Vector-Borne Diseases
The Vector-Borne Diseases Program of TDH conducts surveillance on mosquito-borne, tick-borne, and other vector-borne diseases to measure the burden and risk of these diseases in Tennessee. The program also conducts education and outreach activities based on collected data about vector-borne diseases from a number of sources.Vector-Borne Diseases
Vector-borne diseases are illnesses caused by viruses and bacteria that are spread by vectors, such as mosquitoes, ticks, and other arthropods.
Vector-Borne Diseases Program
The Vector-Borne Diseases Program, housed within the Communicable and Environmental Diseases and Emergency Preparedness (CEDEP) section of the Tennessee Department of Health, conducts surveillance on:
- Mosquito-borne diseases
- Tick-borne diseases
- Other vector-borne diseases
This surveillance helps measure the burden and risk of vector-borne diseases in Tennessee. The program tracks and responds to mosquito-borne and tick-borne diseases statewide to protect public health.
Program activities include:
- Conducting surveillance and monitoring disease trends
- Collecting and testing mosquito samples
- Investigating reported human cases
- Collaborating with local agencies on control efforts
- Providing education and outreach to the public and healthcare providers
Trends and Public Health Focus
Mosquito- and tick-borne diseases are increasing in Tennessee and across the United States. The Tennessee Department of Health works to keep the state’s healthcare community informed about the latest vector-borne disease developments to:
- Identify individuals who may be at greater risk
- Improve the timeliness of diagnosis
- Increase the accuracy of diagnoses
Office Contact
For questions or additional information, please contact:
Abelardo Moncayo
Vector-Borne Diseases Program Director
Email: Abelardo.Moncayo@tn.gov
Infestations and Other Arthropods of Concern
Infestations and other arthropods of concern can affect people and animals in different ways. This page provides information about common infestations, such as bed bugs, lice, and fleas, as well as other arthropods that may pose a public health concern in Tennessee.
Infestations
Infestations are caused by pests such as fleas, bed bugs, and lice.
- Bed bugs and head lice do not transmit human diseases. However, they can be disruptive and a nuisance.
- Fleas can be a nuisance to pets and their owners. In some parts of the United States, fleas can act as vectors for plague. This risk does not apply in Tennessee.
Other Arthropods of Concern
Kissing Bugs (Conenose or Vampire Bugs)
Kissing bugs, also known as conenose bugs or vampire bugs, are arthropod vectors found in South America, Central America, and the southern half of North America.
Kissing bugs are important because they can transmit the parasite that causes Chagas disease.
- In Tennessee, an average of two Chagas disease cases per year were reported from 2011 to 2014.
- There have been no confirmed cases of Chagas disease reported in Tennessee since that time.
To learn more, visit the Centers for Disease Control and Prevention (CDC) Chagas disease webpage.
Resources
External link and accessibility notice: Some links on this page take you to websites outside the Tennessee Department of Health (TDH). TDH does not control the content, privacy policies, or accessibility of external sites.
Bed Bugs
Lice
Fleas and Ticks
Spiders
- NIOSH Venomous Spiders Information (includes brown recluse spiders)
Mosquitoes in Tennessee
External link and accessibility notice: Some links on this page take you to websites outside the Tennessee Department of Health (TDH). TDH does not control the content, privacy policies, or accessibility of external sites.
Diseases spread by mosquitoes are a growing concern in Tennessee. Nine mosquito species that can transmit diseases to humans live in the state, and their populations have increased in recent decades.
Mosquitoes need water to lay eggs and develop. Different mosquito species prefer different environments, but reducing standing water helps limit mosquito breeding.
Which Types of Mosquitoes Live in Tennessee?
More than 200 mosquito species live in the United States and its territories. However, only about a dozen species are known to spread pathogens that can cause illness in people.
Below are some of the most common disease-carrying mosquito species found in Tennessee. Selecting the name of a mosquito provides its scientific name, general U.S. distribution, and the diseases it can transmit in Tennessee.
For more information about mosquito species nationwide, visit the CDC Mosquitoes in the United States webpage.
- Asian Bush Mosquito (Aedes japonicus)
Distributed: Eastern and Midwestern United States and the Pacific Northwest
Transmits: La Crosse encephalitis virus - Asian Tiger (Forest) Mosquito (Aedes albopictus)
Distributed: Eastern, Midwestern, and Southern United States
Transmits: La Crosse encephalitis virus, Zika virus, dengue virus, chikungunya virus - Eastern Treehole Mosquito (Aedes triseriatus)
Distributed: Eastern half of the United States
Transmits: La Crosse encephalitis virus - Malaria Mosquito (Anopheles quadrimaculatus)
Distributed: Eastern half of the United States
Transmits: Malaria - Northern House Mosquito (Culex pipiens)
Distributed: Northern half of the United States
Transmits: West Nile virus, St. Louis encephalitis virus, eastern equine encephalitis virus - Southern House Mosquito (Culex quinquefasciatus)
Distributed: Southern half of the United States
Transmits: West Nile virus, St. Louis encephalitis virus, eastern equine encephalitis virus - Western Encephalitis Mosquito (Culex tarsalis)
Distributed: Most of the continental United States, except the Northeast, Mid-Atlantic, and southern Florida
Transmits: West Nile virus, St. Louis encephalitis virus, western equine encephalitis virus - White-Dotted Mosquito (Culex restuans)
Distributed: Most of North America, except parts of the western U.S.
Transmits: West Nile virus, St. Louis encephalitis virus, eastern equine encephalitis virus - Yellow Fever Mosquito (Aedes aegypti)
Distributed: Southern and southwestern United States
Transmits: Zika virus, dengue virus, chikungunya virus, yellow fever virus
Where Are These Mosquitoes Located in Tennessee?
Although mosquito species vary in their environmental preferences, most mosquitoes live near still or slow-moving water, such as:
- Lakes and ponds
- Flooded areas
- Containers that collect rainwater
Mosquito populations may increase significantly in areas prone to flooding, as standing water creates ideal breeding conditions.
Reducing standing water around homes and communities helps limit mosquito populations and reduce disease risk.
Mosquito-Borne Diseases of Concern
The following section highlights mosquito-borne diseases of public health concern in Tennessee, including information about how they are transmitted, potential health effects, and why prevention is important.
West Nile virus (WNV) is the most common mosquito-borne virus in the United States that can infect people. The virus exists in nature primarily through a cycle involving mosquitoes and birds. Mosquitoes become infected with WNV when they feed on infected birds.
Most people infected with WNV have no symptoms. About 20 percent may develop flu-like symptoms, and fewer than 1 percent develop severe illness affecting the brain or nervous system. As with any disease, the public should increase awareness and practice protective measures when exposed to mosquitoes.
To submit dead crows or blue jays for WNV testing, contact your local health department.
For more information, visit the CDC West Nile virus webpage.
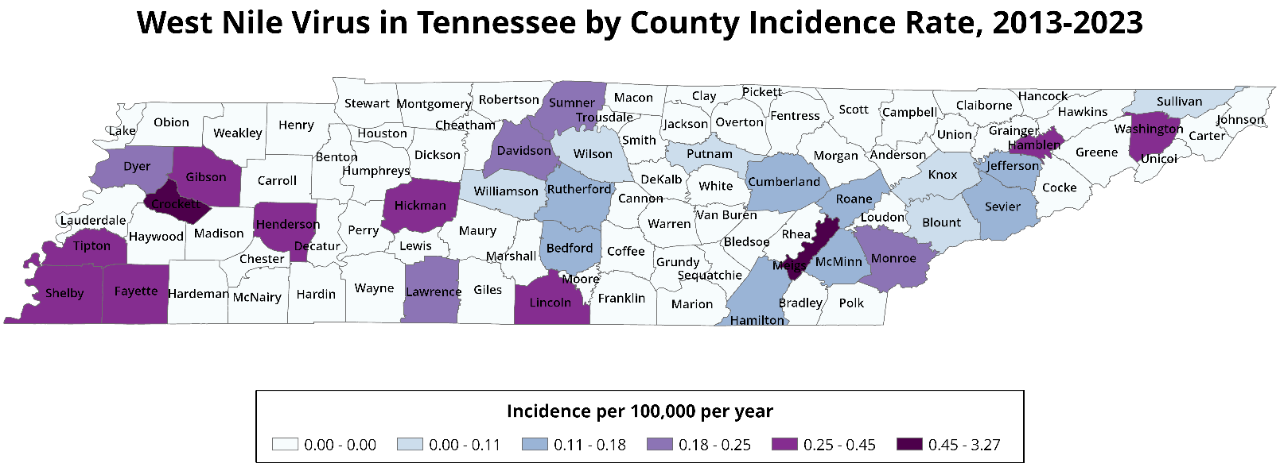
The gradient on this map refers to average WNV incidence rates for each county in Tennesee from 2013-2023, which was calculated using county population data from the 2020 U.S. Census.
