advice Code Usage Rules (TR2) is the encyclopedia of Group Codes, specific Claim Adjustment Reason Codes (CARC) and Remittance Advice Remark Codes (RARC) combinations, for payers to use when providing bill payment, reduction, or denial information. These codes, and their combinations, are defined, maintained, modified, and/or deleted by the X12 External Code Committees and CMS Remittance Advice Remark Committee, which meets every three months. The TR2 has a specific Workers’ Compensation CARC and RARC defined usage section that shall be used to explain a claim denial or adjustment in the 005010x221A1 transaction. The TR2 is available at www.wpc-edi.com.
The great variability in the mapping and combinations of codes used in both the health care and property and casualty industries today results in different interpretations by the providers for each payer. The TR2 workers’ compensation section defines CARC/RARC combinations that provide a concrete and predictable message, thereby allowing providers to set up rules to automate actions based upon the combinations of codes. Consistent use of these codes by all payers will result in significant administrative simplification, especially in the workers’ compensation industry.
In the event that a jurisdiction requires its specific CARC and/or RARC codes to be used in electronic billing, it should contact the IAIABC EDI Medical Committee for assistance in submitting its codes to the External Code Committees and/or CMS Remittance Advice Remark Committee for inclusion in the national code sets.
7.7 Electronic Funds Transfer (EFT) and Electronic Remittance Advice (ERA) Operating Rules
The Patient Protection and Affordable Care Act (ACA) defines operating rules as, “the necessary business rules and guidelines for the electronic exchange of information that are not defined by a standard or its implementation specifications.” By Rule 0800-02-26-.05 (6)(b),Tennessee has adopted the following ACA mandated EFT and ERA Operating Rules (effective January 1, 2014) for eBill payment processing:
- CAQH CORE 370 ERA EFT (CCD+) Reassociation Rule;
- CAQH CORE 380: EFT Enrollment Data Rule; and
- CAQH CORE 382: ERA Enrollment Data Rule.
7.8
This section is not applicable in Tennessee at this time.
7.9
This section is not applicable in Tennessee at this time.
7.10 Product/Service ID Qualifier
The Product/Service Identification Number transmitted in the inbound electronic billing format is returned in the 005010X221A1 transaction SVC Service Payment Information segment with the appropriate qualifier.
7.11 Workers’ Compensation Health Care Claim Payment/Advice Instructions
The following table identifies the application/instructions for Tennessee workers’ compensation requirements that need clarification beyond the X12 Technical Reports Type 3.
| Loop | Segment or Element | Value | Description | IAIABC Companion Guide Workers’ Compensation Comments or Instructions |
|---|---|---|---|---|
| 1000A | PER | Payer Technical Contact Information | ||
| PER03 | TE | Communication Number Qualifier | Value must be ‘TE’ Telephone Number. | |
| PER04 | Communication Number | Value must be the Telephone Number of the submitter. | ||
| 2100 | CLP | Claim Level Data | ||
| CLP06 | WC | Claim Filing Indicator Code | Value must be “WC” – Workers’ Compensation. | |
| CLP07 | Payer Claim Control Number | The payer- assigned claim control number for workers’ compensation use is the bill control number. | ||
| 2100 | REF | Other Claim Related Identification | Not applicable in Tennessee | |
| REF01 | CE | Reference Identification Qualifier | ||
| REF02 | Reference Identification | |||
| 2110 | REF | Healthcare Policy Identification | Not applicable in Tennessee | |
| REF01 | 0K | Reference Identification Qualifier | ||
| REF02 | Reference Identification | |||
Chapter 8 | Companion Guide X12N/005010X210 Additional Information to Support a Health Care Claim or Encounter (275)
8.1 Introduction and Overview
The information contained in this companion guide has been created for use in conjunction with the X12N/005010X210 Additional Information to Support a Health Care Claim or Encounter (275) Technical Report Type 3. It is not a replacement for the X12N/005010X210 Additional Information to Support a Health Care Claim or Encounter (275) Technical Report Type 3, but rather is an additional source of information.
This companion guide is not, nor was it ever intended to be, a comprehensive guide to the electronic transaction requirements for each of the jurisdictions. The companion guide is intended to be used by jurisdictions to develop and publish companion guides tailored to their regulatory environment that consistently apply the syntactical requirements of the X12N Technical Reports Type 3.