In 2023, WNV activity increased as compared to previous years, with a total of 9 human cases. Five of these cases occurred in Shelby County, and single cases also occurred in Davidson, Hamblen, Rutherford, and Williamson Counties.
There were also 1 WNV positive equine case in 2023, which occurred in Gibson County. WNV positive mosquito pools were detected in all 3 counties where mosquito trapping was conducted; Davidson, Shelby, and Knox Counties.
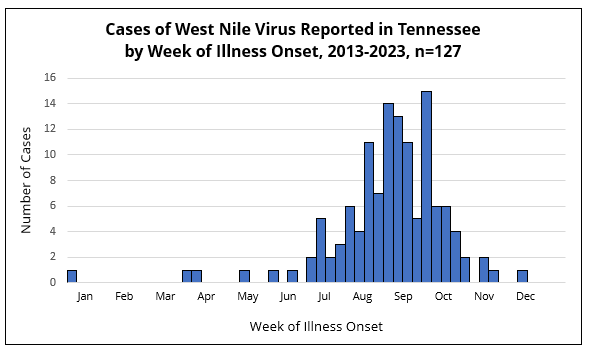
In Tennessee, illness onset for cases of WNV is mainly reported in the second half of the year. The number of reported WNV cases is lowest in the winter (December-March), slightly increases in the late spring to mid-summer (April-July), peaks in the late summer (August-September), and then gradually declines through autumn (October-November).
Signs and symptoms of WNV typically begin 1-2 weeks after being bitten by an infected mosquito. Late spring through mid-summer is the time of year when Tennesseans are most at risk for contracting WNV.
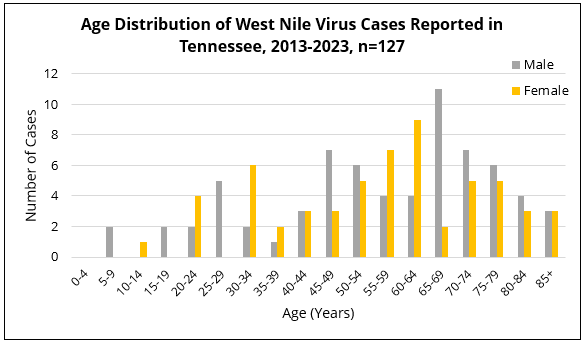
Anyone who spends time outdoors in Tennessee is at risk of contracting WNV. However, persons over 50 years of age are at highest risk of developing the most severe form of the disease, and persons over the age of 70 with pre-existing health problems are at greatest risk for death.
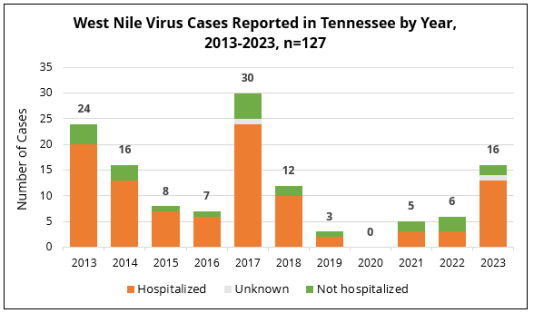
In regards to trends over the past decade, case numbers for WNV have risen in 2023, compared to recent previous years. The dip in cases seen in 2020 can be identified in vector-borne diseases across the board during that year, likely due to a number of factors surrounding the COVID-19 pandemic.
Most people infected with WNV do not devleop any symptoms. About 1 in 5 people who are infected will develop a mild febrile illness, which includes a fever in addition to one or more of the following symptoms:
- Headache
- Body aches
- Joint pains
- Vomiting
- Diarrhea
- Rash
- Fatigue and weakness lasting for weeks or months
About 1 in 150 people who are infected develop a severe illness affecting the central nervous system, such as encephalitis (inflammation of the brain) or meningitis (inflammation of the membranes that surround the brain and spinal cord). Symptoms of severe illness include:
- High fever
- Headache
- Neck stiffness
- Stupor
- Disorientation
- Coma
- Tremors and/or convulsions
- Muscle weakness
- Vision loss
- Numbness and/or paralysis
For more information, see the CDC WNV Symptoms, Diagnosis, & Treatment web page.
WNV is diagnosed by a healthcare provider, who can order blood tests to look for evidence of WNV infection should you begin to experience the signs and symptoms listed above.
For more information, see the CDC WNV Symptoms, Diagnosis, & Treatment webpage.
| Year | Human | Horses | Birds | Mosquito Pools |
|---|---|---|---|---|
| Positive | Positive | Positive | Positive | |
| 2000 | 0 | 0 | 0 | 0 |
| 2001 | 0 | 1 | 46 | 0 |
| 2002 | 56 | 141 | 823 | 307 |
| 2003 | 26 | 103 | 275 | 308 |
| 2004 | 14 | 15 | 34 | 405 |
| 2005 | 18 | 7 | 12 | 574 |
| 2006 | 22 | 8 | 1 | 626 |
| 2007 | 11 | 4 | 7 | 600 |
| 2008 | 19 | 6 | 3 | 658 |
| 2009 | 8 | 5 | 1 | 488 |
| 2010 | 4 | 3 | 0 | 403 |
| 2011 | 18 | 3 | 0 | 995 |
| 2012 | 33 | 6 | 6 | 916 |
| 2013 | 24 | 4 | 1 | 824 |
| 2014 | 16 | 0 | 0 | 728 |
| 2015 | 8 | 1 | 0 | 694 |
| 2016 | 7 | 0 | 0 | 776 |
| 2017 | 32 | 3 | 32 | 1671 |
| 2018 | 13 | 12 | 2 | 1119 |
| 2019 | 4 | 1 | 0 | 488 |
| 2020 | 0 | 0 | 0 | 725 |
| 2021 | 5 | 2 | 0 | 666 |
| 2022 | 6 | 1 | 0 | 288 |
| 2023 | 16 | 2 | 2 | 1238 |
La Crosse virus (LACV) is transmitted by the bite of an infected Aedes mosquito, most commonly the eastern treehole mosquito. Some people may develop severe neuroinvasive disease such as La Crosse encephalitis (LACE), which can include seizures, coma, or paralysis. Severe disease occurs most often in children under 16.
In 2023, there were three probable or confirmed cases of LACE in Tennessee, and the patients were less than 9 years old. Over the past decade, nearly all LACE cases reported in Tennessee had neuroinvasive symptoms.
For more information, visit the CDC La Crosse encephalitis webpage.
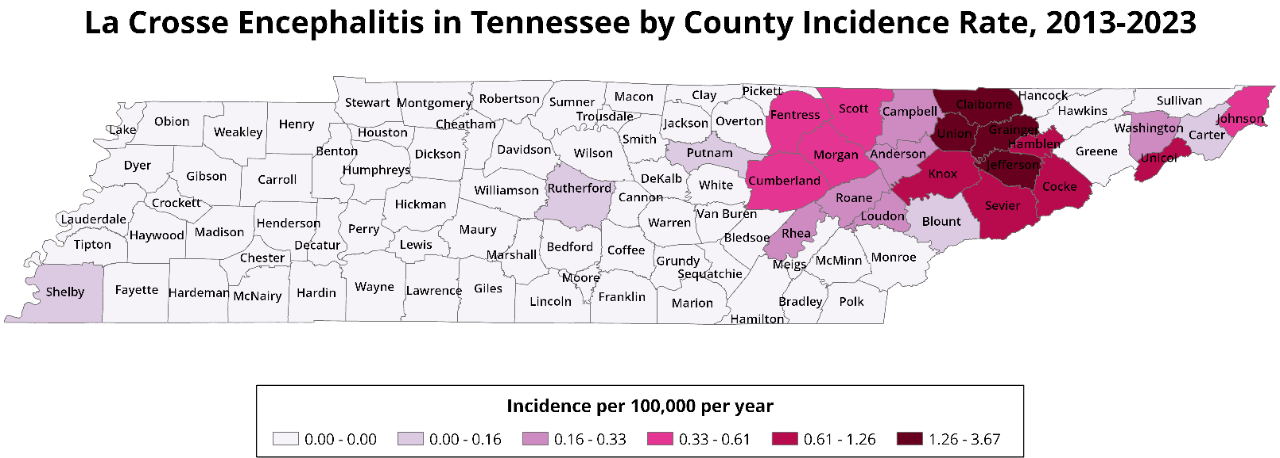
The gradient on the map below refers to average LACE incidence rates for each county in Tennesee from 2013-2023, which was calculated using county population data from the 2020 U.S. Census.
According to data from the past ten years, LACE cases are generally reported in the Eastern portion of the state.
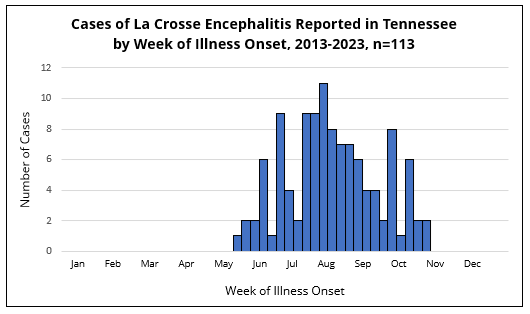
In Tennessee, illness onset for cases of LACE is mainly reported in the warmer months of the year. The number of reported LACE cases is lowest in the winter and spring (December-April), slightly increases in the early- to mid-summer (May-July), peaks in August, and then gradually declines through autumn (September-November).
Signs and symptoms of LACE typically begin 3-10 days after being bitten by an infected mosquito. Late spring through mid summer is the time of year when Tennesseans are most at risk for contracting LACV from a mosquito.
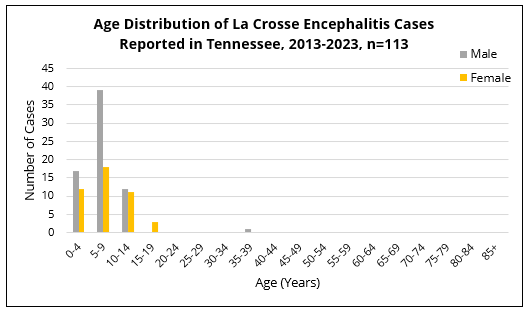
Anyone who spends time outdoors in Tennessee is at risk of contracting LACV from the bite of an infected mosquito. However, the majority of people infected with LACV do not develop LACE. The severe neuroinvasive disease associated with LACE occurs most frequently in chlidren under the age of 16 years.
From 2013-2023, only one Tennesseean above the age of 19 developed LACE.
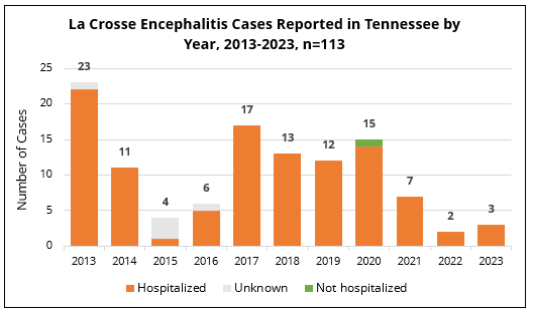
LACE is most often diagnosed for severe cases, because testing for this virus is rarely done on patients presenting with mild febrile illness. As a result, most LACE cases have already developed severe neuroinvasive disease by the time that they are diagnosed, leading to a high hospitalization rate.
Over the last 10 years in Tennessee, 96% of LACE cases were hospitalized for severe illness. Although LACE case numbers decreased in 2015 and 2021-2022, there has been a median of approximately 15 cases per year in our state.
Most people infected with LACV do not have any symptoms. For those who do develop symptoms, the time from infected mosquito bite to feeling sick ranges from 3-10 days. Early signs and symptoms are usually mild or moderate, and they may include:
- Fever (lasting for 2-3 days)
- Headache
- Nausea and/or vomiting
- Tiredness and reduced activity/alertness
Severe neuroinvasive disease classified as LACE occurs most frequently in children under the age of 16 years. Although seizures and other nervous system conditions are common, most patients recover completely. However, some effects on the central nervous system from severe LACE can persist overtime. Long-term effects can include:
- Recurrent seizures
- Partial paralysis of one side of the body
- Cognitive or behavioral impairments
For more information, see the CDC's LACE Symptoms, Diagnosis, & Treatment webpage.
LACE is diagnosed by a healthcare provider, who can order blood tests to look for evidence of LACV infection if you experience the symptoms described above. For more information, see the CDC's LACE Symptoms, Diagnosis, & Treatment web page.
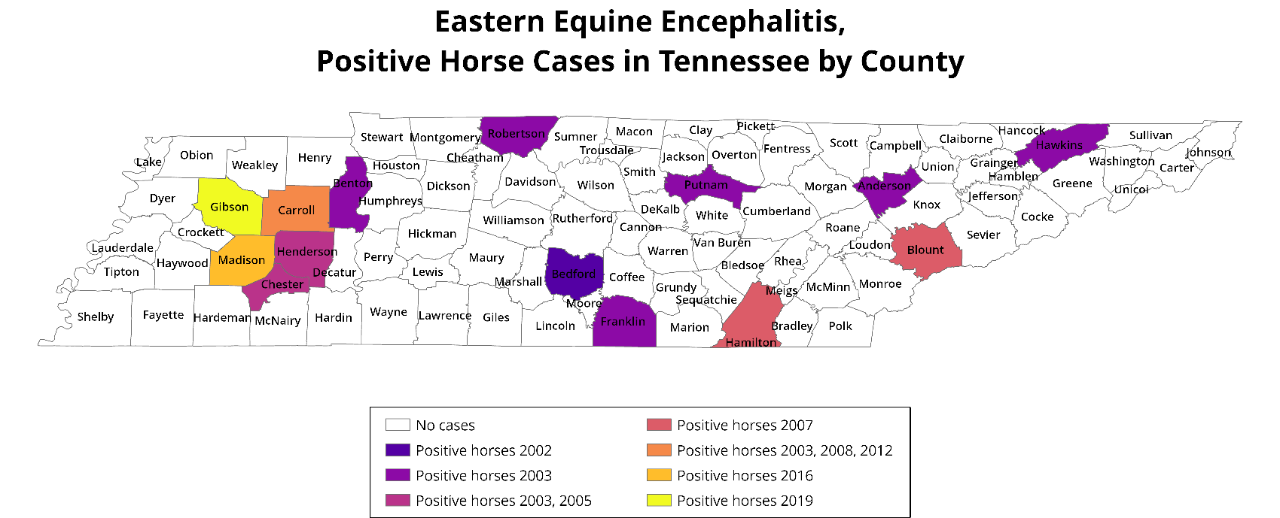
Eastern equine encephalitis (EEE) virus is spread to humans and horses by the bite of an infected Aedes or Culex mosquito. These mosquitoes typically inhabit swamps and surrounding areas in rural portions of the country. Although only a few cases are reported in the United States each year, EEE is very serious. About 30 percent of people with EEE die, and many survivors have ongoing neurologic issues.