The X12N/005010X210 Additional Information to Support a Health Care Claim or Encounter (275) Technical Report Type 3 is available through the Accredited Standards Committee ( ) X12, http://store.x12.org.
8.2 Method of Transmission
The 005010X210 transaction is the recommended standard electronic format for submitting electronic documentation in workers' compensation. Health care providers, health care facilities, or third party biller/assignees and claim administrators may agree to exchange documentation in other non-prescribed electronic formats (such as uploading to a web-based system) by mutual agreement. If trading partners mutually agree to use non-prescribed formats for the documentation they exchange, they must include all components required to identify the information associated with the documentation.
Health care providers, health care facilities, or third party biller/assignees and claim administrators may also elect to submit documentation associated with electronic bill transactions through other ways, i.e.., secure fax, secure Web upload, or secure e-mail. Health care providers, health care facilities, or third party biller/assignees and claim administrators must be able to electronically exchange medical documentation that is required to be submitted with the bill based on the regulatory requirements found in Rule 0800-02-17.
8.3 Documentation Requirements
“Medical documentation” includes, but is not limited to, medical reports and records, such as evaluation reports, narrative reports, assessment reports, progress report/notes, clinical notes, hospital records, and diagnostic test results. Documentation requirements for Tennessee workers’ compensation billings are defined Rule 0800-02-17.
Chapter 9 | Companion Guide Acknowledgments
There are several different acknowledgments that a clearinghouse and/or payer may use to respond to the receipt of a bill. The purpose of these acknowledgments is to provide feedback on the following:
1. Basic file structure and the trading partner information from the Interchange Header.
2. Detailed structure and syntax of the actual bill data as specified by the X12 standard.
3. The content of the bill against the Jurisdictional complete bill rules.
4. Any delays caused by claim number indexing/validation.
5. Any delays caused by attachment matching.
6. The outcome of the final adjudication, including re-association to any financial transaction.
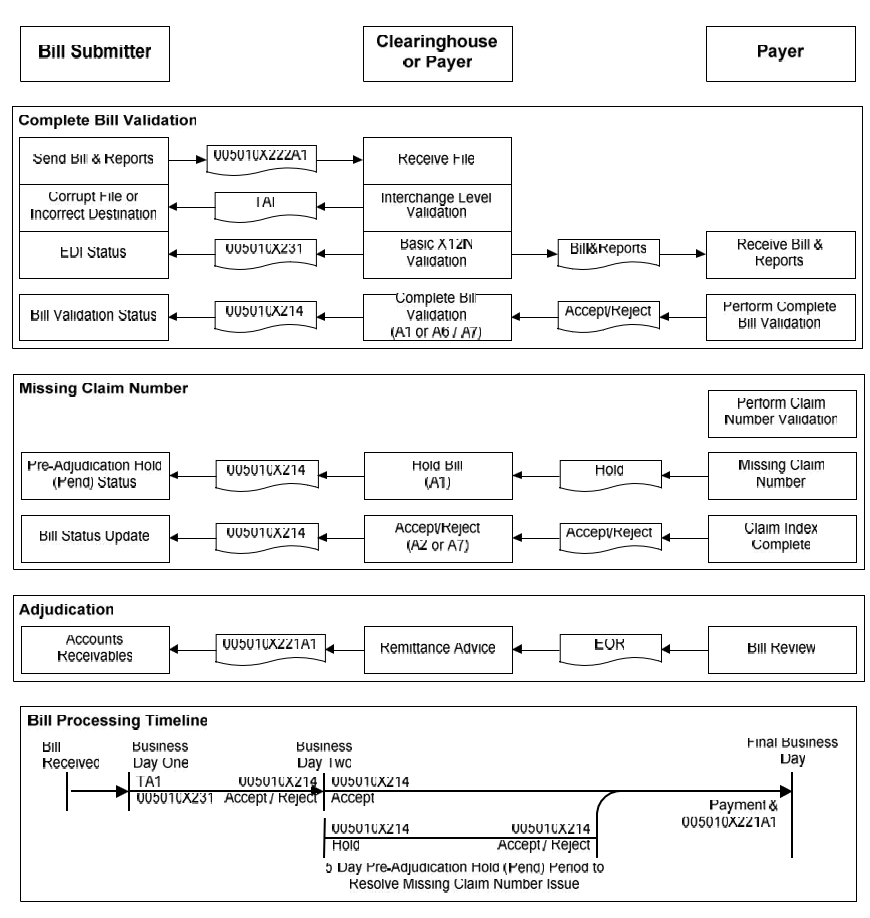
9.1 Bill Acknowledgment Flow and Timing Diagrams
The process chart below illustrates how a receiver validates and processes an incoming 005010X222A1, 005010X223A2, or 005010X224A2 transaction. The diagram shows the basic acknowledgments that the receiver generates, including acknowledgments for validation and final adjudication for those bills that pass validation.
9.1.1 Process Steps
- Interchange Level Validation: Basic file format and the trading partner information from the Interchange Header are validated. If the file is corrupt or is not the expected type, the file is rejected. If the trading partner information is invalid or unknown, the file is rejected. A TA1 (Interchange Acknowledgment) is returned to indicate the outcome of the validation. A rejected EDI file is not passed on to the next step.
- Basic X12 Validation: A determination will be made as to whether the transaction set contains a valid 005010X222A1, 005010X223A2, or 005010X224A2. A 005010X231 (Implementation Acknowledgment) will be returned to the submitter. The 005010X231 contains ACCEPT or REJECT information. If the file contains syntactical errors, the locations of the errors are reported. Bills that are part of a rejected transaction set are not passed on to the next step.
- Complete Bill Validation: The jurisdictional and payer specific edits are run against each bill within the transaction set. The receiver returns a 005010X214 (Health Care Claim Acknowledgment) to the submitter to acknowledge that the bill was accepted or rejected. Bills that are rejected are not passed on to the next step.
- Complete Bill – Missing Claim Number and/or Missing Required Report: Refer to Section 9.2 Complete Claim - Missing Claim Number Pre-Adjudication Hold (Pending) Status and Section 9.3 Complete Claim - Missing Report Pre-Adjudication Hold (Pending) Status regarding bill acknowledgment flow and timeline diagrams.
- Bill Review: The bills that pass through bill review and any post-bill review approval process will be reported in the 005010X221A1 (Remittance Payment/Advice). The 005010X221A1 contains the adjudication information from each bill, as well as any paper check or EFT payment information.
9.2 Complete Bill - Missing Claim Number Pre-Adjudication Hold (Pending) Status
One of the processing steps that a bill goes through prior to adjudication is verification that the bill concerns an actual employment-related condition that has been reported to the employer and subsequently reported to the claims administrator. This process, usually called “claim indexing/validation,” can cause a delay in the processing of the bill. Once the validation process is complete, the claim administrator assigns a claim number to the injured worker’s claim. This claim number is necessary for the proper processing of any bills associated with the claim. Until the claim number is provided to the bill submitter, it cannot be included on the 005010X222A1, 005010X223A2, and 005010X224A2 submission to the payer. In order to prevent medical bills from being rejected due to lack of a claim number, a pre-adjudication hold (pending) period of up to five business days is mandated to enable the payer to attempt to match the bill to an existing claim in its system. If the bill cannot be matched within the five days, the bill may be rejected as incomplete. If the payer is able to match the bill to an existing claim, it must attach the claim number to the transaction and continue the adjudication process. The payer then provides the claim number to the bill submitter using the 005010X214 for use in future billing. The 005010X214 is also used to inform the bill submitter of the delay and the ultimate resolution of the issue.
Due to the pre-adjudication hold (pend) status, a payer may send one STC (Status Information) segment with up to three claim status composites (STC01, STC10, and STC11) in the 005010X214. When an otherwise complete bill has a missing claim number and a missing report, the one STC segment in the 005010X214 would have the following three claim status composites: STC01, STC10, and STC11.
An example: STC*A1:21*20090830*WQ*70******A1:629*A1:294~
When an otherwise complete bill is only missing a claim number or missing a report, the one STC segment in the 005010X214 would have the following two claim status composites: STC01 and STC10.
An example: STC*A1:21*20090830*WQ*70******A1:629~
A bill submitter could potentially receive two 005010X214 transactions as a result of the pre-adjudication hold (pend) status.