In 2019, Tennessee’s first human case of EEE was reported in Hamilton County. There are no vaccines to prevent or medicines to treat EEE. Preventing mosquito bites is the best way to reduce risk.
For more information, visit the CDC Eastern equine encephalitis webpage.
CDC Light Trap

Mosquito Resting Box

Trinidad Trap

For those EEE-infected persons who experience symptoms, the time from infected mosquito bite to feeling sick ranges from 4-10 days. The type of illness that develops depends on the age of the person and other factors, but in general, EEE infection can result in febrile illness or neurologic disease. Febrile illness lasts for 1-2 weeks, and most people recover completely. Signs and symptoms of febrile illness can include:
- Fever
- Chills
- Body aches
- Joint pain
Neurologic disease resulting from EEE infection can include meningitis (infection of the membranes that surround the brain and spinal cord) or encephalitis (infection of the brain). People who recover from this severe illness are often left with long-term physical or mental impairments, which can range from mild brain dysfunction to severe intellectual or social impairment. In addition to fever and headache, signs and symptoms of neurologic disease can include:
- Diarrhea
- Seizures
- Behavioral changes
- Drowsiness
- Coma
For more information, see the CDC's EEE Symptoms, Diagnosis, & Treatment webpage.
EEE is diagnosed by a healthcare provider, who can order blood tests to look for evidence of EEE virus infection if you experience the symptoms described above. For more information, see the CDC's EEE Symptoms, Diagnosis, & Treatment webpage.
Travel-Associated Mosquito-Borne Diseases
Some mosquito-borne diseases reported in Tennessee are typically associated with international travel, including:
If you think you may have a mosquito-borne disease, contact a healthcare provider immediately.
Tick-Borne Diseases
Diseases spread by ticks are a growing concern in Tennessee. Six medically important tick species live in the state, and their populations have increased in recent decades. Ticks typically dwell in grassy, brushy, or wooded areas, and people may be bitten while camping, gardening, hunting, or spending time outdoors. Many people encounter ticks in their own yard or neighborhood.
Most tick bites occur during warmer seasons, but the black-legged tick may pose a threat year-round when temperatures are above freezing.
Which Types of Ticks Live in Tennessee?
Six key tick species live in Tennessee. Selecting the name of a tick should provide its scientific name, where it is commonly found, which diseases it can transmit in Tennessee, and other notes.
- American Dog Tick (Wood Tick) (Dermacentor variabilis)
Distributed: East of the Rocky Mountains and parts of the Pacific Coast
Transmits: Tularemia and Rocky Mountain spotted fever
Notes: Highest risk in spring and summer - Asian Longhorned Tick (Haemaphysalis longicornis)
Distributed: Eastern U.S.; recently found in eastern Tennessee
Transmits: No known human diseases in the U.S.
Notes: Invasive species that can reproduce quickly and cause infestations - Black-Legged Tick (Deer Tick) (Ixodes scapularis)
Distributed: Eastern U.S.
Transmits: Lyme disease, anaplasmosis, babesiosis, Powassan virus
Notes: May bite any time temperatures are above freezing - Brown Dog Tick (Rhipicephalus sanguineus)
Distributed: Worldwide
Transmits: Rocky Mountain spotted fever
Notes: Primarily bites dogs but can bite humans - Gulf Coast Tick (Amblyomma maculatum)
Distributed: Southeastern and mid-Atlantic states
Transmits: Rocky Mountain spotted fever
Notes: Mostly feeds on birds and wildlife - Lone Star Tick (Amblyomma americanum)
Distributed: Eastern U.S.; more common in the southeast
Transmits: Ehrlichiosis, tularemia, Heartland virus, STARI, Alpha-gal syndrome
Notes: Aggressive; adult females have a white dot
Where Are These Ticks Located in Tennessee?
These tick species are commonly found in wooded, brushy areas and can also be found in grassy fields or yards. Always take precautions when spending time outdoors in Tennessee.
The following map provides a general idea of where Ixodes ticks have and can be found throughout the state.
Map of Reported and Established Ixodes Ticks, 2018-2019
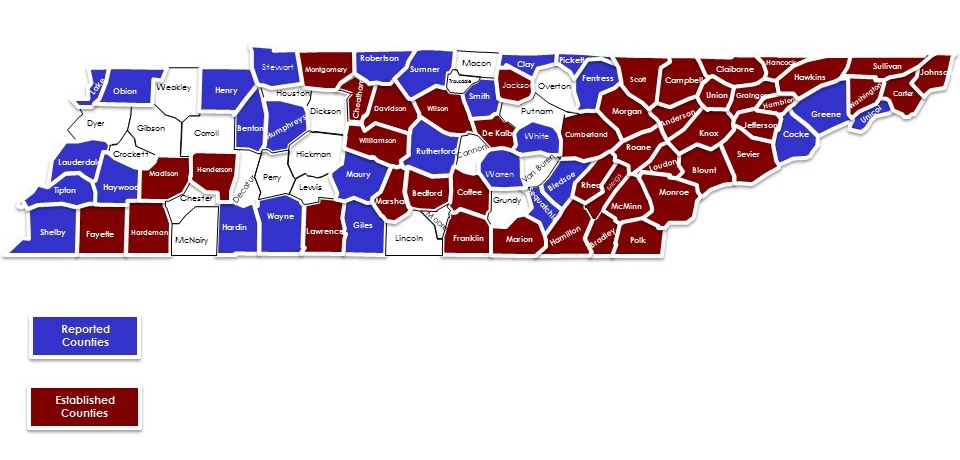
This map shows all counties in the state of Tennessee and categorizes them by the status of Ixodes (blacklegged) tick presence as of 2019. Counties are grouped into three categories indicated by labels in the map legend.
Counties where Ixodes ticks have been reported but are not yet considered established are shown in blue. Counties where Ixodes ticks are established are shown in dark red. Counties with no reported data or no confirmed presence are shown in white.
Established Ixodes tick populations are concentrated primarily in Middle and East Tennessee, including many counties surrounding the Nashville metropolitan area and extending eastward toward the Appalachian region. Reported (but not established) counties are scattered across West Tennessee and parts of Middle Tennessee. Several counties across the state remain unreported or without confirmed Ixodes tick presence.
This map is intended to provide a general geographic overview of Ixodes tick distribution in Tennessee and should not be interpreted as indicating risk at the neighborhood or individual property level.
Tick-Borne Diseases of Concern
The following section highlights tick-borne diseases of public health concern in Tennessee, including information about how they are transmitted, potential health effects, and why prevention is important.
Spotted Fever Rickettsioses are a group of tick-borne diseases caused by Rickettsia bacteria, including Rickettsia rickettsii and Rickettsia parkeri. Rocky Mountain spotted fever (RMSF), caused by Rickettsia rickettsii, is the most severe. In Tennessee, these bacteria are transmitted by the American dog tick and other tick species.
SFR is frequently reported in Tennessee. In 2023, 75 probable and confirmed cases were reported (a decrease from 2022). Prior to 2019, Tennessee often reported over 600 cases annually; COVID-19 and a case definition change in 2020 likely reduced reported case counts. Tennessee is one of five states that account for over 50% of national SFR cases.
For more information, visit the CDC Rocky Mountain spotted fever webpage.