9.2.1 Missing Claim Number 005010X214 Acknowledgment Process Steps
When the 005010X222A1, 005010X223A2, or 005010X224A2 transaction has passed the complete bill validation process and Loop 2010 CA REF02 indicates that the workers’ compensation claim number is “unknown,” the payer will need to respond with the appropriate 005010X214.
| Claim Number Validation Status | 005010X214 |
|---|---|
| Complete Bill - Missing Claim Number | If the payer needs to pend an otherwise complete bill due to a missing claim number, it must use the following Claim Status Category Code and Claim Status Code: STC01-1 = A1 (The claim/encounter has been received. This does not mean that the claim has been accepted for adjudication.) STC01-2 = 21 (Missing or Invalid Information) AND STC10-1 = A1 (The claim/encounter has been received. This does not mean that the claim has been accepted for adjudication.) STC10-2 = 629 (Property Casualty Claim Number) Example: STC*A1:21*20090830*WQ*70******A1:629~ |
| Claim Index/Validation Complete | 005010X214 |
|---|---|
| Complete Bill Was Found | Once the Claim Indexing/Validation process has been completed and there is a bill/claim number match, then the payer should use the following Claim Status Category Code with the appropriate Claim Status Code: STC01-1 = A2 (Acknowledgment/Acceptance into adjudication system. The claim/encounter has been accepted into the adjudication system.) STC01-2 = 20 (Accepted for processing) Payer Claim Control Number: Use Loop 2200D REF Payer Claim Control Number segment with qualifier 1K Identification Number to return the workers’ compensation claim number and/or the payer bill control number in the REF02: Always preface the workers’ compensation claim number with the two digit qualifier ‘Y4’ followed by the property casualty claim number. Example: Y412345678 If there are two numbers (payer claim control number and property casualty claim number) returned in the REF02, a blank space should be used to separate the numbers. The first number will be the payer claim control number assigned by the payer (bill control number). The second number will be the workers’ compensation property casualty claim number assigned by the payer with a ’Y4’ qualifier followed by the property casualty claim number. Example: REF*1K*3456832 Y43333445556~ |
| Claim Index/Validation Complete | 005010X214 |
|---|---|
| No Bill Found | After the Claim Indexing/Validation process has been completed and there is no match between the bill and the claim number, payers should use the following Claim Status Category Code with the appropriate Claim Status Code: STC01-1 = A6 (Acknowledgment/Rejected for Missing Information - the claim/encounter is missing the information specified in the Status details and has been rejected.) |
9.3 Complete Bill - Missing Report Pre-Adjudication Hold (Pending) Status
One of the processing steps that a bill goes through prior to adjudication is verification that all required documentation has been provided. The bill submitter can send the reports using the 005010X210 or other mechanisms such as fax or e-mail. In order to prevent medical bill rejections because required documentation was sent separately from the bill itself, a pre-adjudication hold (pending) period of up to five business days is mandated to enable the payer to receive and match the bill to the documentation. If the bill cannot be matched within the five days, or if the supporting documentation is not received, the bill may be rejected as incomplete.
If the payer is able to match the bill to the documentation within the five day hold period, it continues the adjudication process. The 005010X213 is used to inform the bill submitter of the delay and the ultimate resolution of the issue.
9.4 Missing Report - 277 Health Care Claim Acknowledgment Process Steps
When a bill submitter sends an 837 that requires an attachment and Loop 2300 PWK segment indicates that a report will be following, the payer will need to respond with the appropriate 277 HCCA response(s) as applicable:
| Bill Status Findings | 277 Health Care Claim Acknowledgment (HCCA) Options |
|---|---|
| Complete Bill - Missing Report | When a complete bill is missing a required report, the payer needs to place the bill in a pre-adjudication hold (pending) status during the specified waiting time period and return the following Claim Status Category Code and Claim Status Code: STC01-1 = A1 (The claim/encounter has been received. This does not mean that the claim has been accepted for adjudication.) STC01-2 = 21 (Missing or invalid information) AND STC10-1 = A1 (The claim/encounter has been received. This does not mean that the claim has been accepted for adjudication.) STC10-2 = Use the appropriate 277 Claim Status Code for missing report type. Example: Claim Status Code 294 Supporting documentation Example: STC*A1:21*20090830*WQ*70******A1:294~: |