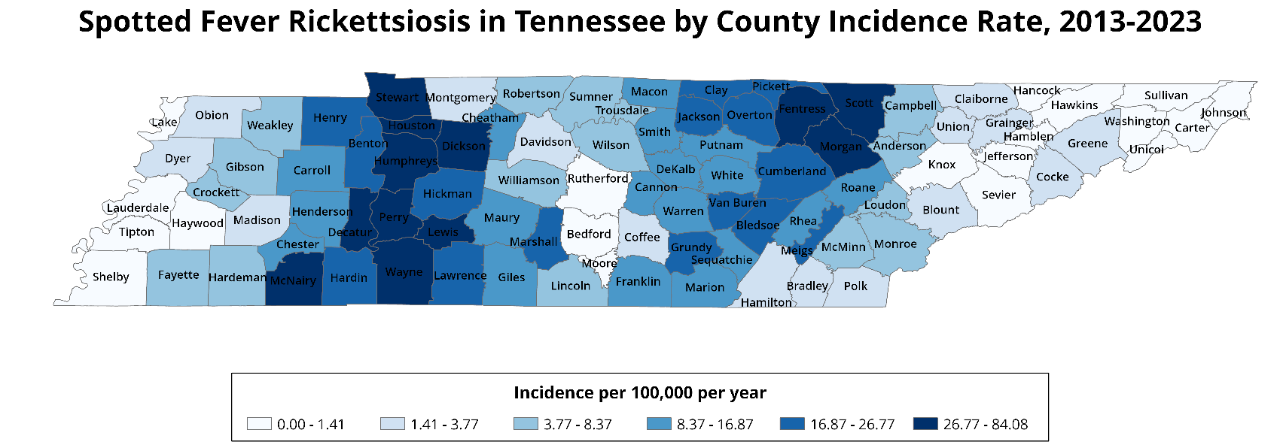
The gradient on the map below refers to average SFR incidence rates for each county in Tennesee from 2013-2023, which was calculated using county population data from the 2020 U.S. Census.
From 2013-2023, there were 4,352 probable and confirmed cases of SFR reported. The top ten counties with the highest reported SFR cases in 2022 and 2023 were in the Mid-Cumberland, South Central, Southeast, Upper Cumberland, and Western regions. Sumner, Lawrence, Stewart, and Wayne counties had an increase in cases in 2023, while case numbers in Davidson, Dickson, and Maury counties dropped by 50% or more. Overall, there was a noticeable decrease in SFR cases in 2023 as compared to 2022.
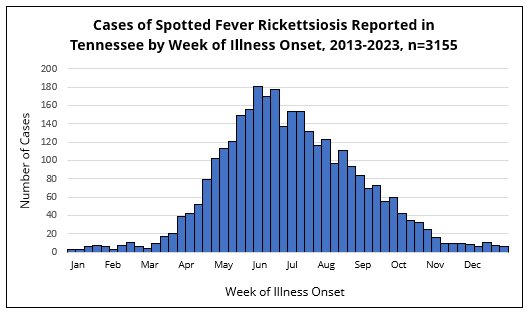
In Tennessee, illness onset for cases of SFR is mainly reported in the warmer months of the year. The number of reported SFR cases is lowest in the winter (December-February), slightly increases in the early spring (March-April), peaks in the late spring to late summer (May-September), and then gradually declines through autumn (October-November).
Peak transmission for SFR in Tennessee is associated with tick season, which occurs annually from early spring to late summer.
Anyone who spends time outdoors in Tennessee is at risk of contracting SFR, because the ticks that spread this disease are most often found in wooded, brushy areas. People holding outdoors-based occupations, such as farmers and landscapers, may be at increased risk of getting bitten by an infected tick, as are people who regularly hike, camp, hunt, or garden in or around wooded areas.
Ticks may also dwell in the property surrounding Tennessee homes, especially if your yard is either next to a brushy area or has tall grass and/or leaf litter. Even outside of our state's forests, it is important to take the necessary steps to prevent tick bites in any environment habitable by these ticks.
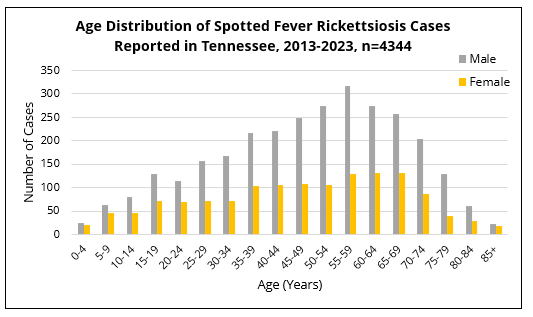
Individuals of any reported gender, sex, and age group in Tennessee can get sick with SFR. However, most cases of SFR are reported in residents 50 years of age or older. Additionally, within every age group, significantly more SFR cases affect male patients than female patients.
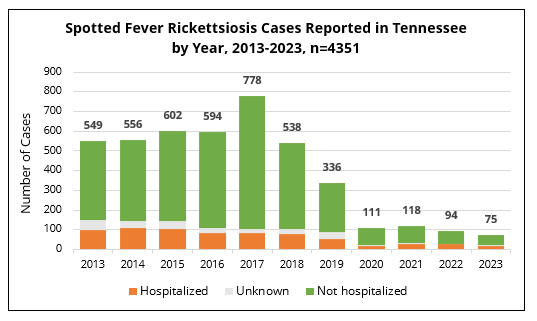
The number of SFR cases reported in Tennessee used to be over 600 annually; however, COVID-19 and a case definition change in 2020 likely reduced this number in 2020-2023. Despite this recent decline, SFR is still a highly reported tick-borne disease in Tennessee.
Early signs and symptoms of SFR typically mirror those of other tick-borne diseases, such as fever and headache. However, if left untreated, this disease can rapidly progress to a serious and life-threatening illness. Common signs and symptoms include:
- Fever
- Headache
- Rash (red splotches or pinpoint dots)
- Nausea
- Vomiting
- Stomach pain
- Muscle pain
- Lack of appetite
Some patients who recover from severe SFR may be left with permanent damage as a result of the acute illness. Long-term health problems can include:
- Amputation of arms, legs, fingers, or toes from damage to blood vessels in these areas
- Hearing loss
- Paralysis
- Mental disability
For more information, see the CDC Rocky Mountain Spotted Fever webpage.
SFR is diagnosed by a healthcare provider, who can order blood tests to look for evidence of Rickettsia species bacteria. It may take several weeks for test results to return. If your provider is concerned, they should prescribe you with antibiotics while you wait for the results.
For more information, see the CDC Rocky Mountain Spotted Fever webpage.
Ehrlichiosis is caused by Ehrlichia chaffeensis (most common) and Ehrlichia ewingii (less common). In Tennessee, it is transmitted by the lone star tick.
Ehrlichiosis was the most reported tick-borne disease in Tennessee in 2023, and reports have increased since 2015. Based on 2023 surveillance data, about 56% of probable and confirmed cases were hospitalized.
For more information, visit the CDC Ehrlichiosis webpage.
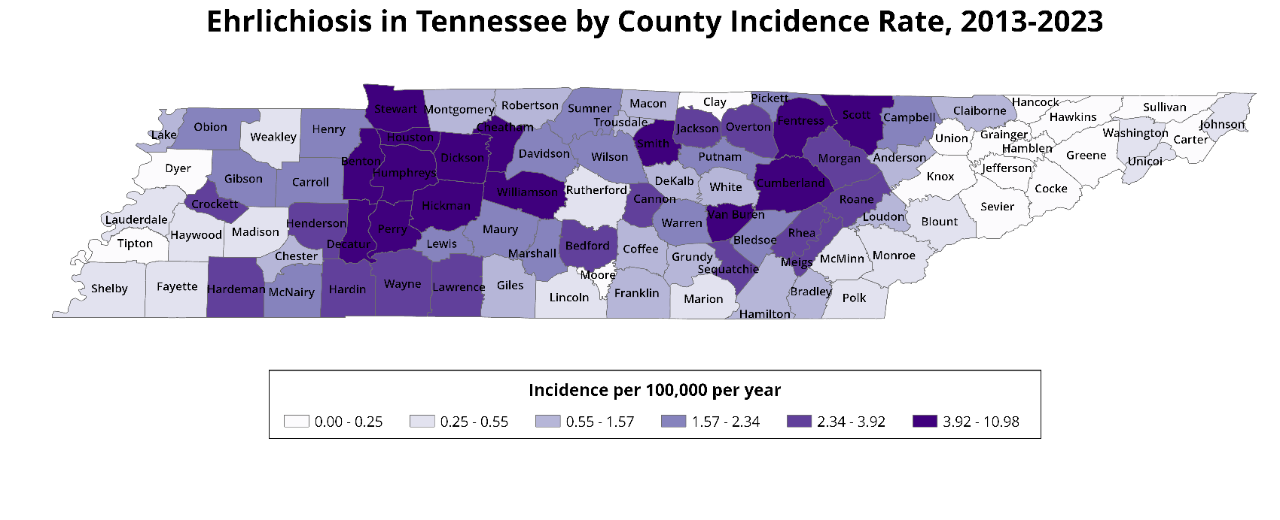
The gradient on the map below refers to average ehrlichiosis incidence rates for each county in Tennesee from 2013-2023, which was calculated using county population data from the 2020 U.S. Census.