| Report Received within the 5 day pre-adjudication hold (pending) period | Once the Claim Indexing/Validation process has been completed and there is a bill/claim number match, then the payer should use the following Claim Status Category Code with the appropriate Claim Status Code: STC01-1= A2 Acknowledgment/Acceptance into adjudication system. The claim/encounter has been accepted into the adjudication system. STC01-2=20 Accepted for processing Use Loop 2200D REF segment “Payer Claim Control Number with qualifier 1K Identification Number to return the workers’ compensation claim number and or the payer bill control number in the REF02: Always preface the workers’ compensation claim number with the two digit qualifier “Y4” followed by the property casualty claim number. Example: Y412345678 If there are two numbers (payer claim control number and the workers’ compensation claim number) returned in the REF02, the payer should use a blank space to separate the numbers. The first number will be the payer claim control number assigned by the payer (bill control number). The second number will be the workers’ compensation property casualty claim number assigned by the payer with a “Y4” qualifier followed by the claim number. -Example: REF*1K*3456832 Y43333445556~ |
| No Report Received within the 5 day pre-adjudication hold (pending) period | Use the following Claim Status Category Code and Claim Status Code. STC01-1= A6 Acknowledgment/Rejected for Missing Information. The claim/encounter is missing the information specified in the Status details and has been rejected. STC01-2=294 Supporting documentation |
9.5 Transmission Responses/Acknowledgments
9.5.1 Acknowledgments
The X12 transaction sets include a variety of acknowledgments to inform the sender about the outcome of transaction processing. Acknowledgments are designed to provide information regarding whether or not a transmission can be processed, based on structural, functional, and/or application level requirements or edits. In other words, the acknowledgments inform the sender whether or not the medical bill can be processed or if the transaction contains all the required data elements.
Claim administrators must return one of the following acknowledgments, as appropriate, according to the Bill Acknowledgment Flow and Timing Diagrams found in Section 9.1:
- TA1 -- Implementation Acknowledgment
- 005010X231 -- Implementation Acknowledgment (999)
- 005010X214 -- Health Care Claim Acknowledgment (277)
Detailed information regarding the content and use of the various acknowledgments can be found in the applicable X12N Technical Reports Type 3 (Implementation Guides).
9.5.2 005010X213 - Request for Additional Information
The 005010X213, or Request for Additional Information, is used to request missing required reports from the submitter. The following are the STC01 values:
Claim was pended; additional documentation required.
STC01-1 = R4 (pended/request for additional supporting documentation) STC01-2 = The LOINC code indicating the required documentation
9.5.3 Additional information regarding this transaction set may be found in the applicable X12N Technical Report Type 3 (Implementation Guides).
005010X221A1 - Health Care Claim Payment/Advice Within 15 of days of receipt of a complete electronic medical bill, the claims administrator is required to send the health care provider the 005010X221A1, or Health Care Claim Payment/Advice. This transaction set informs the health care provider about the payment action the claims administrator has taken. Additional information regarding this transaction set may be found in Chapter 7 of this companion guide and the applicable X12N Technical Report Type 3 Implementation Guides.
9.5.4 005010X212 Health Care Claim Status Request and Response
The 005010X212 transaction set is used in the group health industry to inquire about the current status of a specified healthcare bill or bills. The 276 transaction set identifier code is used for the inquiry and the 277 transaction set identifier code is used for the reply. It is possible to use these transaction sets unchanged in workers’ compensation bill processing. Additional information regarding this transaction set may be found in the applicable ASC X12N Technical Reports Type 3 Implementation Guides.
Appendix B | Jurisdiction Report Type Codes and Tennessee Descriptions
This Appendix is designed to provide stakeholders with the list of “jurisdictional codes” that will be used to identify documents for which an X12 code is not yet available. Jurisdictions should review the code list contained in the X12 Technical Report Type 3 and evaluate jurisdiction-specific documentation requirements before completing this table. Any code values not used by a jurisdiction must be removed from the table (for example, J3 Medical Permanent Impairment Report is not used in California and would be removed from the California companion guide). The code values listed below represent the first two characters of the attachment control number when a jurisdictional report is being submitted with the 837 transaction.
Appendix C | Tennessee’s Change Log
Changes to Conform to IAIABC Workers' Compensation Electronic Billing and Payment National Companion Guide
| Section | Change |
|---|---|
| Important Notes | Updated the telephone number for IAIABC |
| Permission from IAIABC | Updated the Release version from 2.2 to 2.3 |
| Contact Information | Updated the telephone number and email for the BWC contact |
| All Sections | Converted document from PDF to HTML (March 2026) |
| 7.1 | Fixed broken link to NCPDP Pharmacy Reference Guide to the X12/005010X221 Health Care Claim Payment/Advice (835) |