Davidson and Williamson counties accounted for 27% of all ehrlichiosis cases reported in the state in 2023.
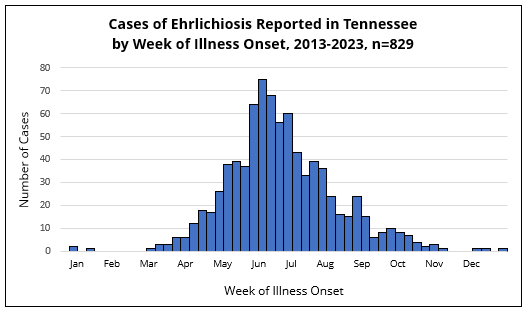
In Tennessee, illness onset for cases of ehrlichiosis is mainly reported in the warmer months of the year. The number of reported ehrlichiosis cases is lowest in the late autumn through winter (November-February), slightly increases in the early spring (March-April), peaks in the late spring to mid summer (May-July), and then gradually declines late summer through early autumn (August-October).
Signs and symptoms of ehrlichiosis typically begin 5-14 days after being bitten by an infected lone star tick. Therefore, late spring through early summer (April-June) is the time of year when Tennesseans are most at risk for contracting ehrlichiosis.
Anyone who spends time outdoors in Tennessee is at risk of contracting ehrlichiosis, because the lone star ticks that spread this disease are most often found in wooded, brushy areas. People holding outdoors-based occupations, such as farmers and landscapers, may be at increased risk of getting bitten by an infected tick, as are people who regularly hike, camp, hunt, or garden in or around wooded areas.
Lone star ticks may also dwell in the property surrounding Tennessee homes, especially if your yard is either next to a brushy area or has tall grass and/or leaf litter. Even outside of our state's forests, it is important to take the necessary steps to prevent tick bites in any environment habitable by these ticks.
Individuals of any reported gender, sex, and age group in Tennessee can get sick with ehrlichiosis. However, most cases of ehrlichiosis are reported in older residents over 50. Additionally, within almost every age group, ehrlichiosis was reported more in males than females.
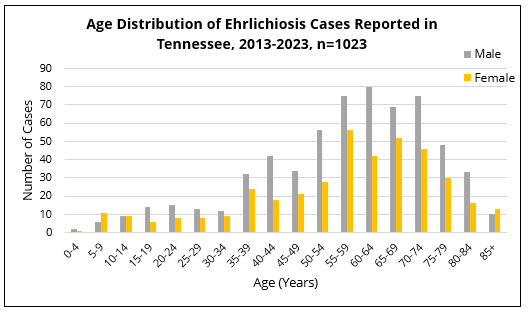
The number of ehrlichiosis cases reported in 2023 increased 22% from the previous year. Although 2020 saw a significant decrease in case counts, likely due to less human-tick exposure during the start of the COVID-19 pandemic, reports of ehrlichiosis in Tennessee have generally been rising since 2015.
Unlike other reportable tick-borne diseases in the state, ehrlichiosis results in hospitalization for 35-65% of Tennesseeans who become infected. In 2023, approximately 56% of all probable and confirmed ehrlichiosis cases were hospitalized for their illness.
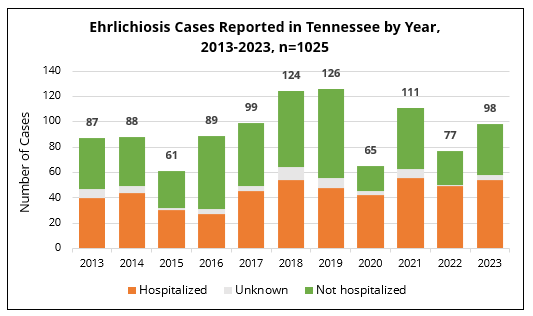
Signs and symptoms of ehrlichiosis typically develop within 1-2 weeks after being bitten by an infected tick. Early signs and symptoms (days 1-5) are usually mild or moderate, and they may include:
- Fever and/or chills
- Severe headache
- Muscle aches
- Nausea, vomiting, diarrhea, or loss of appetite
- Confusion
- Rash that looks like red splotches or pinpoint dots (more common in children than adults)
If antibiotic treatment is delayed, ehrlichiosis can sometimes cause severe illness. Early treatment can reduce your risk of developing severe illness. Late stage signs and symptoms can include:
- Damage to the brain or nervous system (e.g. inflammation of the brain and surrounding tissue)
- Respiratory failure
- Uncontrolled bleeding
- Organ failure
- Death
For more information, see the CDC Signs and Symptoms of Ehrlichiosis webpage.
Ehrlichiosis is diagnosed by a healthcare provider, who can order blood tests to look for evidence of Ehrlichia chaffeensis or Ehrlichia ewingii infection. It may take several weeks for test results to return. If your provider is concerned, they may prescribe you with antibiotics while you wait for the results.
For more information, see the CDC Ehrlichiosis Diagnosis and Testing webpage.
Lyme disease is caused by Borrelia burgdorferi. In Tennessee, it is transmitted by the black-legged tick (deer tick).
Lyme disease is the third highest reported tick-borne disease in Tennessee. There were 39 cases in 2023, an 18% increase from 32 cases in 2022. Although Lyme disease is often associated with the Northeast and Midwest, expansion of black-legged ticks in the Southeast has increased concern in northern and eastern Tennessee.
For more information, visit the CDC Lyme disease webpage.
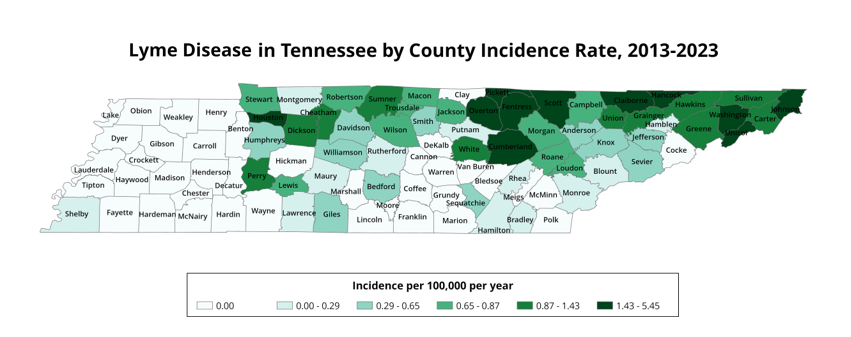
The gradient on the map below refers to average Lyme disease incidence rates for each county in Tennesee from 2013-2023, which was calculated using county population data from the 2020 U.S. Census.
From 2013-2023, there were 382 Lyme disease cases reported; 94% of those cases were in residents from the Middle and Eastern grand divisions of the state. In the last decade, 9 of the top 15 counties with the highest incidence rate of Lyme are in the northeast region that borders Virginia and North Carolina. The other counties with the highest incidence rates tend to fall along the northern part of the state that borders Kentucky. This may indicate a need for enhanced surveillance and messaging to healthcare providers in these regions.
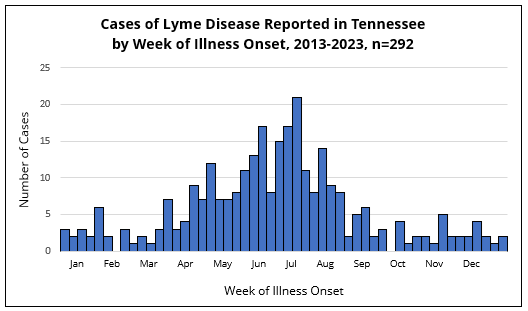
In Tennessee, illness onset for cases of Lyme disease is mainly reported in the warmer months of the year. The number of reported Lyme disease cases is lowest in the winter (December-February), slightly increases in the spring (March-May), peaks in the early to late summer (June-August), and then gradually declines through autumn (October-November).
Signs and symptoms of Lyme disease typically begin 3-30 days after being bitten by an infected black-legged tick. Therefore, late spring through mid summer is the time of year when Tennesseans are most at risk for contracting Lyme disease.
Anyone who spends time outdoors in Tennessee is at risk of contracting Lyme disease, because the black-legged tick that spreads this disease are most often found in wooded, brushy areas. People holding outdoors-based occupations, such as farmers and landscapers, may be at increased risk of getting bitten by an infected tick, as are people who regularly hike, camp, hunt, or garden in or around wooded areas.
Black-legged ticks may also dwell in the property surrounding Tennessee homes, especially if your yard is either next to a brushy area or has tall grass and/or leaf litter. Even outside of our state's forests, it is important to take the necessary steps to prevent tick bites in any environment habitable by these ticks.
Individuals of any reported gender, sex, and age group in Tennessee can get sick with Lyme disease. However, a relatively larger number of cases of Lyme disease are reported in female-identifying patients ages 30-55.
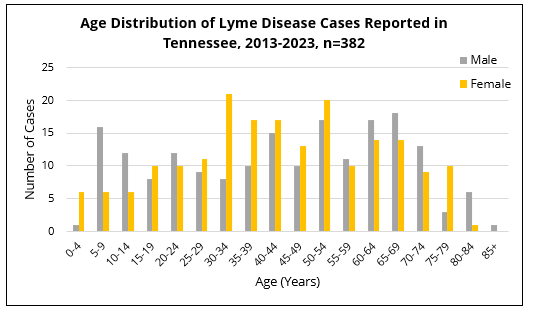
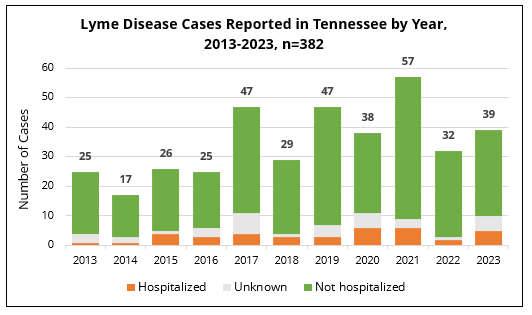
The number of Lyme disease cases reported per year in Tennessee has been steadily increasing since 2014. In 2023, a 39 confirmed and probable cases were reported. The overall rise in the past 8 years can be attributed to the expansion of Ixodes ticks from the northeastern to the southeastern U.S. region.
Hospitalization rates for Lyme disease patients in Tennessee have been consistently low.
Signs and symptoms of Lyme disease typically develop between 3-30 days after being bitten by an infected tick. Early signs and symptoms may include:
- Fever, chills, headache, fatigue, muscle and joint aches, and swollen lymph nodes
- Erythema migrans (EM) rash:
- Occurs in approximately 70-80% of infected persons
- Begins at the site of a tick bite after a delay of 3-30 days (average is about 7 days)
- Expands gradually over several days, reaching up to 12 inches or more across
- May feel warm to the touch, but is rarely itchy or painful
- Sometimes clears as it enlarges, resulting in a target or "bull's-eye" appearance
- May appear on any area of the body
- Does not always appear as a "classic" EM rash
If antibiotic treatment is delayed, Lyme disease can produce a wide array of symptoms, depending on the stage of infection. Late stage signs and symptoms occur days to months after a tick bite and can include:
- Severe headaches and neck stiffness
- Additional EM rashes on other areas of the body
- Facial palsy (loss of muscle tone or droop on one or both sides of the face)
- Arthritis with severe joint pain and swelling, particularly in the knees and other large joints
- Intermittent pain in tendons, muscles, joints, and bones
- Heart palpitations or an irregular heart beat
- Episodes of dizziness or shortness or breath
- Inflammation of the brain and spinal cord
- Nerve pain
- Shooting pains, numbness, or tingling in the hands or feet
For more information, see the CDC Signs and Symptoms of Untreated Lyme Disease webpage.
Lyme disease is diagnosed by a healthcare provider, who will use a combination of clinical observations and laboratory testing to assess whether Borrelia burgdorferi is present. Providers will consider the signs and symptoms of Lyme disease, the likelihood that the patient has been exposed to infected black-legged ticks, the possibility that other illnesses may cause similar symptoms, and the results of laboratory testing to decide whether a diagnosis should be made.
The laboratory criteria recommended by the CDC involves two tests, both of which can be done using the same blood sample. It may take several weeks for test results to return. If your provider is concerned, they may prescribe you with antibiotics while you wait for the results.
For more information, see the CDC Clinical Testing and Diagnosis for Lyme Disease webpage.
Anaplasmosis is caused by Anaplasma phagocytophilum. In Tennessee, it is transmitted by the black-legged tick.
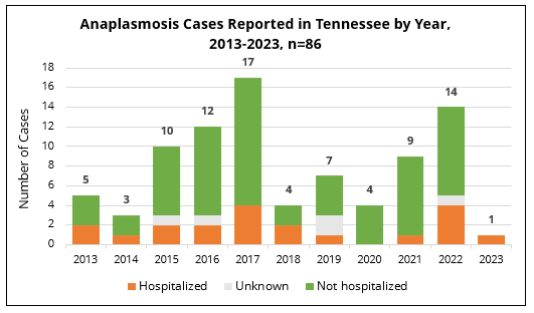
Cases have increased since 2014. In 2023, there was a decrease to one case, compared to 14 cases in 2022. The expanding distribution of black-legged ticks makes this an emerging concern.
For more information, visit the CDC Anaplasmosis webpage.
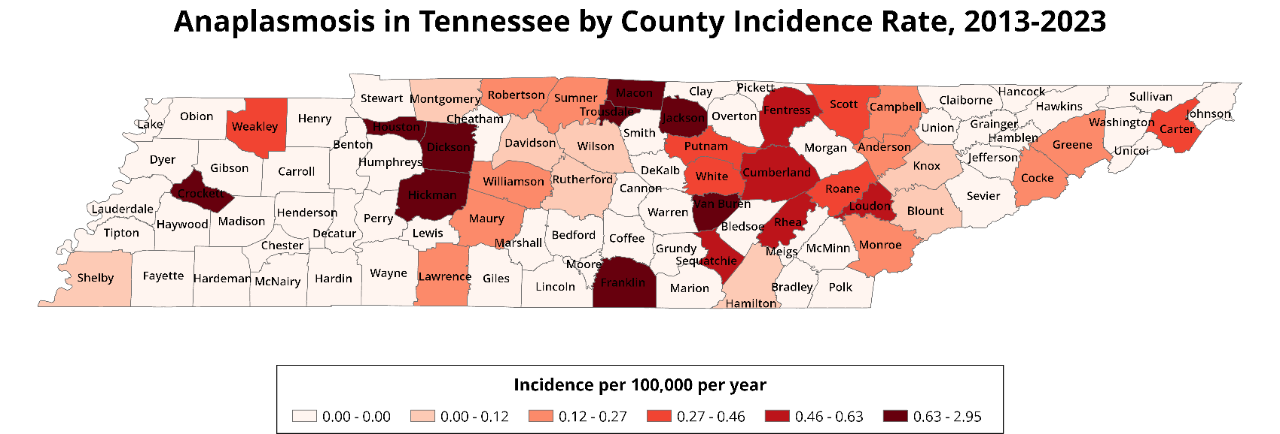
The gradient on the map below refers to average anaplasmosis incidence rates for each county in Tennesee from 2013-2023, which was calculated using county population data from the 2020 U.S. Census.
From 2013-2023, there was an average of 2 cases per county reporting positive Anaplasma infections. Dickson County reported 12 anaplasmosis cases (or 12% of all reported cases) during that time.
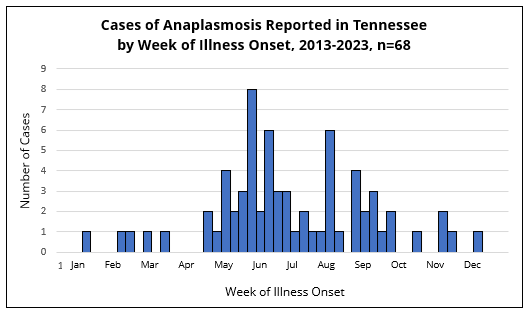
In Tennessee, illness onset for cases of anaplasmosis is mainly reported in the warmer months of the year. The number of reported anaplasmosis cases is lowest in the winter (December-February), slightly increases in the spring (March-May), peaks in the mid to late summer (June-September), and then gradually declines through autumn (October-November).
67% of anaplasmosis cases occur in the mid to late summer months between June and September.
Signs and symptoms of anaplasmosis typically begin 5-14 days after being bitten by an infected black-legged tick. Therefore, late spring through mid summer is the time of year when Tennesseans are most at risk for contracting anaplasmosis.
Anyone who spends time outdoors in Tennessee is at risk of contracting anaplasmosis, because the black-legged tick that spreads this disease is most often found in wooded, brushy areas. People holding outdoors-based occupations, such as farmers and landscapers, may be at increased risk of getting bitten by an infected tick, as are people who regularly hike, camp, hunt, or garden in or around wooded areas.
Black-legged ticks may also dwell in the property surrounding Tennessee homes, especially if your yard is either next to a brushy area or has tall grass and/or leaf litter. Even outside of our state's forests, it is important to take the necessary steps to prevent tick bites in any environment habitable by black-legged ticks.
Individuals of any reported gender, sex, and age group in Tennessee can get sick with anaplasmosis. However, most cases of anaplasmosis are reported in residents between the ages of 35 and 70.
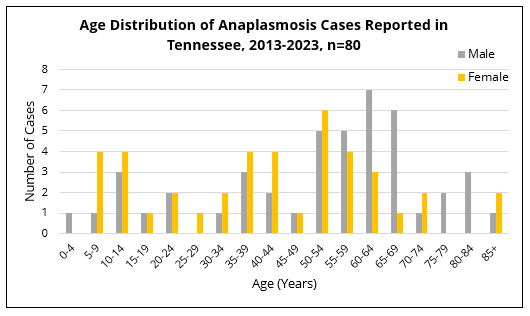
Signs and symptoms of anaplasmosis typically develop within 1-2 weeks after being bitten by an infected tick. Early signs and symptoms (days 1-5) are usually mild or moderate, and they may include:
- Fever and/or chills
- Severe headache
- Muscle aches
- Nausea, vomiting, diarrhea, or loss of appetite
If treatment is delayed or if there are other medical conditions present, anaplasmosis can, in rare cases, cause severe illness. Late stage signs and symptoms can include:
- Respiratory failure
- Bleeding problems
- Organ failure
- Death
For more information, see the CDC Anaplasmosis webpage.
Anaplasmosis is diagnosed by a healthcare provider, who can order blood tests to look for evidence of Anaplasma infection. It may take several weeks for test results to return. If your provider is concerned, they may prescribe you with antibiotics while you wait for the results.
For more information, see the CDC Anaplasmosis webpage.
Other Tick-Borne Diseases
Other tick-borne diseases exist in Tennessee, but are reported too infrequently to draw state-specific conclusions. If you are concerned about one of the following, contact a healthcare provider and refer to CDC resources:
Preventing Bites (Mosquitoes and Ticks)
External link and accessibility notice: Some links on this page take you to websites outside the Tennessee Department of Health (TDH). TDH does not control the content, privacy policies, or accessibility of external sites.
This section provides guidance on how to prevent mosquito and tick bites and reduce the risk of illness.
Preventing Mosquito Bites
Preventing mosquito bites is the best way to reduce risk of mosquito-borne disease.
Know where to expect mosquitoes
All mosquitoes need water to lay eggs and develop. Breeding sites include permanent water (lakes, ponds, swamps), temporary pools from rain or flooding, containers that hold water, and tree holes.
For more information about the water preferences of mosquitoes, visit the CDC Where Mosquitoes Live webpage.
Use insect repellent
Use EPA-registered insect repellents as directed. Effective ingredients include DEET, picaridin, IR3535, oil of lemon eucalyptus (OLE), PMD, and 2-undecanone.
Find the right insect repellent for you by using the EPA insect repellent search tool.
Safety reminders
- Do not use repellent on babies under 2 months
- Do not use OLE or PMD on children under 3 years
- Follow label instructions carefully, especially for children
Wear protective clothing
Wear long sleeves and pants when possible. Treat clothing and gear with 0.5% permethrin or buy pre-treated items. Use mosquito netting over strollers and carriers in high-mosquito areas.
Protect your home and yard
Use window and door screens and keep doors closed. Remove standing water weekly (tires, buckets, planters, toys, birdbaths). Cover rain barrels and storage containers. Fill tree holes so they do not collect water. If you have a septic tank, repair any cracks or gaps. Consider larvicides for water that cannot be drained and adulticides for areas where mosquitoes rest, following label instructions or using a licensed professional.
Travel safely
Research mosquito-borne risks at your destination. If traveling where malaria occurs, ask a healthcare provider about prevention medication. Pack repellent, long clothing, permethrin-treated gear, and mosquito nets if needed.
Preventing Tick Bites and Removing Ticks
The following information provides steps to help prevent tick bites and safely remove ticks, which can reduce the risk of tick-borne diseases.
Know where to expect ticks
Ticks live in grassy, brushy, or wooded areas and may also be carried by animals. Many people encounter ticks in their own yard.
Before you go outdoors
- Treat clothing and gear with permethrin
- Use EPA-registered insect repellents (DEET, picaridin, IR3535, OLE, PMD, or 2-undecanone)
- Follow label instructions and child safety precautions
Workers who spend time outdoors can reference NIOSH Tick-Borne Diseases Workplace Safety guidance.
After you come indoors
- Check clothing and remove ticks
- Tumble dry clothes on high heat for 10 minutes (dry clothes)
- Use hot water if washing first
- Check your body (use a mirror) and check children
- Shower within two hours to reduce Lyme risk and help remove unattached ticks
If you find an attached tick
Remove it immediately with tweezers, close to the skin, and pull straight out. Avoid using bare hands. If possible, note the tick’s appearance. For more information about removing ticks, visit the CDC What to Do After a Tick Bite webpage.
Monitor for illness (rash or fever) in the days and weeks after a bite, and contact a healthcare provider if symptoms occur.
Reduce ticks in your yard
Remove leaf litter, clear tall grass and brush, place gravel or wood chips between lawns and wooded areas, and keep play areas away from vegetation. Consider tick control products or professional services and discourage deer from entering your yard.
Protect pets
Use veterinarian-recommended tick prevention products. Talk with your veterinarian about the best option for your pet. For more information on animals and health, visit the CDC Preventing Ticks on Pets webpage.
Resources for Children: Preventing Tick Bites and Removing Ticks
It is important for children to understand what ticks are, why they can be harmful, where they are commonly found, and how to check their bodies for ticks. This education can begin at a young age and should use materials designed specifically for children.
The following resource from the Centers for Disease Control and Prevention (CDC) can be used in classroom, community, or home settings to help teach Tennessee children about tick prevention and safety.
- CDC Kids’ Tick Prevention Fact Sheet (PDF)
Educational material designed for children that explains how to prevent tick bites and what to do if a tick is found.
This Page Last Updated: March 26, 2026 at 3:42 PM